The U.S. Fumbled Its Early Vaccine Rollout. Will the Biden Administration Put America Back on Track?1/21/2021 On a frigid morning in January, Trudy Ronnel settled into her favorite sofa chair at the Westminster Place senior-living community in Evanston, Ill., pulled down the neckline on her red blouse and braced herself for a shot she’d anticipated for almost a year. At 92 years old, with multiple medical conditions, she spent most of 2020 fearful of contracting the COVID-19 plague that ravaged the world outside her first-floor window. To protect herself, for the past few months she’d avoided Westminster’s communal rooms, which had provided a means to stay active and engaged but risked becoming a pathogenic petri dish. Whenever she left her room, she dutifully wore a surgical face mask and maintained the mandated 6-ft. distance. The most difficult change came in the fall, when visits from her son, daughter and five grandchildren were cut off. Living in relative isolation was not how Ronnel envisioned spending her golden years. Like millions of Americans, as soon as the first coronavirus vaccine was authorized, she began anxiously counting down to the day she’d receive her shot. As an elderly resident of a long-term-care facility, Ronnel is at higher risk of getting infected and experiencing serious symptoms, and thus belongs to one of the first priority groups to get vaccinated, along with health care workers. So, when a Walgreens pharmacist finally appeared in her doorway with the shot on Jan. 6, it came as a welcome sight. After getting the injection, Ronnel allowed herself to feel something that she hadn’t felt since the pandemic first began: the prospect of normality. “I hope this all begins to end soon,” she says. That will depend. TIME spent the past year observing, traveling and speaking with dozens of people involved in the development, distribution and administration of the coronavirus vaccine. A month into the operation it has become clear that health experts, military logisticians and government authorities have often been at odds with one another over miscues, miscommunications and mistrust as they grappled with overcoming a tangle of logistical challenges in building an unprecedented health campaign from scratch. According to local health officials, the Trump Administration’s decision to limit the federal government’s role in administering the vaccines left each state to create its own plans for locally distributing the shots and launching programs for getting them into people’s arms. That already-complicated logistical task, they say, was compounded by a lack of funds and a health care workforce already overwhelmed with COVID-19 testing, contact tracing and pandemic-control campaigns, not to mention mixed messages that left states in the dark about how many doses they could expect, and when. In rolling out the vaccine, the U.S. in many ways repeated the same mistakes it made with COVID-19 testing last spring. Lack of federal leadership first in coordinating distribution of the tests, and later in supporting states to set up and staff testing sites, led to limited access and critical delays in getting results. Public-health officials across the country, as well as many experts TIME spoke with, say there has been a similar lack of coordinated planning and infrastructure to distribute and administer vaccines at the local level. “This vaccination program is complicated, and the way it’s gone so far is a microcosm of the 11 months of failed federal response,” says Dr. Tom Frieden, former director of the Centers for Disease Control and Prevention (CDC) under President Barack Obama. “There has been a lack of organization, a lack of a systemic approach and a lack of a public-health approach coming out of the White House.” The Biden Administration enters office exactly a year into the U.S. pandemic, with the country’s tally of COVID-19 cases at 24 million, along with 400,000 related deaths. Those numbers are only growing. The Administration’s new health leaders will come in with their own ideas for how to control the pandemic and answer the critical question of what went wrong. Their answers won’t simply be a matter of administrative accountability, but a matter of public health and economic urgency. If the current slow pace of getting vaccines from the assembly lines into people’s arms continues, it could lead to weaker population-level protection, enabling the virus to continue spreading–especially with a new, more contagious variant afoot. And the more it spreads, the more likely it is that new, mutant forms will emerge, some of which could be resistant to any hard-won protection from vaccines. Health officials warn that current delays and problems in moving vaccines will only be amplified when tens of millions more Americans become eligible for COVID-19 shots in coming months. Biden’s team has indicated it will erase the brand name Operation Warp Speed (OWS) from the federal vaccine initiative, and introduce a new structure with the immediate goals of vaccinating 100 million people by the 100th day of his presidency while working toward reopening most schools by spring. Getting there will require a more aggressive federal response to support states, the President says, involving the National Guard and the Federal Emergency Management Agency to set up thousands of mass-vaccination centers and mobile teams to reach people living in more remote areas. Whether these efforts will be enough to efficiently immunize hundreds of millions of people in a matter of months will depend on how well the Biden Administration, in contrast to the Trump White House, can persuade the public to trust the science behind the vaccines, and the public-health experts who maintain that until most of the population is vaccinated, the virus will retain the upper hand. 
The only way out of this pandemic, public-health officials say, is to use vaccines to achieve herd immunity, a type of biological fortress in which the vast majority of the population is protected against disease, blocking a roaming virus from finding new human hosts. The U.S. authorized two vaccines in mid-December: the first from Pfizer-BioNTech and the second from Moderna, both roughly 95% effective in protecting against the disease. The government-led effort to develop and test COVID-19 shots stands as a record-setting feat that reduced standard vaccine development time from 10 years to under one (and there are a handful of others currently in testing). But having an authorized vaccine isn’t the same as having a vaccinated public. Getting the shot to some 300 million Americans was never going to be trivial, but Donald Trump’s Administration fell well short of its projections. The Trump team had boasted that by Jan. 1, 2021, some 20 million Americans were expected to be vaccinated against COVID-19. Instead, when the New Year rang in, just 3.5 million people had received the shot. The quest to develop and manufacture a safe and effective vaccine for a new infectious disease was always going to be a gamble, even for pharmaceutical companies with deep experience in mass-producing vaccines. To motivate the industry, the Trump Administration established OWS, a so-called whole-of-America public-private partnership that coordinated pharmaceutical leaders, government health experts and the military to incentivize and pave the way for developing COVID-19 vaccines as quickly as possible. The White House compared the crash program, in its size and scope, to the Manhattan Project, which produced the world’s first atomic bomb that helped end World War II. By the spring, billion-dollar contracts were drawn up to support the research-and-development and manufacturing costs for millions of doses from Moderna, AstraZeneca, Novavax, Sanofi-GlaxoSmithKline and Johnson & Johnson. Pfizer-BioNTech chose not to accept support from OWS to develop its vaccine but signed a nearly $2 billion contract to supply 100 million doses with an option for 500 million more even before its vaccine received federal approval. To lead the group, Trump chose Moncef Slaoui, the former head of research and development for pharmaceutical giant GlaxoSmithKline, who had brought 14 vaccines to market over his career. The creation of a vaccine was just one item on a long list of needs. Inoculation on such a mass scale meant truckloads of supplies had to be located and obtained–little things like glass vials to hold the vaccines, alcohol pads, masks and other personal protective equipment for people giving the shots. To oversee logistics, Trump tapped Gus Perna, a four-star Army general who spent his career working to ensure that soldiers stationed in the world’s most hard-to-reach places were still able to get food, fuel, weapons and supplies. Perna quickly handpicked his staff–the best officers and civilians he’s worked with over the past 37 years–and familiarized himself with the practices, players and perplexing jargon of this new unfamiliar terrain of public health. The national COVID-19 vaccination campaign is an unlikely collaborative effort led by the Department of Health and Human Services (HHS) and the Department of Defense out of a low-rise Brutalist office building in the shadow of the U.S. Capitol in downtown Washington, D.C., where HHS is headquartered. From the start, the military’s regimented, top-down approach clashed with the more casual culture at HHS, particularly at the CDC. Many at the agency had a difficult time understanding why Trump was bringing in soldiers to carry out a core CDC mission: controlling a disease. For decades, the CDC has been managing, without major issues, the Vaccines for Children Program, the country’s largest vaccination initiative–working with manufacturers and distributors to determine supply and storage of more than a dozen childhood immunizations, and collaborating with states to oversee shipment of the shots. Dr. Nancy Messonnier, director of the CDC’s National Center for Immunization and Respiratory Diseases, which researches vaccine-preventable diseases and works with CDC committees to set national policies on any vaccines distributed in the U.S., including childhood immunizations, repeatedly pushed back against the Pentagon’s taking the driver’s seat. She made it clear during conference calls with OWS that she and her team felt it already had a solid vaccine-distribution plan in hand, based on one that had been drawn up to deal with the H1N1 swine-flu pandemic in 2009. But when Perna began establishing daily “battle rhythm” meetings between federal agencies and health-industry leaders to discuss the latest progress or problems with the vaccine program, they were led by HHS and the military, not by CDC, as the agency had done during previous outbreaks. Weekly phone conferences with states, broken into groups by region, were also arranged by OWS to ensure public-health leaders had the latest information and could ask questions. Although CDC had a seat at the table, agency officials felt they were consistently sidelined. (The agency did not respond to requests for comment on this story.) OWS officials determined CDC’s plans were old and not nearly extensive enough to accomplish the mass vaccination they were faced with. In the end, though, OWS contracted with McKesson, a private health care distribution company CDC had used since 2006 to get its childhood vaccines around the country. McKesson subcontracted the work to logistics behemoths such as UPS and FedEx. OWS also created partnerships with pharmacy retailers, such as Walgreens and CVS, to administer vaccines to residents and staff at long-term-care facilities. Overall, OWS has spent nearly $25 billion in federal funding to more than 120 companies to develop, manufacture and deliver vaccines across the nation. Authority under the Defense Production Act was invoked 18 times to mobilize U.S. private-production capacity to manufacture the supplies. Much of the material wasn’t even in the U.S. For example, Goldbelt, an FDA-authorized company that manufactures in China, was granted a $125 million contract to deliver 530 million needles and syringes. The blueprint for the national strategy is represented in a dozen maps and charts Scotch-taped to the walls of Perna’s seventh-floor office at HHS headquarters. And yet, despite the attention to detail and months of strategizing, he acknowledged that success is far from certain. “Our vulnerability will be: we’re too confident,” he tells TIME. “So we have to constantly check ourselves and ensure the plans work and make sense.” 
