|
Bruce Willis, the 67-year-old actor and star of classic action movies like Die Hard, is halting his acting career after being diagnosed with the language disorder aphasia. On March 30, his daughter Rumer, ex-wife Demi Moore, and other family members announced the diagnosis on Instagram. “Our beloved Bruce has been experiencing some health issues and has recently been diagnosed with aphasia, which is impacting his cognitive abilities,” the family wrote. “As a result of this and with much consideration Bruce is stepping away from the career that has meant so much to him.” Here’s what experts say about living with the condition and caring for someone who has it. Living with aphasiaSymptoms vary, but generally, aphasia affects people’s ability to speak or comprehend language. Speech, reading, writing, and the ability to listen can be affected. It often occurs suddenly after a stroke or other brain injury damages parts of the brain involved in language expression and comprehension. In other cases, known as primary progressive aphasia, the condition gets worse slowly over time, and patients may develop dementia-like symptoms. Estimates vary, but between 1 and 2 million Americans have aphasia, and almost 180,000 develop the disorder annually. Although it’s most common in older people, who are at greater risk of health events like strokes, it can affect people at any age. “It can be catastrophic,” says Swathi Kiran, director of the Aphasia Research Laboratory at Boston University. “Not being able to say a full sentence, or saying a sentence where the words sound garbled, is extremely frustrating.” It can also cause a person to feel embarrassed or ashamed, “so they would rather choose not to speak anymore than to say something and feel embarrassed about it,” Kiran says. That can lead to social isolation, one of the most emotionally painful potential consequences of aphasia. Patients often know exactly what they’d like to say but may have no way to express it, says Kiran. People with aphasia may need to change their lives dramatically to cope, such as giving up their careers and finding new ways to communicate with loved ones. “I think the most important thing for families to understand is that despite the fact that they don’t seem like themselves, they still are,” says Brenda Rapp, a professor in the department of cognitive science at Johns Hopkins University. “Trying to navigate those often dramatic changes can be really difficult. They really need a lot of support.” Can people recover from aphasia?Although there’s no cure, in sudden onset aphasia, speech therapy can improve patients’ ability to communicate over time. Rapp says that in patients who suddenly develop aphasia, the biggest improvements often happen in the immediate period after the disorder first appears, but patients can continue to improve even years later. “I’ve never actually worked with someone who, if you work concertedly with them, won’t continue to improve,” says Rapp. How well patients recover depends on factors like the severity of the disorder and the way it developed. For some patients, it can even go away completely—like it reportedly did after about a week for Game of Thrones star Emilia Clarke, who developed the disorder after having a brain aneurysm. In other cases, however, patients will continue to cope with symptoms for the rest of their lives. Symptoms in people with primary progressive aphasia, for example, typically continue to get worse, says Kiran. Kiran says there are also promising clinical trials for aphasia, including treatments that stimulate the brain with electricity. Research suggests that treatment can even slow down aphasia in patients with progressive disorders, which is why it’s key that people with aphasia and their loved ones don’t give up, says Kiran. “It’s long and hard, but there’s definitely a road to recovery,” she says. How to support someone with aphasiaPatience is paramount. Kiran recommends slowing down when speaking with someone with aphasia and repeating yourself, if necessary, to make sure that the person understands what you’re saying. She suggests giving them a chance to communicate with you, and encouraging them to draw or use gestures can reveal other modes of communication that may be easier than speech. “Make sure that the person doesn’t feel rushed, because when they feel under pressure, the aphasia definitely gets worse,” says Kiran. Consistently communicating with someone who has aphasia can be essential for helping them to improve and to ward off social isolation. “Every practice they get—whether it’s watching TV together, or drinking a cup of coffee and chatting—is therapy for the brain, and it definitely impacts the outcomes in a positive way,” says Kiran. “What family members have to understand is that they need to support the patient through the recovery process, and never give up.” from https://ift.tt/iW4lbpX Check out https://takiaisfobia.blogspot.com/