As the delivery truck snaked its way over Northern California’s interstates and two-lane highways on Dec. 15, a team of distribution analysts in Washington, D.C., watched over nearly every aspect of its journey in real time. They could see the stops the driver took, they knew the weather outside and, most important, they knew the condition of the precious cargo onboard: thousands of doses of COVID-19 vaccine. In the back of the truck, containers packed with vials of Pfizer-BioNTech’s newly authorized vaccine were loaded onto customized trays, resembling small pizza boxes, each container carrying at least 975 doses. The containers were also packed with dry ice, tracking devices and sensors, which enabled the team to watch as the temperatures of two of the trays–one destined for Napa, Calif., the other to Sonora, Calif.–plunged to –133.6°F, more than 21° below the accepted threshold. A call was made to the truck driver to stop and keep the trays in the vehicle. Thousands of doses of vaccines made by Pfizer-BioNTech and Moderna have been wasted since shipments began in early December, according to government officials. The reasons vary–sometimes doctors inadvertently leave vials out too long; sometimes the day ends with doses that were supposed to be administered left over because patients never showed–but several deliveries have encountered temperature problems. If the doses deviate from their target destination in each of the nearly 42,000 U.S. ZIP codes, or if the temperature of the vials exceeds –76°F (–60°C) or falls below –112°F (–80°C), officials at Pfizer-BioNTech and the government are immediately alerted. “We want to see everything,” says Marion Whicker, who spent decades moving tanks and armored vehicles around war zones for the Army and now serves as OWS’s head of logistics for vaccine distribution. “Just like you track your Christmas gift from Amazon.” The information streams into the Vaccine Operations Center, known as the VOC. The windowless, conference-hall-size command hub at HHS headquarters is where uniformed military members, HHS officials, private contractors and U.S. marshals keep a watchful eye over logistics. On the operations floor, dozens of analysts work behind rows of computer monitors. Along the far wall in front of them, four large flat screens glow with real-time information about the day’s deliveries, which enables them to track shipments from manufacturing facilities to their destinations across the nation. But once the vaccine vials leave OWS’s hands, the daunting task of distributing the shots to the people who need them falls to the states. Already facing shrinking budgets and overwhelmed by the demands of managing the pandemic over the past year, state public-health departments have struggled with the additional obligation to distribute and administer vaccines. Last fall, the CDC asked every state health department and jurisdiction the agency supports for a plan; most were vague by necessity and in some cases relied too heavily on existing programs and call centers designed for childhood-immunization programs, but which may not have been robust enough to handle COVID-19. “They underestimated the uniqueness of vaccinating 30% of Americans in a few months,” says Joshua Walker, co-founder of Nomi Health, which helped the health departments of Iowa, Florida, Nebraska and Utah set up COVID-19 testing programs and is now supporting dozens of cities, counties, states, hospitals, airports, hotels and other groups to quickly manage vaccination programs. In addition, many states found that initial federal funding for COVID-19-related response wasn’t adequate, making it hard to form concrete plans to buy the ultra-cold freezers needed to store the Pfizer-BioNTech vaccine, for example, or to hire staff for vaccination clinics. Funding for COVID-19 response authorized by Congress last spring expired at the end of the year, says Dr. Jinlene Chan, acting deputy secretary for public health services for the Maryland department of health, and “we had no anticipation of any additional dollars of support for all of these efforts.” As the number of cases in her state started to climb, and to ensure that citizens would get vaccinated, Chan says, other pandemic-related efforts, like the depth of the contact-tracing interviews, had to be temporarily scaled back to prioritize vaccination. As Kris Ehresmann, director of infectious disease at the Minnesota department of health, puts it, “We got an amazing vaccine, the Cadillac of vaccines, and yet we’re skimping on resources for getting it out.” New funding to support state COVID-19 programs was authorized only in the last days of 2020. On the weekly calls, Perna and Slaoui informed state health officials that the federal government would get them the vaccine but that it was up to them to work with the CDC in order to form and execute “last mile” inoculation plans. “We’re solving problems ahead of execution,” Perna said on one call, observed by TIME in early December. “Does this mean perfection? No. The plan is only good to get you started. What’s important is the open collaboration and communication between everyone.” To keep track, a government contractor developed a new software platform called Tiberius, which enables states and federal agencies to see their orders and track vaccine shipments. After vaccine producers say how many doses are available for distribution in the upcoming week, each state then has the opportunity to place an order up to a certain amount allocated by OWS. Once approved, that order is locked into Tiberius every Tuesday. Even with the system, states at first complained they didn’t know exactly how many doses they could expect. Some say they expected a certain amount based on what the federal government had told them (which Perna says were based on rough population-based estimates) only to find out just the day before delivery–or sometimes on the delivery day itself–that they’d be getting fewer than anticipated. That made it nearly impossible to adequately plan vaccination campaigns. Dr. Eric Dickson, CEO of Massachusetts’ UMass Memorial Health Care, says his hospital system received half the number of doses it expected during the first two weeks of vaccinations, which led to “vaccine envy” among staff members who could not get vaccinated along with their colleagues. Though the situation has improved since then, Dickson says communication from the federal government was sorely lacking at first. “It could have been a lot better than going to the loading dock with the FedEx guy and saying, ‘How many did we get?'” 


The COVID-19 vaccines authorized so far, from Pfizer-BioNTech and Moderna, require two shots spaced about a month apart. In the initial push, OWS sent out the first dose but held back a reserve of second doses, because Perna did not want to be caught shorthanded if manufacturing faltered and supply dried up. Vaccinemakers, however, have proved their reliability. A steady stream of more than 4 million doses were available for distribution for each of the past three weeks. Because of that, on Jan. 8, Biden’s team announced that it planned to release nearly all available vaccines in order to inoculate as many people as possible, rather than hold vaccines back to ensure that anyone who received a first dose would get the second one. It didn’t take long before the Trump Administration said it would adopt this immediate distribution system–but states expecting an additional windfall of vaccines were frustrated to learn on Jan. 15 that the government did not in fact have vaccines on reserve to release. The discovery was neither the first nor the last disappointment states would face as the rollout unfolded. Amid the chaos and confusion, many states simply aren’t administering the shots delivered to them. Though the pace is picking up, CDC data published Jan. 19 show only about 15.7 million doses have been administered, out of 31.1 million delivered to the states. Some of the shortfall may be a reporting lag as states learn new tracking systems. Another possible factor is winter storms delaying some deliveries and forcing office closures. But it’s clear there are entrenched problems. States don’t have the staff or infrastructure to manage the volume. When Florida’s Miami-Dade County opened up 2,000 or so vaccination appointments, they were gone in under a minute as 80,000 people slammed the reservation site during those 60 seconds. Believing that their existing childhood-vaccination programs could handle the load, many states failed to fully account for the overwhelming demand from a desperate and impatient public. County health offices around the country are inundated daily with phone calls from residents bewildered by the mixed messages from federal, state and local officials. Vaccine eligibility requirements have contributed to that confusion. Though the CDC provides recommendations about who should get the shots first, states make their own rules. For example, New York began vaccinating all people over age 65 on Jan. 11, while in Maryland, that group is set to gain eligibility on Jan. 25. Such differences are causing potentially dangerous confusion that could lead some to miss their opportunity for a shot or decide not to get one at all. Making matters worse, once a vial (which contains at least five doses in the case of the Pfizer-BioNTech vaccine and 10 doses in the case of Moderna) is opened, it needs to be used within six hours or discarded. As a result, in situations where someone changes their mind about getting vaccinated or misses an appointment, nurses, doctors or pharmacists, holding doses that would otherwise go to waste, are deciding to give them to anyone who happens to be around–regardless of whether they are in the right priority group. This, in some cases, has become regional policy; Michigan’s chief medical executive, Dr. Joneigh Khaldun, says she has told providers to aim to use 90% of their vaccine supplies within seven days of receiving them, even if that means straying from state guidelines in “a good-faith effort to use the vaccine.” The lack of federal leadership has resulted in state health departments scrambling to figure out solutions, creating a patchwork approach to allocating and administering allotted doses. Health officials in Florida decided to offer a number of vaccines through Eventbrite, a website primarily known for obtaining tickets to sports events, concerts and even monster-truck shows. In southwest Florida’s Lee County, officials decided against building an appointment-based system, so senior residents instead had to spend more than seven hours, some overnight, in line, hoping to snag one of the limited vaccines available. “It’s only now that the states are starting to realize the gravity of the situation and the volume required to vaccinate their populations,” says Dr. Peter Hotez, a vaccine scientist from Baylor College of Medicine in Texas. Given the diverse population and topography of the U.S., and the differences from state to state, local health departments are trying to come up with creative and flexible strategies to reach people in as short a period of time as possible. In Alaska, for example, health workers have been taking planes, boats and sleds to reach the 80% of the state’s communities living in places that cannot be accessed by road, and setting up makeshift clinics inside bush planes or going door-to-door in villages to vaccinate Indigenous communities. And because of the travel challenges, the state requested and now receives its allotments for these groups from the Indian Health Service (IHS) monthly rather than every other week, so doctors and nurses can plan in advance, and distribute and use the vaccines more efficiently. In Carlton County, Minnesota, health officials plan to rely on drive-through vaccination clinics to make the process more convenient. After months of planning, the county’s drive-through clinic opened for two days in December to vaccinate first responders; the health team plans to reopen it soon, along with a number of other drive-through locations, to accommodate all of the county’s residents when it’s their turn to get the shots. “The drive-through model allows us to potentially vaccinate thousands of people in a day,” says Ali Mueller, emergency-preparedness coordinator for the county. Other states have taken similar approaches, such as converting professional sports stadiums into mass-vaccination sites, some of which operate 24/7. Carlton County also worked with Redlands, Calif.–based Esri, a geographical information systems software company, to set up a tracking tool that offers real-time information on the ebb and flow of people through the county’s drive-through clinic. In theory, that will help Carlton’s health team anticipate what times of day demand will likely be highest at their next clinics, so they know ahead of time how many vaccines they will need and thus don’t waste any doses. Many other states and counties are working with similar companies to build software to manage the higher demand and to answer people’s questions about where and when they can get vaccinated. Without solutions to such challenges, the national vaccination effort will only grow more difficult in the coming weeks. After all, health care workers and long-term-care residents are both fixed populations that are relatively easy to locate; when vaccines are opened up to everyone in the country, things could rapidly deteriorate into an even more chaotic state than they are in today. 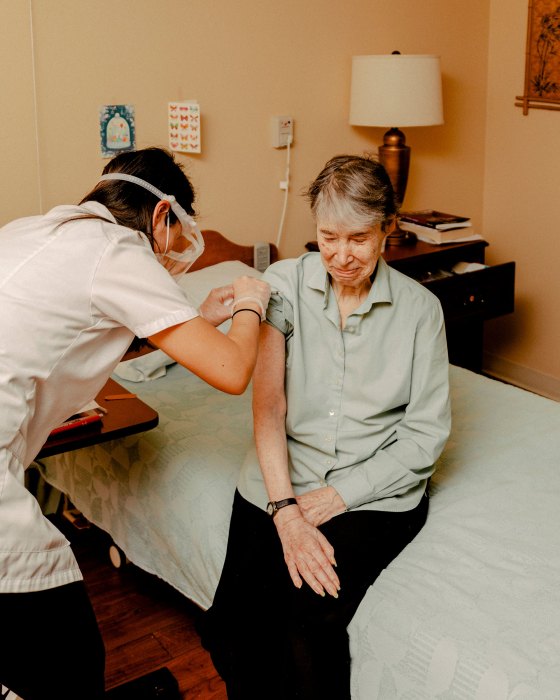
It’s difficult to say whether this is a uniquely American problem. Some countries, such as Israel and the United Arab Emirates, have outpaced the U.S. in vaccinating more people out of every 100–about 32 and 20, respectively, compared with less than five in the U.S. In Israel, that success can be traced to a combination of centralized vaccination programs and saturated messaging campaigns to educate people about the public-health benefits of vaccines and encourage them to get immunized. In contrast, rollouts in European countries have been slower, partly because the E.U.’s regulatory agency lagged behind both the U.S. and the U.K. in authorizing the first shots. What we do know is that vaccinating the general public in the U.S. will take more of everything that has been in short supply during the first phases of rollout: vaccines themselves, storage for those doses, facilities that can accommodate mass vaccine clinics, staff or volunteers to run them, and communication with people who will ultimately receive the shots. More doses are on the way. Not only are Pfizer-BioNTech and Moderna perfecting their manufacturing and distribution systems, but other vaccine candidates are moving closer to emergency-use authorization, perhaps getting the green light as early as next month. The crucial challenge will be ensuring that as supply ramps up, so too does the machinery of vaccination. While each state has its own challenges and considerations to make, the federal government can even the playing field by ensuring each one has the resources and information required to implement a system that works at the local level. To actually turn vaccines into vaccinations, states also need support and transparency from the federal government; enough money to furnish a robust network of well-staffed public vaccination centers; and coherent public-information campaigns, both for building trust in COVID-19 vaccines and for conveying who is eligible to get vaccinated, when and where. Biden plans to address those weaknesses and change the current pace of the U.S. vaccination program. “The vaccine rollout in the United States has been a dismal failure, thus far,” he said in a Jan. 15 speech. He’s already asked Slaoui to submit a letter of resignation from leading OWS scientific development. Internally, officials with OWS expect further personnel changes in the weeks to come, although–for the time being–the Biden team plans to keep Perna in his current role. Meanwhile, Biden’s proposed plan does indeed give the federal government a more central role in ending the pandemic, which includes establishing more federally funded and operated vaccination sites. “On my first day in office,” he said, “I’ll instruct the Federal Emergency Management Agency, FEMA, to begin setting up the first of these centers,” he said in that speech. He set a goal of standing up 100 such sites by the end of his first month in office. To get this done, Biden has proposed a coronavirus-relief package that calls for at least $20 billion for vaccine distribution and additional funds to support the hiring of 100,000 public-health workers. If approved by Congress, that could significantly relieve the burden on cash-strapped states with exhausted health care workforces. Biden has also promised “a massive public-education campaign” to address another major roadblock in the quick administration of vaccines: rebuilding trust among people who have been hardest hit by the pandemic, in racial and ethnic minority groups including Black, Latinx and Indigenous Americans. As the rollout continues, more vaccines are administered each week, and many states are falling into a rhythm of knowing how many vaccines to expect on a regular basis. But each day the demand far exceeds the supply of shots is a day the virus can gain the upper hand by infecting more people, sending them to the hospital or contributing to their deaths. Vaccines can lead us to the end of the pandemic, but only if we find a way to move them more efficiently from the government’s hands and into the arms of Americans. With reporting by Alejandro de la Garza, Simmone Shah and Leslie Dickstein from https://ift.tt/393X0xf Check out https://takiaisfobia.blogspot.com/
0 Comments
Dr. Jacqueline Parchem, a maternal-fetal medicine physician at UTHealth in Houston, considers herself a private person. Even still, she logged on to Twitter on Dec. 22 and began drafting a series of posts. “Pregnant and unsure about the #COVID19 vaccine?” she wrote in a tweet that has now been liked more than 3,000 times. “You’re not alone. Got vaccinated today at 31 weeks [pregnant] and feel very fortunate. But it’s complicated.” Over the course of nine tweets, Parchem broke down the thinking that went into her difficult decision to get vaccinated during pregnancy. Ultimately, she wrote, she decided her substantial risk of being exposed to COVID-19 while caring for patients outweighed any hypothetical risks associated with the vaccine—but the choice wasn’t easy. There are virtually no data on how COVID-19 vaccines affect pregnant people and their fetuses, since vaccine makers—like many companies testing a new drug—enrolled only non-pregnant adults in their clinical trials. Plus, the two vaccines authorized so far in the U.S., those made by Moderna and Pfizer-BioNTech, are the first widely available shots to use mRNA technology, so there is little frame of reference as to how they might affect pregnant people. Moderna reportedly found no safety concerns after testing its shot in rats prior to or during pregnancy, but animal data only reveal so much. While the mRNA technology used in Pfizer-BioNTech and Moderna’s shots hasn’t been tested on pregnant people, the U.S. Centers for Disease Control and Prevention (CDC) says “they are unlikely to pose a significant risk for people who are pregnant.” The vaccines do not contain live virus, which means they cannot infect the recipient with COVID-19, and they do not enter the part of the cell that holds DNA. Still, without strong data, most U.S. health groups have essentially left the decision about whether to get vaccinated while pregnant—or while breastfeeding or trying to get pregnant—up to individuals. The CDC, the American College of Obstetricians and Gynecologists and the Society for Maternal-Fetal Medicine (of which Parchem is a member) say pregnant people should not be excluded from vaccination if they are otherwise eligible to get their shots, but they do not explicitly make a recommendation one way or the other. In the U.K., however, health authorities have specifically stated that “those who are pregnant should not routinely have this vaccine,” though people at particularly high risk of COVID-19 exposure may choose to get it. That pregnant people in the U.S. haven’t been excluded from vaccination is “great, but it doesn’t answer the question, ‘Should I get the vaccine?’” Parchem says. Experts saw this dilemma coming. Even though millions of people in the U.S. alone give birth each year, pregnant people are frequently excluded from drug trials, in part due to understandable concerns about exposing unborn babies to potentially harmful substances. The legacies of drugs that were proven to be dangerous for pregnant people and their fetuses—including the anti-nausea medication thalidomide and the synthetic hormone diethylstilbestrol—after approval still loom large. Pregnant people have historically been considered a “vulnerable” population—a designation also applied to groups, such as children and the incarcerated, who may be coerced into participating in research. OB/GYN and author Dr. Jen Gunter says that label was never appropriate for pregnant people, who are “more medically complex, for sure,” but are perfectly capable of deciding whether or not to enroll in a study. The medical community is increasingly moving away from using the “vulnerable” label for pregnant people, but pharmaceutical companies must still take certain precautions when designing study protocols that include expectant mothers. Many simply choose not to—especially in situations, like developing COVID-19 vaccines, where speed is crucial. One study found that, out of 468 drugs approved by the U.S. Food and Drug Administration from 1980 to 2000, more than 90% came with no conclusive information about their risk of birth defects. As a maternal-fetal medicine specialist, helping pregnant people navigate this dearth of research was part of Parchem’s job even before the pandemic. Taking drugs often presents a moral quandary for pregnant people, she says, since medications are rarely tested for use among that population. “Naturally, people tend to center on the fetal risk,” Parchem says. But she says it’s also important to consider “the consequence of not getting this treatment” for the mother. In the case of COVID-19, that could include severe illness or death. Pregnant people who get COVID-19 are at increased risk of requiring intensive care, studies show, and they may also be at risk of complications including preterm birth. Faced with that calculus, many other pregnant health care workers have chosen to get vaccinated. Dr. Leslie Kim, a facial plastic surgeon at the Ohio State University Wexner Medical Center, in early January posted on Twitter and Instagram about her decision to get vaccinated at 32 weeks pregnant. After speaking with her own doctor, Kim, who regularly performs procedures on or near patients’ airways, decided her risk of exposure to COVID-19 was high enough to justify getting vaccinated. Kim also felt a responsibility to add, in however small a way, to the public’s understanding of vaccination during pregnancy. “For pregnant people to be included in studies, they do have to volunteer,” Kim says. “All of us who are stepping forward…[are] contributing to the science of this vaccine.” While formal studies on COVID-19 vaccines and pregnancy have not yet been completed, Kim says she hopes others in her position are “diligently reporting side effects or anything we experience so we can help future people in our shoes.” For Dr. Denise Cardenal, an OB/GYN affiliated with OB Hospitalist Group in St. Lucie, Fla., the desire to protect her family and community from COVID-19 provided motivation not only to get vaccinated at 31 weeks pregnant, but also to post about the decision on Facebook. “I’m not one to share anything about what I do as a physician on Facebook,” she says. But “I saw this as such an important opportunity to set an example.” Already, she says, she’s heard from people who have decided to get vaccinated because she did. Still, Cardenal emphasizes that the decision is a personal one. Someone who can stay home throughout her pregnancy may want to wait to get vaccinated until after she gives birth, whereas someone with a higher exposure risk may not. Each individual should talk to their doctor and read up on health groups’ guidance before making a choice, she says. “People should question the data, the science, what is out there. You have to inform yourself,” Cardenal says. Hearing from health care workers who have chosen to get vaccinated can be part of that. Until there are published clinical trial results, the best information about COVID-19 vaccines and pregnancy may indeed come from people choosing to share their private decisions publicly. “We don’t want to make any decisions by a [sample size] of one,” Gunter says, “but people stepping up is really an amazing service.” from https://ift.tt/2NqTq8f Check out https://takiaisfobia.blogspot.com/ Heres What Joe Biden Can Do About the COVID-19 Pandemic Starting On His First Day as U.S. President1/20/2021 Every pandemic starts as a squall—a localized disturbance in a single city or town, causing all manner of problems there, but sparing the larger world outside. Squalls become storms, however, and storms become tempests and before long the entire world is being lashed by winds of disease and death that no one saw coming just a few months before. As President Joe Biden takes office, he is facing nothing short of a pathogenic typhoon, with COVID-19 raging around the world, nowhere more so than in the U.S., with some 24 million cases and 400,000 deaths—more than 20% of the global toll. If the pandemic unfolded in stages so too must it be contained that way. During the campaign, Biden promised swift action on such steps as testing, vaccine manufacture and distribution, and preventive measures like mask mandates. That, he’s said, will be followed by other steps like improving surveillance of emerging variants of SARS-CoV-2, extending unemployment benefits to people whose jobs were lost as a result of quarantining and lockdowns, extending the moratorium on evictions, and ensuring that people who contract COVID-19 and survive don’t face discrimination in insurance benefits. It would, the candidate promised, be nothing short of a stepwise, war-like mobilization. Less than a week before his inauguration, Biden unveiled a massive $1.9 trillion plan, proposing short-term, medium-term and long-term fixes intended to bring the current rate of infection and death under control and set the U.S. up for a sustainable recovery from both COVID-19 and the economic devastation it has wrought, in the coming year and beyond. The proposed bill is a shaggy thing—equal part hit list and wish list, containing long-hoped-for Democratic goals like increasing child tax credits and boosting support for pre-K childcare and public transportation, most of which are likely to face GOP pushback in a closely divided House and a 50-50 Senate. But much of the rest is precisely targeted to meet the current crisis and then build on that hoped-for success. That kind of focus can’t come too soon. “We are inheriting a situation that could politely be said to have been neglected,” says an incoming Biden official working on COVID-19 response. “There’s been no plan in place for the country even for 2020, never mind 2021 or 2022.” Here is what the Day One priorities for the new Administration look like and some of the steps that will follow them. Starting on day oneThe president’s most conspicuous and sound-bite-friendly pledge is to launch his recovery program by vaccinating 100 million Americans within the first 100 days of his Administration. It’s achievable, but only if the right pieces fall into place. The first, of course, is getting the vaccines manufactured, which may call for invoking the Defense Production Act (DPA)—a step the president can take by executive order before the sun even sets on inauguration day—requiring industry to accept and prioritize government contracts to ramp up production fast. The Administration also plans to lean on states both to expand and make uniform the categories of people who are eligible to receive the shots, including all people 65 and older—who currently are eligible in some states but not others—and front-line workers who are not necessarily medical workers, like transit, pharmacy and grocery employees. That could not come with a first-day order, but Biden can impose first-day pressure. Even if he doesn’t enjoy much of a new-president honeymoon, it could be hard for governors to make the case that their seniors and front-line workers don’t deserve extra protection. Implemented well, both the production and eligibility steps could help the U.S. not only meet the president’s target, but actually exceed it, especially if, as expected, the Johnson & Johnson and AstraZeneca vaccines are soon approved, joining the Moderna and Pfizer-BioNTech shots in the vaccine arsenal. “Getting the vaccine rollout to at least one million a day is what the president promised,” says Dr. Leana Wen, an emergency physician and public health professor at George Washington University, and previously Baltimore’s Health Commissioner. Even then, of course, it would take 328 days to vaccinate 328 million Americans—and