0 Comments
The first human genome was mapped in 2001 as part of the Human Genome Project, but researchers knew it was neither complete nor completely accurate. Now, scientists have produced the most completely sequenced human genome to date, filling in gaps and correcting mistakes in the previous version. The sequence is the most complete reference genome for any mammal so far. The findings from six new papers describing the genome, which were published in Science, should lead to a deeper understanding of human evolution and potentially reveal new targets for addressing a host of diseases. A more precise human genome[time-brightcove not-tgx=”true”] “The Human Genome Project relied on DNA obtained through blood draws; that was the technology at the time,” says Adam Phillippy, head of genome informatics at the National Institutes of Health’s National Human Genome Research Institute (NHGRI) and senior author of one of the new papers. “The techniques at the time introduced errors and gaps that have persisted all of these years. It’s nice now to fill in those gaps and correct those mistakes.” “We always knew there were parts missing, but I don’t think any of us appreciated how extensive they were, or how interesting,” says Michael Schatz, professor of computer science and biology at Johns Hopkins University and another senior author of the same paper. The work is the result of the Telomere to Telomere consortium, which is supported by NHGRI and involves genetic and computational biology experts from dozens of institutes around the world. The group focused on filling in the 8% of the human genome that remained a genetic black hole from the first draft sequence. Since then, geneticists have been trying to add those missing portions bit by bit. The latest group of studies identifies about an entire chromosome’s worth of new sequences, representing 200 million more base pairs (the letters making up the genome) and 1,956 new genes. “Since the Human Genome Project [in 2001], we have declared victory a few times over the last two decades,” says Evan Eichler, professor of genome sciences at the University of Washington and another senior author of one of the papers. Eichler, who was also involved in the mapping of that original sequence, says the emphasis of what has been sequenced this time around is different. “While the original goal of the Human Genome Project was to order and orientate every base pair, that couldn’t be achieved because the technology wasn’t sufficiently advanced enough. So we finished the parts that we could finish.” The promise of the new findingsThe newly sequenced regions include previously inaccessible sections such as the centromeres, the tightly wound central portions of chromosomes that keep the long double strands of DNA organized as the strands unwind, bit by bit, to copy themselves and separate into two cells as a single cell divides. These regions are critical for normal human development and also play a role in brain growth and neurodegenerative diseases. “It’s been one of the great mysteries of biology that all eukaryotes—all plants, animals, people, trees, flowers and higher organisms—have centromeres. It’s a really fundamental part of how DNA replicates and how chromosomes organize and how cells divide. But it’s been a great paradox, because while its function has been around for billions of years, it was almost impossible to study because we didn’t have a centromere sequence to look at,” says Schatz. “Now we finally do.” Scientists were also able to sequence the long stretches of DNA that contained repeated sequences, which genetic experts originally thought were similar to copying errors and dismissed as so-called “junk DNA”. These repeated sequences, however, may play roles in certain human diseases. “Just because a sequence is repetitive doesn’t mean it’s junk,” says Eichler. He points out that critical genes are embedded in these repeated regions—genes that contribute to machinery that creates proteins, genes that dictate how cells divide and split their DNA evenly into their two daughter cells, and human-specific genes that might distinguish the human species from our closest evolutionary relatives, the primates. In one of the papers, for example, researchers found that primates have different numbers of copies of these repeated regions than humans, and that they appear in different parts of the genome. “These are some of the most important functions that are essential to live, and for making us human,” says Eichler. “Clearly, if