that is just the first shot. “Working up to at least three million a day is going to be critical,” says Wen. As yet, the Biden Administration has not laid out a clear plan for how to triple the already ambitious 100-day target. Still, a steady and predictable flow of vaccines could help address a vexing problem that’s occurring now, with hospitals and clinics holding back shots, keeping them in stock for fear that if they administer all of their initial supply at once, they’ll have nothing left when people return for their second dose three or four weeks later. “We should have people putting those vaccines in arms the moment they can,” says Dr. Howard Forman, professor of public health and management at Yale University and a practicing physician. “I should have confidence in my supply chain like I do in FedEx. And I don’t mean FedEx ground; I mean 99.99% certainty that I’m getting it tomorrow.” Of course, just having vaccines on hand is not enough if there aren’t the necessary resources to administer them. Within one month of taking office, Biden thus envisions establishing a network of federally funded vaccination centers across the country in places that are both easily accessible and able to accommodate large numbers of people, like stadiums, school gymnasiums and community centers. That would be another Day One move: “On my first day in office, I will instruct the Federal Emergency Management Agency, FEMA, to begin setting up the first of these centers,” Biden said in a Jan. 15 address to the nation unveiling his $1.9 trillion plan. Mobile vaccination clinics, which can also come via Day One order, would help bring the vaccines to people, rather than requiring people—some of whom are sick or elderly or otherwise less able to travel—to come to the vaccines. A standing army of up to 100,000 health workers will be recruited to help with such work as vaccine outreach and contact tracing. “So much of that infrastructure should have been in place months ago, but it is not,” Wen says. Then too, there is the immediate business of prevention, testing, and health care worker protection. On his first day in office, Biden can sign an executive order he has announced that will require masking by federal employees on federal property, as well by all people on busses, trains and planes traveling across state lines. He has also pledged to double the number of drive-through testing sites across the country and to use the DPA to increase the availability of personal protective equipment in hospitals and other health care settings. Finally within the first 100 days, Biden promises to reopen schools nationwide, providing federal funding to help improve sanitation and make social distancing possible—with barriers between desks say, or tenting for outdoor learning. None of this is cheap and Biden doesn’t pretend it is. Reopening schools will cost up to $170 billion; testing and vaccine rollout will be another $160 billion; manufacturing necessary PPE will cost another $30 billion—all of which was spelled out in a document the transition team released along with the announcement of the overall plan. “In this moment of crisis, with interest rates at historic lows, we cannot afford inaction,” Biden said in a Jan. 14 address to the nation. “I know what I just described will not come cheaply, but failure to do so will cost us dearly.” Other steps will not be nearly as hard on the federal purse. Biden plans to sign another executive order, in his first few days in office, committing the U.S. to rejoining the World Health Organization and plans to relaunch the United States Agency for International Development’s (USAID) pathogen-tracking program to help detect emerging viruses and strains. Both steps will help restore the U.S.’s place as a global health leader. Plans for the mid-termCash is at the center of another tranche of Biden plans—targeted at the economy, which has contracted its own pandemic-related illness. Making good on a campaign pledge, the president is calling for an additional payment of $1,400 to individuals earning up to $75,000 per year or couples earning $150,000, which will add to what Biden calls the $600 “downpayment” on stimulus money taxpayers received in the relief package passed in the final weeks of the Trump administration. He also hopes to extend unemployment benefits through the end of 2021, add an additional $400 per week in unemployment supplement payments and extend emergency paid sick leave through Sept. 30. The existing moratorium on evictions would be extended to the same date and Biden seeks $25 billion in rental assistance to keep people in their homes after the protections lapse, plus $5 billion to provide housing for people already rendered homeless by the pandemic. This, the Biden team argues, is both a public and moral imperative. “I don’t think that there’s an argument that a public health crisis doesn’t require a good safety net,” says the Administration official. “If you’re going to ask for sacrifices of your citizenry like the ones we’ve seen in the last year, you’re going to have to let them know that there’s a country looking out for them.” Messaging—which costs little or nothing at all—will be important too. Biden has promised transparency in communicating about the virus and the outlook for national recovery and has regularly offered hard facts to a public already suffering from pandemic fatigue. “Truthfully, we remain in a very dark winter,” he said in his Jan. 15 address. “The honest truth is, things will get worse before they get better.” A release from the Biden transition team explicitly promised “a federally led, locally focused public education campaign that will build public trust through increased transparency, communication around progress and setbacks, and a public education campaign that addresses vaccine hesitancy and is tailored to meet the needs of local communities.” That’s important as far as it goes, but the plan is vague on who will do the messaging—and it can’t all come from Biden alone. Forman sees a place for all manner of public figures to help sell the safety and efficacy of vaccines and explain the challenges the nation still faces. “The messaging piece may have to include more celebrity endorsements of vaccines,” he says. “It may have to include more community connections with religious leaders, ministers and so on.” Wen sees a similar role for expected sources like the Centers for Disease Control and Prevention—whose credibility was tarnished during the Trump years due to excessive politicization on topics like climate change and, later, the efficacy of mask wearing—as well as for less expected sources like corporate figures. “Business leaders and CEOs will be critical because of the unfortunate narrative that somehow the choice is between public health and the economy,” she says. “They will be key messengers.” What Biden should do down the lineIf the Biden plan has a weakness, it’s in the challenges some of its longer-term provisions are likely to face on Capitol Hill. Many of those proposals involve the progressive goodies that are likely to run into Republican resistance—$20 billion in aid for public transit, $13 billion in federal nutrition assistance programs; aid to states in funding Supplemental Nutrition Assistance Program (SNAP) benefits; increasing the child tax credit to $3,000 per child. While the plans may have tangible benefits in a time of economic suffering, they are less directly linked to the pandemic than the rest of the proposal is. More important downstream effects will come from long-term implementation of programs to track mutations of the COVID-19 virus and to conduct surveillance of the next virus to jump species from animal to human as SARS-CoV-2 did. That, says the Administration source, is why re-engaging with the WHO and relaunching the USAID’s pathogen-tracking program is so important. “I think rejoining the world is a critical first step,” he says. “Being at the table and having an ability to share knowledge, whether it’s a new strain, a new virus, is important. This is not a uniquely American problem.” An additional long-term issue the Biden team plans to address is eliminating health inequities in both treating and preventing COVID-19. Black, Latino and Indigenous American communities are being infected at roughly four times the rate of whites and dying at three times the rate, as Biden pointed out in his Jan. 15 address. “We have seen health disparities unveiled and unmasked,” Wen says. “We have seen that, once again, it’s those who are most disadvantaged and the most vulnerable who suffer the most.” Vice President Kamala Harris has proposed a COVID-19 Racial and Ethnic Disparities Task Force to ensure health equity in dealing with the crisis, and further proposes converting the body to a permanent Infectious Disease Racial Disparities Task Force after the pandemic is over. The proposal—which was featured conspicuously during the campaign—does not, however, appear as part of the $1.9 trillion plan, though the plan does mention health disparities repeatedly and they are framed as central to the president’s thinking. If there’s a certainty in exactly how the Biden plan will unfold over the next 24 or 12 or even three months, it’s that there’s no certainty at all. Viruses are at once both mindless and clever—infecting and eluding, spreading and shape-shifting. It takes a set of policies that are equally adaptable, equally nimble to defeat them. The new president’s plan is an ambitious first step. A lot of sure-footed steps remain before the pandemic is defeated. from https://ift.tt/2KC8sac Check out https://takiaisfobia.blogspot.com/ In coming years, families around the world will be reminded of what happened in January 2021 by gaps in photo albums, saved video chats or text message threads, and in some cases, tragically, empty seats at future weddings. But in the history books, the pandemic’s impact will be traced in terms of milestones, including one passed on Friday: 2 million people have died from the COVID-19 pandemic, according to the Johns Hopkins Coronavirus Resource Center. The novel coronavirus has caused the deadliest global epidemic since the emergence of HIV/AIDS 40 years ago, and the deadliest respiratory pandemic in a century. Worldwide, some 12,000 to 13,000 people have died from COVID-19 every day over the past week. Deaths have been increasing steadily since October, when about 5,500 people were dying per day globally. The staggering number of deaths from COVID-19 intensifies the urgency of global efforts to distribute coronavirus vaccines. In the U.S. and other countries, efforts to distribute the vaccine have been hampered by supply chain limitations and other logistical problems. The World Health Organization has repeatedly warned that distributing vaccines equitably across counties will be necessary to stop the spread of the pandemic, although 95% of the vaccines distributed so far have been handed out in just 10 countries, Dr. Hans Henri P. Kluge, WHO Regional Director for Europe, said Thursday. Newly discovered mutations of the virus, including the variant initially found in the U.K., and since spread to multiple countries including the U.S. threaten to drive the death toll up even higher; the U.K. variant is thought to spread 70% more quickly, which could lead more vulnerable people to becoming infected. More U.S. resident have died after contracting COVID-19 than in any other country. Over 389,000 Americans have died from the virus, followed by Brazil, with more than 207,000 deaths, and India, with nearly 152,000. The U.S. also leads the world by number of reported infections; more than 23.3 million people have been infected with the virus. COVID-19 was likely the third-leading cause of death in the U.S. in 2020; when preliminary numbers from last year are compared to 2018, they suggest more U.S. residents died from COVID-19 in 2020 than from strokes, accidents or Alzheimer’s disease. Achieving herd immunity to protect people from COVID-19 through vaccination is still a long way off. In the U.S., less than 3% of the population has been vaccinated so far, while experts estimate that at least 75% of people would need to be vaccinated to achieve herd immunity. Therefore, stopping more deaths from COVID-19 in the coming weeks will require individuals to keep taking the steps experts say are needed to stop the virus’ spread: staying home, wearing masks, and maintaining physical distance from one another. from https://ift.tt/3oNhFep Check out https://takiaisfobia.blogspot.com/ Israel, which has already vaccinated more than 2 million of its citizens, is ramping up COVID-19 shots to 250,000 per day, meaning most Israelis over the age of 16 are on track to have two doses by the end of February. But even as the country wins plaudits for the world-leading pace of its vaccine rollout, its government is facing rising criticism for excluding millions of Palestinians from the program. Some 75% of citizens over the age of 60 have been inoculated so far, including Palestinian (or “Arab Israeli”) citizens of Israel and occupied East Jerusalem, and Israelis living in illegal West Bank settlements. Not included, however, are more than 4.5 million Palestinians living under Israel’s direct or indirect military control in the West Bank and Gaza. Gerard Rockenshlaub, the head of the World Health Organization Office for the occupied Palestinian territory told TIME on Jan 13 that “unequal access to essential vaccines is hardly anywhere as visible as it is in this particular context.” Israel has a “duty” to vaccinate Palestinians, the Palestinian Authority said in a statement it released on Jan 10. Not doing so constitutes “racial discrimination against the Palestinian people and a denial of their right to healthcare.” In a Jan. 14 statement, The UN’s body for human rights also called on Israel to ensure swift and equitable access to the COVID-19 vaccine for the Palestinian people, in accordance with its responsibilities as an occupying power under the Geneva Convention. Israel’s successful vaccination rollout can be credited to a combination of its small size, its strong public healthcare system, and its early acquisition of vaccines. But critics also point to the fact that Prime Minister Benjamin Netanyahu—who is facing a criminal trial on three criminal charges and months of protests over his handling of the economy—is in dire need of a political win ahead of an unprecedented fourth election in two years slated to take place in March. Here’s what to know about Israel’s vaccination program, and how its reputation—and efficacy—could be undone if Palestinians are not inoculated too: Why has Israel’s vaccination rollout been so successful?As of Jan. 14, more than 20% of Israeli citizens had been given the shot. The UAE came in next at around 10%, of its population, while the U.K., the U.S., and Denmark all hovered around the 2% mark. Vaccine hesitant countries like France, where surveys indicate that only 40% of people intend to get the jab, are far further behind. Vaccine hesitancy based on misinformation and conspiracy theories was also an issue in Israel. But the Health Ministry’s multi-channel public information campaign—including Netanyahu receiving the country’s first shot on live television—and outreach to minority community leaders such as Ultra-Orthodox rabbis helped create a consensus, says the Chief Medical Officer for the Israel Defence Forces (IDF) Col. Dr. Tomer Koler. “In the end, I think all the groups will be vaccinated because they want to be,” he tells TIME. Collaboration between the military and Israel’s strong public healthcare system is another factor in the efficiency of Israel’s COVID-19 response, Koler says. “The IDF and the medical corps and the homefront command are intertwined with civilian life in Israel,” he says, adding that the IDF called up and trained 700 reservist medics to support the government-funded healthcare providers with the program. Israel’s small geographical size--barely bigger than New Jersey by pre-1967 borders—helps too when it comes to transporting the Pfizer shot, which has to be kept at minus 75 degrees Celsius (about minus 103 degrees Fahrenheit). How did Israel get so many vaccines so quickly?That’s down to a deal Israel’s government struck with U.S. pharmaceutical giant Pfizer, Netanyahu revealed on Jan. 7. Under the deal, Israel gets 10 million doses of the BioNtech-Pfizer vaccine in return for sharing anonymized biometric data on who receives it and how it affects them, Politico reports. Israel’s public broadcaster also reported that its government paid more than other countries for BioNtech-Pfizer and Moderna vaccines—at an average of $47 per person for the two-dose inoculation. The Washington Post reported in December that the US was paying Pfizer/BioNTech $19.50 per dose while the EU was paying $14.76. Despite Israel’s economic woes, the reported premium has drawn scant pushback. ”Maybe it was more expensive, but it was worth paying for,” says lawmaker Nitzan Horowitz, leader of Israel’s left-wing Meretz party, “I think that is something we all agree on.” Where Horowitz does disagree, is on Israel’s responsibilities: vaccinating Palestinians in the West Bank after Israelis is “our moral obligation,” he says. Israeli rights organization Rabbis for Human Rights has similarly argued that Israel has a “moral imperative” to vaccinate Palestinians, especially in Gaza. Does Israel have a responsibility to inoculate Palestinians?According to the U.N., it does. Israel first occupied the West Bank and Gaza during the war with its Arab neighbors in 1967. Its military withdrew from the Gaza Strip in 2005—which has since 2007 been governed by the militant group Hamas—but it continues to control the movement of goods in and out of the territory via an air, land, and sea blockade. When Gazans were under full lockdown this summer, for example, Israel restricted fuel supplies in response to rocket attacks Hamas launched against Israel. That amounts to “collective punishment” of Palestinians, says Miriam Marmur, spokesperson for the Tel Aviv-based rights group Gisha, “which plunged people into darkness most hours of the day.” Some commenters—and Israel’s coordinator of government activities in the occupied Palestinian territories, COGAT--have argued that Israel is not responsible for the health of Palestinians because the Oslo Accords, the historic agreements Israel signed with the Palestinian Liberation Authority in the early 1990s, give the Palestinian Authority oversight of public health under the principles of self-determination. “It’s important to mention that Israel has not denied any request for medical assistance that has reached its doorstep,” a spokesperson for COGAT told Al Jazeera for a story published on Jan. 13. Until their public statement on the matter on Jan. 10, Palestinian officials had made contradictory claims on whether or not they had asked Israel for vaccinations. But Israeli authorities citing the Oslo accords is an example of how they do so “at their convenience,” says Marmur. “In reality, Israel has undermined the ability of the Palestinian Authority and also of the de-facto Hamas Authorities in Gaza to actually take full responsibilities for health as was provided for in the Oslo agreement.” U.N. human rights experts say that the Oslo Accords must be “interpreted and applied consistently with international law, and cannot derogate from its broad protections,” according to the Jan. 14 OCHA statement. The exclusion of Palestinians from Israel’s vaccination program is “reflective of a system of apartheid,” says Dr. Mustafa Al Barghtoy, a physician and former Palestinian minister who serves on the Palestinian health committee dealing with COVID-19. The injustice is underscored by the fact that hundreds of thousands of Israeli settlers are eligible to receive the vaccine, he says, while their Palestinian neighbors are not. Meanwhile, Israel will be vaccinating prison guards, but not the Palestinian political prisoners they oversee, he adds. How urgent is the need for vaccinations in the Palestinian territories?In total, more than 160,000 Palestinians in the occupied territories have tested positive for the coronavirus since March 2020, with more than 1,700 deaths related to COVID-19, according to the U.N’s figures. But those numbers might not tell the whole story: among those who are tested, the rate of infection in the occupied territories is 30%, compared to 7.4% in Israel, says Barghtoy. Many had feared that COVID would especially devastate the Gaza strip—one of the world’s most densely populated areas, with an ill-equipped health system. As of Jan. 14. Gaza’s health ministry had reported almost 47,000 cases and 464 deaths due to the virus. That’s an alarming number, but still lower per-capita than the more than half a million cases Israel’s Health Ministry reported on Jan. 12. The impact has in part been mitigated by the international community’s “tremendous” efforts to shore up Gaza’s health system, says the WHO’s Rockenschaub. That includes substantially scaling up the strip’s intensive care unit capacity and mobilizing vital supplies such as oxygen and ventilators. Still, vaccinations are an urgent concern. “The sooner we can move in vaccinating and protecting essential health workers the better,” he says, “because we see quite a substantial number of the health workforce being infected.” Before the PA formally said Israel is responsible for vaccinating Palestinians, the WHO had informally requested Israel provide vaccinations to inoculate frontline Palestinian health workers. Israel denied that request on the basis of vaccine shortages for its own citizens. Can Israel achieve herd immunity without inoculating Palestinians?With the IDF moving throughout the West Bank, and some 130,000 Palestinians working in the settlements or Israel, not making the vaccine available is “counterproductive” in terms of achieving herd immunity, Barghotoy says. The Palestinian Authority has made efforts to import vaccines independent of Israel. Its health ministry on Jan 11 announced it had given emergency approval to Russia’s Sputnik V Covid-19 vaccine for use in areas it administers under limited Palestinian self-rule; it also says it has struck a deal with AstraZeneca for vaccines it expects to receive in late February. On top of that and the first shipment of vaccines under the WHO’s COVAX program could become available as early as February. For the next few weeks at least, they will be forced to wait. “Our main concern is really that we can only overcome this pandemic in solidarity and in a collaborative spirit,” says Rockenschaub, “We will either succeed together or we will fail together.” from https://ift.tt/3sw6fOr Check out https://takiaisfobia.blogspot.com/ Since the global pandemic began, one of the grimmer features of daily life has been watching the coronavirus death count tick up and up as the months have gone by. With so much unnecessary death in 2020, it’s surprising that in many countries, at least according to preliminary numbers, there was one significant group that actually saw its death rates fall: children. Data from the Human Mortality Database, a research project run by a global team of demographers, suggest that COVID-19 did not reverse years-long declines in child mortality, despite a mortality surge in the general population. Demographers, pediatricians and public-health experts say it’s possible that lockdowns and quarantines have prevented children from succumbing to deadly injuries and illnesses. But they also point out that other effects of the pandemic, such as lower vaccination rates and reduced prenatal care may increase childhood mortality rates going forward. The database, jointly maintained by the University of California, Berkeley, the Max Planck Institute for Demographic Research in Rostock, Germany and the French Institute of Demographic Studies in Aubervilliers, France, publishes mortality figures for 38 countries on a weekly basis. As expected, the so-called “excess mortality”—the number of deaths in a population above a normal baseline—was consistently high throughout each country’s pandemic period. (There were a few exceptions like Australia and New Zealand, which managed to contain the virus with early and aggressive lockdown measures.) When broken out by age, however, the data show that fewer children under age 15 died in 2020 compared with prior years, even after accounting for COVID-19-related deaths. Take the U.S., for example, where about 26,000 child deaths in 2020 have been recorded so far. That’s well below the average in recent years, as shown in the chart below:
At this point, it’s impossible to say with certainty how extreme an outlier 2020 was. Between January and mid-November, about 2,500 fewer children in the U.S. died last year compared with the average of the three years prior—a drop of about 9%. However, demographers caution that the 2020 tally is almost certainly undercounted due to lags in reporting. As the death records get updated in the coming weeks, the second half of 2020 will likely start to look more like the first half of the year, which clocked a 7% drop. That would put the yearly deficit at about 2,000 deaths below the 2017 to 2019 average. It’s possible that, as longer death investigations begin to settle in the coming months and years, the gap between 2020 and previous years will shrink in terms of overall child mortality. But presuming 2020 child mortality remains lower than prior years once the data dust settles, it would be an extension of recent trends, says Magali Barbieri, the Human Mortality Database’s associate director. “One thing that’s happening is that mortality has been declining for the zero-to-14 group,” she says. “If you compare 2019 to previous years, you’ll see a deficit, as well.” In any other year, a continuing decline in child mortality would be good news, but not unexpected. In a year like 2020, it’s astonishing. Given the deadliness of COVID-19 in so many demographics, it’s incredibly fortunate that children have been largely spared due to their effective immune system response to the virus that causes the disease. In the U.S., just over 100 children under age 15 died from COVID-19 in 2020. They account for 0.03% of the 376,000 COVID-19 deaths since the virus hit the country last spring and less than 0.5% of the 26,000 total child deaths from all causes. In a year characterized by catastrophe, that’s one small grace. Explaining the drop in child mortality“We are in a privileged historical position that, barring terrible tragedies, children live to grow up,” says Dr. Perri E. Klass, a New York pediatrician and author of the 2020 book A Good Time To Be Born: How Science and Public Health Gave Children a Future. Citing U.S. data, she notes that “most child deaths are in the first month of life, and they are linked to premature gestation and reasons that are connected to the circumstances right around their birth. We aren’t losing nearly as many children to the things that used to kill two- and three- and eight-year-olds, like diphtheria, sepsis, scarlet fever or polio.” Indeed, the leading cause of childhood mortality in the U.S., after the newborn stage, is unintentional injury—things like drownings, car accidents, pedestrian fatalities and accidental suffocations, according to 2018 numbers from the U.S. Centers for Disease Control and Prevention. The agency’s cause-of-death data for 2020 (with the exception of pneumonia, influenza and COVID-19-related deaths) won’t be available until the end of 2021. In the meantime, child health experts can only speculate how the pandemic is shaping the numbers. Several who spoke to TIME said it’s possible that lockdowns, quarantines and social distancing measures are keeping kids safer from physical and biological harm, even as they threaten social, emotional, and mental well-being. “If those data hold, and if it’s true that 2020 mortality was down, then it may well turn out to be around issues of safety, and of people moving less and driving less,” says Klass. Some early reports support that idea: the U.S. Department of Transportation has estimated there was a 2% drop in motor vehicle traffic crashes during the first half of 2020 compared with the same time period in 2019. National drowning data are difficult to come by, but statistics compiled by Total Aquatic Programming, an aquatics consultancy that has tallied drownings since 2008, tabulated fewer child drownings in 2020 compared to 2019. Warm-weather places that publish running tallies of children who drowned, like Texas, Florida and Phoenix, Ariz., show similar numbers or modest decreases compared with recent prior years. In addition to curbing injury rates, it’s possible the pandemic has kept young kids from getting severely ill. Influenza and pneumonia are leading causes of death among toddlers and young children, but last spring, researchers found that influenza, respiratory syncytial virus and other common respiratory viruses died out quickly in response to lockdown measures designed to target COVID-19—and they have not resurged, despite the onset of cold and flu season. (Klass points out that health protocols like wearing masks and washing hands don’t just prevent COVID-19 but other viruses, as well.) Why it isn’t all good newsThe problem, though, is that, in future years, we