you get rid of these genes, you don’t live. That’s not junk to me.” Deciphering what these repeated sections mean, if anything, and how the sequences of previously unsequenced regions like the centromeres will translate to new therapies or better understanding of human disease, is just starting, says Deanna Church, a vice president at Inscripta, a genome engineering company who wrote a commentary accompanying the scientific articles. Having the full sequence of a human genome is different from decoding it; she estimates that scientists have only deciphered about half of what the human genome does. Future researchThere’s still room for improvement. The new sequence comes from essentially half a human—that is, half of the genetic content normally found in a person’s DNA. Each person has two sets of chromosomes, a maternal and a paternal one. Each of those strands of DNA contain slightly different versions of genes, essentially giving us two genomes. Assembling those two genomes is not a trivial task, and those challenges hampered the original Human Genome Project and led to its missing parts. The sequencing technology at the time could not easily separate the maternal and paternal copies of DNA, so if the scientists attempted to match up certain sections thinking they were working with the maternal chromosome, for example, they might run into areas where they failed to match because they were actually working with the paternal chromosome. “It’s similar to having two puzzles in the same box,” says Phillippy. “You have to sort out what the differences are and reconstruct both.” For this new sequence, the scientists took advantage of a fertilization error in which the resulting embryo contains only paternal chromosomes. The resulting growth was removed and in the early 2000s perpetuated in the lab as a cell line that remained viable despite its abnormal chromosomal content. That made it easier for the teams to assemble the genome because they were essentially working with only a single genetic puzzle to solve. Ultimately, however, researchers will need a more complete human genome with the complete sequences of both maternal and paternal chromosomes. That’s coming soon. Phillippy and others are working with trios of DNA samples from volunteers and their mothers and fathers so that the scientists can separate the maternal DNA from the paternal sequences and essentially assemble two genomes separately. The teams expect to have the so-called diploid human genome sequence completed by the end of the year. Already, says Winston Timp, associate professor of biomedical engineering at Johns Hopkins and a co-author on one of the papers, “the new genome assembly is paying dividends because it provides a more accurate map to understand what data we had from before meant.” That includes finding new variants that might distinguish healthy people from those affected by disease, for example, as well as variants that might put people at higher risk of developing certain diseases. “We’ve discovered millions of genetic variants that were previously not known across samples of thousands of individuals whose genomes have already been sequenced,” says Rajiv McCoy, assistant professor of biology at Johns Hopkins and another co-author. “We will have to wait until future work to learn more about their associations with disease, but a big focus of work now will be on trying to discover new genetic variations that were previously uncharacterized.” Even with the more complete version of the human genome, scientists likely won’t be clamoring to replace the old version, despite its gaps and errors. That’s because the decades of work on human genetics has made that older version far more annotated than the new one—similar to the difference between your favorite copy of book, with your handwritten notes and highlighting in the margins, and a fresh copy from the bookstore. “A genome is only as good as its annotation,” says Eichler. “All the clinical and research labs have built decades worth of data based on the old, gap-filled genome. To redo all of that work for any individual lab would be horrific.” He predicts that many labs will gradually switch over to working with the new genome by comparing smaller datasets first in a test run to see how much richer and more comprehensive the information they generate from the newer genome is. As with the original human genome, the new one is also posted on a public database for any scientist to use. “For now, both genomes will be kept up so there will be no replacement,” he says. In coming years, researchers will also start to generate more of the complete genome, using both maternal and paternal DNA, to help scientists identify the best targets for new therapies