may see child mortality increase on a global scale due to the pandemic lockdowns of 2020 (and, perhaps, 2021). For instance, water safety advocates say that declined enrollment in swim programs coupled with a surge in demand for private pools could lead to more drownings. Also, delays in vaccinations for things like measles, fueled by school closures and suspended immunization campaigns in dozens of countries, could cause outbreaks of serious but otherwise preventable diseases. And reduced access to prenatal care during the shutdown could negatively affect fetal health. On top of those concerns, stressors such as income losses, social isolation and ongoing health problems also could have lasting effects. “One cannot rule out the fact that the economic and social consequences of the pandemic on women of reproductive ages and their children had a detrimental impact on their health,” says Barbieri, whose preliminary research suggests that child mortality around the time of the 2008 economic recession increased among the poorest segments of the population. Taken together, all these issues may end up setting back child mortality on a global scale. The outcome could be most dire in less developed countries, where health care infrastructure was already fragile, says Li Liu, associate professor at Johns Hopkins Bloomberg School of Public Health. “Potentially, cases like preterm birth and congenital abnormalities may actually be going up, once we have all the data in,” she says. “We can speculate and come up with theories but we have to wait until data are available to test those theories.” And therein lies the one sure thing among the uncertainty: Because COVID-19 has not led to many childhood fatalities, but has upended the lives of children and pregnant women in significant ways, researchers are seizing a unique opportunity to study child wellbeing and survival. That new knowledge can be used to develop public health practices that can keep children mentally sound and physically healthy and safe when life returns to normal. from https://ift.tt/2XIkEsG Check out https://takiaisfobia.blogspot.com/ Johnson & Johnson’s experimental one-shot Covid-19 vaccine generated a long-lasting immune response in an early safety study, providing a glimpse at how it will perform in the real world as the company inches closer to approaching U.S. regulators for clearance. More than 90% of participants made immune proteins, called neutralizing antibodies, within 29 days after receiving the shot, according to the report, and all participants formed the antibodies within 57 days. The immune response lasted for the full 71 days of the trial. “Looking at the antibodies, there should be good hope and good reason that the vaccine will work,” in the company’s late-stage clinical trial that’s soon to report results, J&J Chief Scientific Officer Paul Stoffels said Tuesday in an interview. The one-shot vaccine generates more neutralizing antibodies than a single dose of other front-runner Covid-19 vaccine, all of which are two-shot regimens. But when compared with two shots of these rivals, the response to J&J’s single shot is in the same range, Stoffels said. Interim results from the phase 1/2 trial of 805 participants ages 18 and older were published Wednesday in the New England Journal of Medicine. The data expanded on more limited findings J&J first published in September. Shares of the New Brunswick, New Jersey-based drugmaker rose 1.3% in post-market trading on Wednesday. Moderna Inc., which makes a two-dose Covid vaccine that’s been authorized for emergency use, fell 0.6% after U.S. markets closed. J&J’s progress is being closely watched by top infectious disease experts because its vaccine has the potential to become the first that can protect people after just one shot, making mass-vaccination campaigns much easier. The company expects to get definitive efficacy data from a final-stage study by early next month, potentially leading to regulatory authorization by March. Efficacy AmbitionsThe U.S. has granted emergency-use authorizations to two vaccines, one developed by Pfizer Inc. and its partner BioNTech SE, and the other by Moderna Inc. Both employ a technology called messenger RNA that has never before been used in an approved product, and each showed more than 90% efficacy against Covid-19 symptoms. Those results were better than expected. U.S. government officials had earlier said any vaccine with greater than 50% efficacy would be considered a success. Based on that guidance, J&J aimed for 60% effectiveness, Stoffels said, but “we hoped and we planned for 70%.” Within weeks, J&J will learn how its vaccine performed in a late-stage trial of 45,000 volunteers. Stoffels now thinks it has the potential to be even higher than 70% effective, based on the early-stage findings and other factors. When the antibody response to J&J’s shot is compared to others that have been through final stage trials “there’s a good reason to believe we can get into very high levels of efficacy,” Stoffels said. “Will it be north of 90%? I don’t know. The data will tell us.” Moncef Slaoui, the chief scientific adviser to the U.S.’s Operation Warp Speed vaccine development and distribution effort, said Wednesday that he anticipates J&J’s one-shot vaccine will show 80% to 85% effectiveness against Covid-19. J&J and its government partners can’t see the data for the time being, a standard measure to prevent bias. One-Dose AdvantageExperts have said that a single-shot vaccine offers advantages: ease of distribution and administration. Vaccines from Moderna, AstraZeneca Plc, and the Pfizer-BioNTech partnership all require two shots, which means repeat shipping and clinic visits. While Moderna and Pfizer-BioNTech’s shots must be frozen, J&J’s shot can be stored at refrigerator temperatures for three months. “A single dose is going to be so much more effective in the world,” Stoffels said. “We are very confident that it works,” but another trial J&J is conducting of its vaccine plus a booster shot “will give us a backup.” The study released Wednesday also found that a second dose of J&J’s shot, administered two months later, led to a three-fold increase in neutralizing antibodies. Stoffels said that’s positive news, as the drugmaker is still evaluating how long immunity from the single-shot will last, and whether higher antibody levels will be needed to combat new strains of the virus. J&J kicked off the separate late-stage study of its two-dose vaccine regimen in November. Stoffels said the company is likely to finish enrolling the 30,000 participants before the end of first quarter, likely in March or April, and expects a data readout come summer. Underlying PlatformJ&J’s vaccine candidate is made from a cold virus, called an adenovirus, that’s modified to make copies of the coronavirus’ spike protein, which the pathogen uses to enter cells. Though the altered virus can’t replicate in humans, it induces an immune response that prepares the body for an actual Covid-19 infection. It was first developed with researchers at Harvard University who have spent years working on the adenovirus platform, which is also used in J&J’s Ebola vaccine, as well as its Zika, RSV, and HIV investigational vaccine candidates. The NEJM report showed the vaccine was well-tolerated across the study participants. There was no difference in the immune response in younger participants and the elderly, which is important given older populations are most vulnerable to the disease. The most frequent side effects were fever, fatigue, headache, muscle pain and injection-site pain.
Dr Rachel Clarke never dreamed that in her medical career, she would say out loud that hospitals in Britain are running out of oxygen. Yet some hospitals in the U.K. are now in that critical situation, as doctors say the U.K.’s third wave of the coronavirus pandemic is pushing the country’s National Health Service to its limits. “We’re seeing younger patients, we’re seeing sicker patients, and we’ve never really recovered from the first wave,” says Clarke, who works on an acute medical ward in a hospital in Oxfordshire, England, and also in an in-patient hospice setting. “You can’t sugarcoat the situation currently in the NHS in Britain. It is unimaginably bad.” The U.K. is currently enduring a painful third wave of COVID-19, far worse than its European neighbors like Spain, France, Italy and Germany. (The Republic of Ireland currently has the world’s highest number of confirmed new COVID-19 cases per capita.) On Wednesday Jan. 13, the U.K. reported a record high of 1,564 deaths within 28 days of a positive COVID-19 test—the biggest figure reported in a single day since the pandemic began, bringing total deaths to more than 84,000. Experts say that the current situation in the U.K., and particularly in London—which declared a state of emergency on Jan. 8 is a cautionary tale. They say the crisis is a result of both the struggle to deal with a new variant estimated to be up to 70% more transmissible, and because of a failure in decisive and strong government leadership. Read More: A New, More Contagious COVID-19 Strain Has Been Reported in the U.K. Is It Headed for the U.S.? One of those failures, they say, was that the U.K. government did not act on the scientific advice that recommended a short “circuit breaker” lockdown in September to halt rapidly rising transmissions after the easing of lockdown restrictions in the summer. Although a second round of national restrictions were introduced in November, it was eased in December and cases rapidly climbed throughout the month. On Jan. 4, Prime Minister Boris Johnson announced a third national lockdown in England, with people only allowed to leave their homes for a select few reasons and non-essential shops and businesses closing. (Wales, Scotland and Northern Ireland each have their own healthcare rules and have also instructed national lockdowns).
The U-turns in policy and the failure to enact a national lockdown early enough this autumn have likely had deadly consequences. Clarke is now seeing patients who caught the COVID-19 virus from a family member who spent Christmas Day with them (as permitted by government rules in certain parts of the country), resulting in entire families becoming infected. “When I see now people dying of COVID-19, who I know might not have caught it had the government been braver and more willing to stand up and put lives first—I find that heartbreaking,” she says.
The picture inside U.K. hospitalsGovernment officials said Monday that the U.K. is at the “worst point” of the pandemic, with 50% more coronavirus patients in hospital now compared to April last year. The same day, Johnson acknowledged oxygen shortages in some places, and reports emerged of hospital mortuaries reaching capacity in one south-eastern region, leading to bodies being stored at a temporary mortuary. “Off the scale” waiting and queuing times for ambulances have been reported in London and parts of the south-east, and many are warning that the worst is yet to come. “The hospitals are full. The intensive care units are full,” says John Ashton, a former regional director of public health for north west England and the author of Blinded by Corona: How the Pandemic Ruined Britain’s Health and Wealth. “People will not be admitted, and will be very sick and dying at home, that’s what’s going to happen over the next two or three weeks.” Clarke remembers watching in disbelief the scenes of the first wave of COVID-19 unfolding in New York City. “That’s what we are going through in Britain at the moment,” she says. “We have ambulances trapped, queued up outside hospitals for six, eight, ten hours at a time because they can’t physically offload their patient and actually get them into hospital at the moment.” Data from Public Health England indicates that there are more people of all ages in hospital in the U.K. with COVID-19 now than in the first wave of spring 2020, including the young and the old. Infections have been highest in teenagers, students, and people in their 20s and 30s in recent months, and the highest hospital admission rate for confirmed COVID-19 has been in the over-85s. There has also been a steep rise in the number of 65-74 year olds and 45-64 year olds admitted to intensive care units. Read More: The U.S. and U.K. Were the Two Best Prepared Nations to Tackle a Pandemic—What Went Wrong? The overwhelming burden on the National Health Service is affecting other patients who do not have COVID-19, but who also are in pain and need treatment or other surgeries. At the north London hospital where spinal surgeon Dr. Hilali Noordeen is based, seven out of the nine operating theaters have been repurposed and made into intensive care units for COVID-19 patients. “The whole of our hospital now, save two male beds and two female beds, are not available for us because they are either full of COVID-19 patients or waiting for COVID-19 patients,” says Noordeen, author of the forthcoming book Letters to a Young Doctor, adding that his hospital is now down to 60% nursing capacity as staff have had to self-isolate at home. A letter earlier in January from the chair of the British Medical Association to its members said that over 46,000 hospital staff were off sick with COVID-19. The lack of capacity, both in terms of facilities and staff, means that on the day Noordeen speaks to TIME, he initially had a list of three pediatric patients with severe spinal deformities to attend to—all those appointments had to be canceled. “I don’t know how many months it’s going to be able to take us to deliver these treatments now,” he says. For junior doctor Kieran Killington, who was redeployed from general practice to a west London hospital, the biggest change he’s noticed is the exhaustion of staff. During the first wave, he heard many colleagues say that it would be hard to cope with the same level of stress again, and yet they now feel they’ve been thrown into a situation where they have to. Clarke too shares that same sense of disappointment, that the mistakes made in the government’s delayed response to the first wave have been replicated now. “The fact that this is the second time round makes it so much more inexcusable and so much harder for staff,” she says. Results from a new study published in the British Medical Journal on Jan. 13 indicated that nearly half of NHS critical care staff surveyed who worked in intensive care units through the first wave reported symptoms of post-traumatic stress disorder, severe depression or anxiety. Of those surveyed, more than one in seven clinicians and more than one in five nurses working in ICUs reported thoughts of self-harm or suicide. 