and improve understanding of human development and evolution. The more genomes they have, the more potentially important patterns will stand out that could lead to new understanding of human disease and new treatments for them. Ultimately, the goal is that every person would be able to have their complete genome sequenced as part of their medical record, which would allow doctors to compare those sequences to reference ones and determine which variations might be contributing to specific diseases. “This is presenting the world with a whole additional chromosome that we have never seen before,” says Karen Miga, assistant professor in biomolecular engineer at University of California, Santa Cruz and a senior author of one of the papers. “We have new landscapes, new sequences and the opportunity and promise of new discoveries.” The excitement in the genomic and medical community is palpable. “Hallelujah, we finally finished one human genome, but the best is yet to come,” Eichler said during a briefing. “No one should see this as the end, but the beginning of a transformation not only in genomic research but in clinical medicine as well.” from https://ift.tt/EzPyTQ7 Check out https://takiaisfobia.blogspot.com/ Federal health officials are dropping the warning they have attached to cruising since the beginning of the pandemic, leaving it up to vacationers to decide whether they feel safe getting on a ship. Cruise-ship operators welcomed Wednesday’s announcement, which came as many people thought about summer vacation plans. An industry trade group said the move by the Centers for Disease Control and Prevention validated measures that ship owners have taken, including requiring crew members and most passengers to be vaccinated against the virus. The CDC removed the COVID-19 “cruise ship travel health notice” that was first imposed in March 2020, after virus outbreaks on several ships around the world. However, the agency expressed reservations about cruising. “While cruising will always pose some risk of COVID-19 transmission, travelers will make their own risk assessment when choosing to travel on a cruise ship, much like they do in all other travel settings,” CDC spokesman Dave Daigle said in an email. Daigle said the CDC’s decision was based on “the current state of the pandemic and decreases in COVID-19 cases onboard cruise ships over the past several weeks.” COVID-19 cases in the United States have been falling since mid-January, although the decline has slowed in recent weeks, and the current seven-day rolling average for daily new cases in the U.S. is roughly unchanged from two weeks ago, according to figures from Johns Hopkins University. States have rolled back mask mandates, putting pressure on federal officials to ease virus-related restrictions. Outbreaks continue to be reported on cruise ships, which conduct random testing before the end of voyages. On Sunday, a Princess Cruises ship returning from the Panama Canal had “multiple” passengers who had tested positive for the virus. Princess Cruises said all the affected passengers showed mild symptoms or none at all, and that all crew members and passengers had been vaccinated. About a dozen passengers tested positive before the same boat docked in San Francisco in January. Operators are required to tell the CDC about virus cases on board ships. The agency has a colored-coded system to classify ships based on the percentage of passengers who test positive. The CDC said that system remains in place. Cruise-ship operators have complained since the start of the pandemic that their industry has been singled out for a shutdown and then tighter COVID-19 restrictions than others, including airlines. The Cruise Lines International Association said in a statement that the CDC’s decision to remove its health warning “recognizes the effective public health measures in place on cruise ships and begins to level the playing field between cruise and similarly situated venues on land.” Colleen McDaniel, editor in chief of Cruise Critic, a site that publishes review of trips, called the CDC decision big news. “Symbolically it’s a notice of winds of change when it comes to cruising,” she said. “I do think it can convince some of the doubters. What the CDC says does matter to cruisers.” from https://ift.tt/AOCQgHW Check out https://takiaisfobia.blogspot.com/ Common sense and our experience show that prevention is much better than treatment. Gone are the days of children paralyzed from polio. Gone are the days of many children having devastating meningitis. Gone are the days of not being able prevent hundreds of children per year dying from influenza. Such is the value of preventative medicine, especially due to vaccination. Like most things in medicine, we must balance the risks and benefits in making decisions for all patients, especially children. Early in our response to COVID-19, we had to make decisions with incomplete information. Two years of both providing care and conducting research has provided us with extensive information about COVID-19. The medical and scientific communities have also given us clear facts to set the record straight about the risks and benefits of COVID-19 vaccines in children. Sadly, in the U.S. there have been more than 1000 pediatric deaths and more than 7,400 cases of children with the unusual condition called multisystem inflammatory syndrome in children (MISC) due to COVID-19. We also are just learning about long-COVID in children, many of whom have not been hospitalized, and may have extreme fatigue, headaches, and “brain-fog,” which can persist for months after COVID-19. For individuals less than 15 years old, COVID-19 is now the sixth leading cause of death in the U.S.. In comparison, when there is a very bad influenza year, up to 200 children will die and 20,000 hospitalized. In part due to influenza vaccines, deaths due to influenza, are thankfully no longer a top 10 cause of death in children. It is true that children generally fare better with COVID-19 than adults. Patients younger than 18 years old are four-times less likely to need hospitalization than patients older than 65 years and are 65-times less likely to die from COVID-19. However, children do become ill and die from COVID-19. During the recent Omicron wave more than 4.8 million children were infected and more than 30,000 were hospitalized. About 20% of children hospitalized during the recent Omicron wave needed care in intensive care units. The overwhelming majority of these children were not vaccinated. Some people suggest that severe COVID-19, which mean cases needing hospitalization or resulting in death, only affects children who have underlying medical conditions. This is wrong. Nearly 40% of children with severe COVID-19 do not have underlying medical conditions. Conditions that increase a child’s risk for hospitalization include asthma, obesity, and diabetes, to name a few. Importantly, mental health issues, including anxiety and depression, have been found to be associated with severe COVID-19. Recent studies also suggest that more than half of children with previous COVID-19 infections do not have antibodies more than six months after infection, suggesting that prior infection may not be protective. Thus, from a physician’s point of view, to protect children from severe COVID-19 and death, it is impossible for us to say one child should have the vaccine but not another. More and more data show that the current COVID-19 vaccines that have FDA approval for children are very effective in reducing the risk of getting severe COVID-19. Recent peer reviewed studies show these vaccines are 70 to 90% effective in preventing children between 5 and 17 years from being hospitalized if the child has two doses, and another recent study also shows protection against severe illness. In the U.S., for every 100,000 children with COVID-19, 700 to 900 are hospitalized. This means is that for every 100,000 fully vaccinated children, more than 500 hospitalizations will be prevented. It means that pediatric deaths and the risk of MISC and long-COVID will be reduced, as well. Having fewer cases of COVID-19 in children means that there will be less spread of the virus to classmates, teachers and family members, some with medical conditions that put them at greater risk for severe disease. It is always important to balance the value of an effective vaccine with potential side effects. We now have data related to 37 million doses of COVID-19 vaccine given to children between 5 and 17 years old. Non-serious side effects that include dizziness, headache, and fever, occur in about 5 per 10,000 children. Serious side effects, which largely include heart inflammation, or myocarditis, occur in 1 per 1,000,000 vaccine doses. These risks are incredibly low when compared to the risk of hospitalization and death for a child who gets COVID-19. Rightfully, there has been concern raised about the relationship between the COVID-19 vaccine and myocarditis. Here too we have lots of information about this risk. In the highest risk group, teenage boys, the rate of myocarditis after vaccination is 5 per 100,000 vaccine doses, there have been no deaths in individuals less than 30 years and cases generally have a full recovery. In comparison if somebody younger than 16 years old gets COVID-19, the risk of myocarditis is 130 per 100,000. The myocarditis risk for children is thus 25-times higher if you get COVID-19 compared to the