How did England end up here and how can other countries avoid it?The new variant of COVID-19 first reported in mid-December is partly to blame for the grave situation in England, experts say. Mutations in the virus make this new strain 50%-70% more transmissible than others, scientists estimate. According to the U.K. government the new strain was likely present in the country as early as September. At least 50 more countries have now reported cases, according to the WHO. British officials have repeatedly said that without the emergence of the new variant, social distancing measures which have been in place across most of England since mid-October, including bans on most indoor gatherings, would have been enough to contain COVID-19. But public health experts say government strategy on COVID-19 contributed both to the surge in cases, and to the emergence of the new variant itself. Many have criticized the government’s decision to considerably loosen restrictions over summer after the first lockdown in spring in order to try to revitalize the economy. Researchers at the University of Warwick found that a government-backed food voucher scheme, dubbed “Eat Out to Help Out,” which encouraged people to dine at restaurants by subsidizing a portion of their meal, drove new infections up by 8% to 17% and accelerated a second wave in the fall. The scheme cost taxpayers almost $1.2 billion. The emergence of the new variant of the virus, says Ashton, the former public health official, was made more likely by the wide spread of infections. “The more people the virus goes through, each generation of people it infects—that gives the virus an opportunity to adapt and get better at doing its deadly work,” he says. Read More: How the U.K. Mismanaged Its Coronavirus Response Government messaging around Christmas may also have driven transmission in December. Initial plans allowed for five days of mixing of up to three households indoors—far more than other European countries. Those plans were scrapped just a few days before Christmas as the spread of the new variant became clear, with new local measures allowing either no indoor mixing or only one day of mixing with two households. But Ashton says restrictions were not introduced early enough to stop rapid spread over the Christmas period. In a survey by the U.K.’s Office of National Statistics, 44% of adults admitted to forming a “bubble” with up to two other households on Dec. 25. “This is the beginning of the Christmas wave,” Ashton says. “We’re still in the foothills of what’s in the pipeline to come from Christmas and New Year.” The U.K.’s overall strategy for combating COVID-19 appears to have been driven by a different understanding of the virus compared to other countries with lower death tolls, said Devi Sridhar, professor and chair of Global Public Health at the University of Edinburgh’s Medical School, speaking at a session of parliament’s Health and Social Care Committee to examine the effectiveness of previous lockdowns in November. The U.K.’s heavy toll “comes down to an early decision to treat this like a flu-like event, that would pass through the population, [with] an uncontrollable spread that you would try to mitigate through building enough hospitals and medical care,” she said. “Rather than treating this like a SARS-like event, which is what East Asian countries have done, as well as the Pacific, Australia, New Zealand, as well as some countries in Europe, like Norway, Finland, Denmark, who are diverting from that flu model and trying to keep their numbers as low as possible.” Ashton agrees that the U.K. failed to “follow through [with successful early lockdowns] like they’ve done in other countries,” because of a focus on the economy. “The way we’ve handled it, we’re going to have the worst of both worlds: the biggest economic impact, and the worst health impact, both in terms of deaths, and people suffering with long COVID,” he says. “That’s because we haven’t been decisive.” Though national economic output bounced back as restrictions were lifted during the second and third quarters of 2020, that recovery proved short-lived, with the economy contracting again in the fourth quarter. By the end of 2020, the U.K. economy was 10% smaller than at the end of 2019. How long will England’s lockdown last?There’s no clear end in sight for England’s lockdown. Although the government has tentatively set a date of mid-February to begin easing measures, the legislation on the new restrictions lasts until March 31. Transmission is so high that, according to government estimates, 1 in 50 people in England currently have COVID-19. In the capital, the average is 1 in 30, or 1 in 20 in “hot spot” areas, London mayor Sadiq Khan said on Friday. As a result, the prime minister is pinning hopes for loosening restrictions on the ability to rapidly vaccinate the 15 million people in the government’s four priority groups: care home residents and their carers, people over 70, frontline health and social care workers, and those considered “clinically extremely vulnerable.” If things go well, Johnson said on Jan. 4, those groups will all receive at least their first dose of a vaccine by the middle of February. Only then could some restrictions be relaxed, as vaccines continue for the rest of the population. Read More: mRNA Technology Gave Us the First COVID-19 Vaccines. It Could Also Upend the Drug Industry It’s unclear if it will be possible to roll out the vaccine that quickly, though. Since vaccines began to be administered on Dec. 8, only 2.4 million people have received a first dose. The U.K. has so far approved three COVID-19 vaccines: those produced by Pfizer-BioNTech, AstraZeneca-Oxford, and most recently Moderna. The AstraZeneca-Oxford vaccine, which can be stored at normal fridge temperatures and of which the U.K. has ordered 100 million doses, is expected to speed up the rollout. But given the immense pressures on health service staff and resources, ramping up the necessary level of 2 million doses a week by the end of January will be extremely difficult, Ashton says. “I fully expect this vaccination program will be the next casualty of over promising and under delivering. It’s unbelievable.” In the meantime, the outlook for England’s hospitals looks bleak. According to a report by health service news outlet HSJ, the NHS expects London’s hospitals to be short of some 2,000 beds by Jan. 19, even under a “best case scenario” of lowering transmission rates and emergency hospital facilities being opened. Clarke, the doctor in Oxfordshire, is steeling herself for the coming weeks. “Knowing that the population is being vaccinated is pretty much the only thing that is stopping me wanting to dissolve and crumble right now,” she says. “Vaccines are the one chink of light to hold on to.” from https://ift.tt/3soxZVa Check out https://takiaisfobia.blogspot.com/ Data Show More Women Are Freezing Their Eggs During the Pandemic Defying Doctors Expectations1/13/2021 If she found the right guy, Kari Arenberg could see herself having kids. But her work was never conducive to dating, let alone to freezing her eggs in hopes of leaving her options open. The 31-year-old event producer traveled constantly between New York City and Los Angeles, with long days lifting heavy boxes and running around venues. Then, in 2020, Arenberg was furloughed, and the egg-freezing process became, for the first time in her life, logistically possible. She moved in with her family in Chicago and visited a clinic. Soon she was giving herself as many as three shots a day to stimulate her ovaries, and visiting the clinic every few days for bloodwork and an ultrasound to determine when the eggs would be ready for retrieval. She was able to freeze 21 eggs, a feat that likely would have been impossible if she had had to give herself shots while stuffed into airplane bathrooms or trying to schedule visits to the clinic around the national events, like Comic Con, that she produces. “I love my work and want to prioritize it,” Arenberg says. “So it’s ironic that my career also kept me from doing this earlier.” When the coronavirus pandemic hit, fertility clinics braced themselves for a downturn. People have been avoiding the doctor’s office since the spring, first because they feared exposure to the virus and later because many people who have been laid off or furloughed cannot afford the medical bills. Fertility treatments are expensive, and the cost of egg freezing ranges from $6,000 to $20,000. (Arenberg’s was $12,000—an especially daunting cost after losing work.) But clinics across the country are reporting an uptick in women freezing their eggs during the pandemic. Though no organization in the U.S. collects national data, 54 clinics across major American cities including Denver, Atlanta and Seattle told TIME that the number of women freezing their eggs has increased year-over-year—an impressive stat considering most of those clinics were forced to shut down and suspend fertility treatments in the early months of the pandemic. An additional five clinics reported the same number of egg freezing cycles in 2020 as in 2019 despite being closed anywhere from one to three months in 2020. Only two clinics told TIME they had seen a decrease in the number of women freezing their eggs since 2019. “We didn’t know what to expect,” says Colleen Wagner Coughlin, the founder of OVA Egg Freezing Center in Chicago. “If anything we expected a downturn. But we’ve seen a huge increase—several hundred more new patients [in 2020].” At some clinics, the changes have been robust. When TIME collected data in November, Shady Grove Fertility, which runs 36 clinics across the Eastern seaboard, had seen a 50% increase in women freezing their eggs since 2019. Doctors at NYU Langone saw a 41% year-over-year increase in women fertilizing their eggs. And Seattle Reproductive Medicine had conducted 289 egg-freezing cycles in 2020, compared with 242 in 2019, a nearly 20% jump. 
Sharon Covington, a therapist who provides counseling services at Shady Grove Fertility Clinic, is “busier than ever” offering mental health support to women considering fertility treatments, including egg freezing. She says the women she sees are freezing their eggs because of the pandemic, not in spite of it. Women who normally travel for work, like Arenberg, are grounded. Those with busy social lives are alone at home. Their schedules are open. But that time in isolation has also afforded space for reflection. “Everybody had to take a hard stop in their lives,” Covington says. “And I think what happened with that is that it gave people the time and the space to kind of reassess their priorities and the directions that they’re taking in their life.” Many single people feel as if they’ve fallen a year behind on their life plans. Dating was almost impossible at the beginning of the pandemic. Even now, near-strangers must negotiate a difficult social dance with one another when they agree to meet up for a distanced drink—when can they hug, kiss or even just go indoors together? When will they feel safe with one another? “I actually went on a few dates,” says Arenberg, “but sitting outside shivering in Chicago in the winter is not conducive to finding someone.” Read More: The Coronavirus Is Changing How We Date. Experts Think the Shifts May Be Permanent Arenberg first heard about egg freezing when the winner of the Bachelor’s 2015 season, Whitney Bischoff Angel, revealed that she froze her eggs. Egg freezing has steadily grown more popular in the years since the American Society of Reproductive Medicine (ASRM) removed the “experimental” label from the procedure in 2012. Many women were already freezing their eggs for medical reasons, either because they were going through a medical procedure like chemotherapy that could reduce their fertility or had a medical condition like endometriosis that could negatively impact ability to conceive. But with the change in labeling came the rise of what doctors call “social egg freezing”—women who freeze their eggs simply because they aren’t ready to have a child yet. In 2009, just 475 women froze their eggs, according to the Society for Assisted Reproductive Technology. By 2018, 13,275 women did so, an increase of 2,695%. The spike comes thanks in part to celebrities like Chrissy Teigen, Michaela Coel and Emma Roberts sharing their own egg-freezing stories. Kourtney Kardashian went so far as to film her egg freezing preparation on Keeping Up With the Kardashians, and Amy Schumer shared pictures of her bloated and bruised stomach as she took the shots this summer to freeze her eggs as part of her IVF process. They’ve demystified a process that was little known just a few years ago, including, in Schumer’s case, the most uncomfortable aspects. René Hurtado, a 28-year-old in Scottsdale, Ariz., knew that she might have to stay home in the weeks before her egg retrieval in case she suffered side effects like cramping or headaches, and believed the pandemic would be the ideal time to nurse those pains without missing meetups with friends. “On day five of injections, I couldn’t even walk. I only felt good if I was lying flat on my bed,” she says. She had to take several days off from her job at WeWork while she recovered. “In an alternate world, I was supposed to be in Miami for a bachelorette party that week. Thank God I did this during COVID so I didn’t have to see anyone or go anywhere because I was in so much pain.” 
Hurtado’s offered egg freezing as part of the company’s benefits package, a perk that’s become increasingly popular among startups as a means of attracting women workers (or, in critics’ eyes, pressuring workers to prioritize work over family). But the trendiness of egg freezing in Silicon Valley may be reaching its peak. Some doctors have cast doubt as to whether companies will continue to offer this costly benefit when many organizations are choosing between cutbacks and layoffs. Wagner Coughlin, the founder of OVA in Chicago, said that her organization is already looking into a new payment structure in anticipation of companies’ dropping the benefit. Michael Jacobs, a doctor at the IVF Center of Miami, believes that moment has already arrived. He was one of the few doctors who told TIME his clinic was seeing a downturn in egg-freezing rates. “In cities like New York and Los Angeles, maybe there are more people who can afford the cost of egg freezing right now,” he says. “But I think a lot of people here are just worried about paying their bills.” The high price of egg freezing has long meant only a specific subset of patients—mostly upper class, and mostly white—pursue the process: a study of nearly 30,000 egg retrievals by ASRM found that just 4.5% of the women who underwent the procedure described themselves as Hispanic and 7% identified as Black. Read More: Women Are Deciding Not to Have Babies Because of the Pandemic. Why That’s Bad for All of Us. Pavna Brahma, a doctor at the Shady Grove clinic in Atlanta, theorizes that this may be the boom period before a bust. “People are coming in who are worried about losing their job or their coverage or their insurance,” Brahma says. “They want to take advantage of the moment when they know they have coverage and economic stability in their job.” She stresses to her patients that waiting until they receive the vaccine to freeze their eggs is a viable option: “Two to six months rarely makes a huge change in their fertility. I don’t want women to feel pressured by the pandemic.” 
Still, pandemic or not, time remains a key driver in women’s family-planning decisions. As a general rule, the younger you are, the more eggs you have, and the more likely an egg-freezing process will be successful. Many women fear the benchmark of 35 years old. Loss of eggs and risks to pregnancy happen gradually over time, not all at once, but 35 is when doctors begin calling pregnancies “geriatric” to reflect increased risks. It’s also the age at which fertility doctors will advise freezing more eggs, often through several procedures to harvest as many eggs as possible and improve the chances that one can be fertilized later. Bryn Woznicki, a 33-year-old filmmaker who lives in Los Angeles, has always known she wants to be a mother, “but every year,” she says, “it’s a ticking time bomb working against your biological clock.” When filming work dried up last spring and dating became more difficult, she took stock of what turning 34 during a pandemic could mean. “Say I met someone today,” she says. “Say I really liked them and we got married. By the time I did that and enjoyed my partner and we decided to take on this huge responsibility of having kids, that’s another few years down the line.” With her work and social life on pause, she decided to divert some of her savings towards a potential future family. “I had some money saved to try to move to New York this fall and then, you know, COVID happened,” she says. “Meanwhile I was feeling the pressure from my biology telling me that time was running out, and I was like this is the one thing I can control in an unpredictable year.” For Arenberg, being able to freeze her eggs was a “silver lining” of the pandemic. “As unfortunate as it is that I’m technically unemployed, this really gave me the mental capacity to look ahead for the first time,” she says. “I don’t know if I want kids, but maybe if I meet the right person some day, this just provided a nice comfort level where I can make some decisions about dating and kids and work when things get back to normal.” from https://ift.tt/35Fjumb Check out https://takiaisfobia.blogspot.com/ On Jan. 7, 2021, the U.S. hit another grim milestone, for the first time recording over 300,000 new cases of COVID-19 and over 4,000 deaths from the infection in one day. Across the country, hospitals and intensive care units are now under enormous strain trying to treat so many sick people. And if a new, more transmissible variant of SARS-CoV-2, the virus that causes COVID-19, were to take hold in the U.S. as it has in the U.K., as seems plausible, our health system could pass its breaking point. It’s all too easy to become numb to the toll and accept these daily figures as a new normal while waiting for the vaccine rollout to have an impact. Since the first vaccines were approved in Dec. 2020, we seem to have stopped talking about the rising cases and deaths. But we must not just accept this level of infection, suffering, and devastation for months on end while we wait until we reach vaccine herd immunity sometime in the summer or fall. COVID-19 is a preventable illness. Many countries, like Australia, China, New Zealand and Taiwan, have practically ended community transmission of the virus and returned to a near-normal life, and they did so without using a vaccine. If we continue to see rising transmission, it will make it all the more challenging for vaccines to act as a tool that ends the U.S. pandemic. There are five key actions we can—and should—take urgently to drive down viral transmission. First, we need to get every American a high-filtration maskWidespread mask wearing across the community is linked with lower transmission rates; face masks reduce viral transmission in two ways. First, they prevent infected people from spreading the virus to others (masks act as “source control”). This effect is particularly important for people who are infected but don’t yet have symptoms—they feel fine and so may be unaware that they are infectious. Second, masks can also help protect the wearer from inhaling virus-laden droplets or aerosols. However, not all masks are equally effective at filtering out the particles that carry the virus. One recent study, for example, found that some masks (e.g. N95 masks and masks comprising two woven nylon layers and a nonwoven filter insert) do a better job than commonly used cloth and surgical masks. So, we need to urgently get these more effective “high-filtration” masks to all Americans. Dr. Abraar Karan at Harvard Medical School and his colleagues argue that the incoming Biden administration should invoke the Defense Production Act to urgently mass manufacture high-filtration masks and fund research to develop new mask designs. We can learn from the remarkable success of South Korea and Singapore, where governments early on manufactured and distributed high-filtration masks (e.g. K-94 masks, the Korean equivalent of N95 masks) to all at no cost to its citizens. In Singapore, you can even get a high-filtration mask for free from vending machines. Why can’t the U.S distribute masks in this way to Americans too? Second, schools and workplaces need to be made saferOn Jan. 20, 2021, it will be exactly one year since the first case of COVID-19 was confirmed in the U.S. It is unconscionable that in all this time we have still not made the necessary investments into schools and workplaces to make these settings safer. The science is clear on the steps that need to be taken—including ventilation, air filtration, spacing between people, universal masking, and reducing the density of people. Third, we must protect our essential workersIt is a moral stain on this country that so many essential workers—including in clinics, hospitals, nursing homes, grocery stores, schools, factories, farms, and warehouses—have been infected and so many have died. While there is no accurate database on health worker infections, by Nov. 15, 2020, the CDC estimated that there had been 216,049 health care worker infections in the U.S. An investigation by Kaiser Health News and the Guardian found that nearly 3,000 U.S. health workers had died as of Dec. 23, 2020, of which around two-thirds were people of color. We’ve witnessed terrible scenes in which nurses and doctors have had to improvise their own personal protective equipment (PPE) out of trash bags, pool noodles, and snorkel masks. It’s equally difficulty to quantify with certainty how many grocery or warehouse workers have been impacted by the virus, but Amazon says that from March 1 to Sept., 19, 2020, 19,816 of its frontline Amazon and Whole Foods Market employees tested positive or were presumed positive. Enough is enough: every single essential worker in America deserves to be protected from COVID-19 with the highest quality PPE combined with the other measures described above to improve building safety. Fourth, we need to urgently build a functioning nationwide “test, trace, isolate, support” (TTIS) systemThe nations that have successfully controlled viral transmission, like Australia, China, Hong Kong, New Zealand, Singapore and Taiwan, have at least one thing in common: they have systems in place to efficiently identify infected and exposed people. This is crucial for controlling transmission, because it means infected people know they need to isolate (isolation means an infected person keeps away from others) and exposed people know they need to quarantine (quarantine means someone who might have been exposed stays away from others). The U.S. needs to emulate, not ignore, this success. The “support” component of TTIS is critically important—people need financial support to isolate or quarantine to replace any lost wages. North Carolina, for example, has such a support program in 29 counties, called the COVID-19 Support Services program, which provides money and delivers meals, medications, face masks, and hand sanitizers to people isolating or quarantining. One powerful tool that could help control transmission in the U.S. would be widespread, frequent and accessible rapid antigen testing. These tests can identify contagious people before they get symptoms. I was one of over 50 U.S. public health experts who signed a Dec. 15 open letter to the federal government, led by Dr. Michael Mina at the Harvard T.H. Chan School of Public Health, to fund aggressive deployment of such tests, in order to “protect public health, allow safe in-school instruction, and to restore our economy.” The good news is that the letter has bipartisan support in Congress and is being seriously considered by the incoming Biden Administration as an effective public health initiative to stop the spread of the virus. Rapid Tests, the all-volunteer group directed by Mina advocating for rapid tests to be made legal and widely available, is working on pilot programs in various cities and states and is advising the CDC/HHS teams on the right testing strategy—with frequent, fast antigen testing as a national policy. Fifth, the U.S. needs a “circuit breaker” to break the chains of transmissionI think it was a mistake for President-elect Joe Biden to rule out instituting a nationwide “circuit breaker”—that is, a short-term, national stay-at-home order. At the very least, we need circuit breakers at the state and city level in the highest transmission states. Great Britain and Israel have recently instituted such circuit breakers in conjunction with their vaccination campaigns (the circuit breaker in Great Britain has already driven down transmission everywhere except North West England). There is strong scientific evidence and consensus that community-wide physical distancing can drive down transmission rates, particularly if adherence is high. In many situations where COVID-19 is out of control, there is typically strong public support for stay-at-home orders—this is not surprising, given that people want to be protected from illness and death. In Great Britain, for example, a Jan. 5, 2021 public poll conducted by the public opinion and data company YouGov found that 85% of the public endorse the current lockdown, which was announced on Jan. 4, and 77% think it should have happened sooner. Nevertheless, research has shown that people living in low-income households are much less likely to be able to work from home under such restrictions, pointing to the critical importance of accompanying stay-at-home orders with financial and social support. In July 2020, when daily new cases in the U.S. were just a quarter of what they are now, over 150 scientists, public health experts, and health workers signed a letter urging the country’s federal government to institute a nationwide circuit-breaker. The letter stated: “Right now we are on a path to lose nearly 300,000 American lives by December 1st. Yet, in many states people can drink in bars, get a haircut, eat inside a restaurant, get a tattoo, get a massage, and do myriad other normal, pleasant, but non-essential activities.” We’ve now lost 380,000 Americans. The toll will keep rising unless we start treating COVID-19 as a national emergency that warrants aggressive public health actions.
from https://ift.tt/2Lx2xUf Check out https://takiaisfobia.blogspot.com/ |
Authorhttps://takiaisfobia.blogspot.com/ Archives
April 2023
Categories |
 RSS Feed
RSS Feed