vaccine. At a time when the public will be taking a larger role in the control and prevention of COVID-19, it is important that parents, children, and healthcare providers have facts that are accurate. For those facing the decision about whether they should vaccinate their child against COVID-19, consider the facts and speak with your healthcare provider about the risks and benefits. Imagine how many children would now be paralyzed from polio, suffer the consequences of meningitis, or die from influenza, if their parents did not balance the risks and benefits of pediatric vaccines. from https://ift.tt/7VzfHZw Check out https://takiaisfobia.blogspot.com/ When Tanya Herasymova woke up on February 24 to the news that Russia had invaded Ukraine, her first thought was to get underground. If the Russian army began bombing her city Kamianske, close to the separatist region Donetsk, she would be at greater risk in her 4th floor apartment. But there was a problem: none of the city’s bomb shelters were accessible to wheelchair users, leaving Herasymova with nowhere to take cover. “It was a horrible feeling because I knew that I couldn’t go down there by myself. I can’t be alone, I need someone to help me,” Herasymova says. “I realized that the only way for me to be safe during the war was evacuation.” Like many disabled Ukrainians, Herasymova felt excluded from safety and relief efforts designed for the able-bodied population. The NGOs European Disability Forum and Inclusion Europe estimate that there are at least 2.7 million people with disabilities in Ukraine, though other estimates suggest that may be an undercount. Many disabled Ukrainians are more vulnerable to Russian attack, while also at greater risk of abandonment, violence, and discrimination within their own communities. Herasymova and her mother bought train tickets to Lviv, near the Western border of Ukraine, the very next day. The train was packed with people, many standing and without tickets. “For half of our journey it was pitch black without any lights,” Herasymova says, to avoid the train being spotted by Russian jets. “It was really dangerous. There were a lot of people, a lot of children who cried and cried all the way.” After many more hours traveling from Lviv to the border by minibus, they finally crossed into Poland. Speaking to TIME from Denmark, where she is now staying, Herasymova says she wouldn’t have made it to safety without her friend and fellow disabled-rights activist Yuliia Sachuk, who found her accessible accommodation in the country and organized her onward journey. Sachuk had been preparing for the possibility of a Russian invasion since the annexation of Crimea in 2014. As chair of Fight For Right, a Ukrainian non-profit supporting people with disabilities, she understood the importance of coordinating inclusive response strategies to conflict. “I had a feeling that in a situation of war, we [the disabled community] would be the first victims,” Sachuk says. “Maybe not directly, but we would become victims because of our disability. We understood clearly that nobody would come and help us in our efforts to survive.” Sachuk says that for months before the war, Fight For Right tried to coordinate with authorities to develop plans to help disabled people evacuate. The organization’s volunteers were ready—they had received donations through GoFundMe, but they needed help in scaling up. But no help came, Sachuk says. “In Ukraine we still don’t have a systemic approach to help different priorities groups, elderly people, people with disabilities, children.” 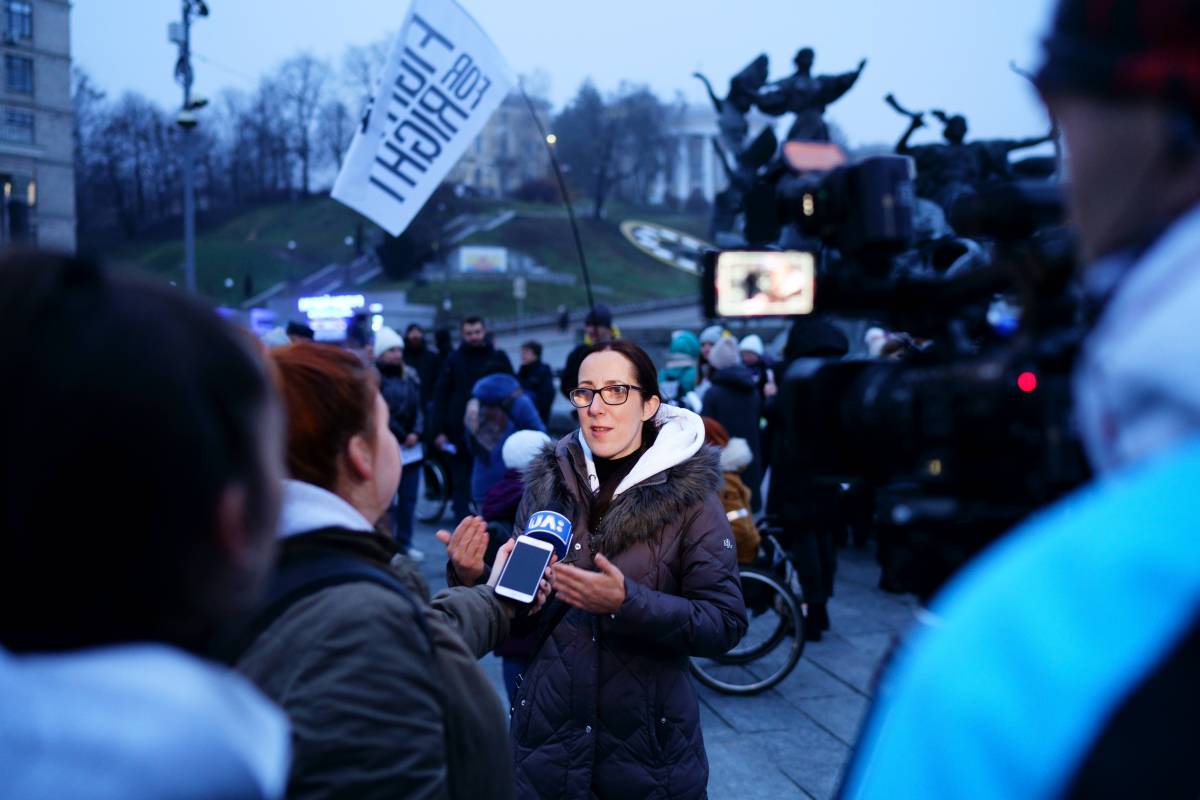
Feeling abandoned by both the state and humanitarian aid groups, disabled Ukrainians have urgently mobilized to help their own communities. Drawing on the strength of pre-existing grassroots networks in the country, activists have coordinated with disabled communities abroad at astonishing speed. Already, Fight For Right’s team of 40 volunteers—many of whom are disabled themselves—have helped 400 people flee the country. The need for solidarity in disabled communities has become ever more clear as the invasion has progressed, stripping away formal support structures and igniting latent prejudices. In a 2020 report on disability rights in Ukraine, the pan-European human rights NGO Council of Europe found that disabled people are often excluded from Ukrainian society because of negative stereotypes, legal and workplace discrimination, and high levels of institutionalization. The war has exacerbated these issues, resulting in what Yannis Vardakastanis, chair of the International Disability Alliance, called “a humanitarian crisis within a crisis.” In some cases, a lack of education and understanding of disabilities has made it difficult for disabled Ukrainians to seek help or safely evacuate. Oleksandr Nikulin and his partner are HIV-positive—they are excluded from government measures which ban men of conscription age from leaving Ukraine. Yet, after a 16 hour trip to the border between Ukraine and Slovakia, they found themselves having to explain their disability to the military. “On our first attempt at the border, a guard got onto our bus and said, ‘You are a man, what are you doing here?’” Nikulin says. They explained they had certificates proving their health exemption from the army. “But the guard said, ‘It doesn’t matter, you are a man, go back.’” After several more failed attempts, Nikulin and his partner met a volunteer who took them to the border police and argued successfully for their safe passage. Still, the experience left Nikulin shaken. “It was so awful because I didn’t understand why,” he tells TIME from Frankfurt, Germany, where he is staying with a friend. “I’m not a criminal, I’ve got documents. I don’t know about war or how to kill people. I can be more useful helping other people with disabilities to evacuate from Ukraine.” Ukrainians with invisible disabilities, like Nikulin, often face even greater levels of misunderstanding and discrimination. 61-year-old Raisa Kravchenko was forced to leave Kyiv with her 28-year-old son, who has an intellectual disability, after the start of the Russian attack. They moved to Kravchenko’s home town 60 miles west and have tried to establish a routine to make her son feel comfortable. They go on walks together every evening, but she can’t control how other people react to him. “There are military checkpoints at the entrance and the exit of the town,” Kravchenko says. “He entered a checkpoint and he was told to stop by the army but he didn’t. And so they shot. Thank God, they were shooting into the air, but they called the police who brought him home.” This has happened three times, she says. “The police say why don’t you control him? And I tell the police: try and tell the wind where to blow.” Now, her son is often afraid when they go out in the town. Kravchenko, who has a physical disability herself, had to make the same devastating decision many disabled people and their families were forced to make. She knows her son wouldn’t cope in a refugee camp or in an unfamiliar environment, and she worries she would fall ill if subjected to a long journey out of the country. So, she and her son will stay in Ukraine. They also struggle to get to bomb shelters when the alarm sounds—so they’ve decided to stay put. “By ignoring all these alarms I have a better chance of survival but if I react and go to the cellar, I could definitely have either a stroke or something,” says Kravchenko, noting the sound of a bomber plane passing overhead. “I’m a kind of fatalist,” Kravchenko says. “Why should I spoil the rest of my life? I don’t know how long I’m going to live. Why should we rush and be in crowded places and suffer?” Kravchenko has spent decades improving the lives of disabled Ukrainians and their families. Dissatisfied with the state’s preference for caring for people with intellectual disabilities in institutions, Kravchenko founded the VGO Coalition, an alliance of 118 local NGOs with the aim of improving policies and support for the intellectually disabled. As leader the local NGO in her area, she successfully lobbied the local authorities in Kyiv to establish a day center for adults with intellectual disabilities. It provided a hub for their guardians—mostly mothers—to meet and share support. Having that network was “life changing,” Kravchenko says. “We brought up a new generation, a different generation of people with intellectual disabilities with an absolutely different quality of life. They were able to be in the city, to communicate, to do meaningful activities. They had friends, sometimes they fell in love and some of them married.” The center was forced to close when war broke out. Now, cut off from the group, Kravchenko has had to find different ways to communicate with other mothers. Some of them have a Viber group chat, where they urgently exchange messages and updates from around Ukraine. One day, Kravchenko received news that a woman and her son who had cerebral palsy were caught in an explosion. The son was badly wounded. His mother had to watch him die for two days, unable to reach help. The situation is clearly taking its toll on Kravchenko, but she hasn’t stopped trying to help in whatever way she can. The VGO Coalition has so far received €20,000 ($22,000) in donations from Inclusion Europe, an international NGO supporting people with intellectual disabilities. Many of the mothers live in rural areas, and don’t have cell phones or bank cards. Yet, word has still spread through the network, and the coalition has distributed the cash through relatives and neighbors. The VGO Coalition, like Fight For Right, is driven by the same community of people who it is trying to support. Katarzyna Bierzanowska, a Polish activist who is helping Fight For Right secure accessible accommodation for disabled refugees in Poland, worries that the burden to help others falls disproportionately on disabled volunteers. “We do not need exhausted heroes,” she says. “We need ready volunteers.” Despite having medical and psychological needs themselves, many disabled volunteers feel they can do the work better than anyone else. “We know how to talk to people, how to make them more confident because we have the same experience,” Sachuk says. Herasymova agrees that the ability to relate to others is vital. “When I say I use a wheelchair and I was evacuated, they think ‘okay if you can, maybe I can do this too.’” While their colleagues and other disabled people remain in Ukraine, the disabled evacuees will continue to help from afar. They still struggle to process the reality of the situation. “We continue to live there. Physically we’re here, but our thoughts and minds are in Ukraine,” Sachuk says. Although she managed to escape with her son, her husband and parents are still living in a war zone. “Of course, I feel safe,” Nikulin says from Frankfurt. “But happy? I don’t know. Because many people with disabilities are still in Ukraine. I can’t believe that war is in my country in the 21st century. I still can’t imagine it.” With no idea of if or when they will ever be able to return, Sachuk and Herasymova are finding comfort within their disability network abroad, which is stronger now than it ever has been before. “I have worked in this area for many years,” Sachuk says, “but I have never seen such unity and solidarity among the disabled community.” from https://ift.tt/fvyJhaV Check out https://takiaisfobia.blogspot.com/ A few days after the Russian invasion of Ukraine, I received an unusual note on Twitter. A Syrian man introduced himself as Mustafa Kayyali. “We are a group of medical doctors with specialization in paramedics, trauma, and war medicine,” Mustafa wrote. “We have suffered from the aggression of Russian forces for the last 8 years, and we trained people to deal with urgent cases, and how to save their lives. We would like to help Ukraine and its people.” He made it clear Syrian doctors had unique experience with treating victims of chemical weapons attacks. Chemical weapons have been used repeatedly against civilians in Syria by the dictator Bashar al-Assad’s army and the Russian forces that support him. I passed Mustafa’s message to my contacts. Two weeks later I was informed that the first training of Syrian doctors for Ukrainian medics had been conducted. More followed, and as of now, several thousand Ukrainian doctors have been trained by Syrian medical professionals on how to deal with patients who suffered from the use of chemical and biological weapons. The training sessions are conducted by Dr Abdullah Abdulaziz Alhaji, MD, a specialist in general surgery. He is the president of the Academy of Health Sciences, established in 2011 after the start of war in Syria to provide medical training to local doctors and civilians. It currently runs programs in paramedics, nursing and physical therapy. “When the Syrian regime attacked our population, we suffered from the reduction of medical staff. Many doctors were arrested, killed or fled Syria. We established our Academy with short courses lasting 15 days, to provide training on trauma first response. There were no paramedics or emergency specialists before in Syria,” Dr Alhaji explains. “With time, Assad’s war machine became more aggressive—more bombings, more shells, more rockets. The more war went on, the more things we did. Syrian people were suffering from the use of chemical weapons. So we trained our students and taught them how to treat different types of injuries.” The Academy had to move several times because its premises were destroyed by Russian airstrikes. It settled in Idlib, the region near the Turkish border which is currently under control of the opposition forces. “For several months, we have been watching the situation in Ukraine, and we thought that we should help doctors there,” says Mustafa Kayyali, vice-president at Academy of Health Sciences. “Many of my colleagues studied in Ukraine, worked there, and we knew that it is a loving country.”’ He continued, “We are happy to help, because people of Syria and Ukraine are fighting against the same enemy.” It was the Syrian medics’ experience with patients affected by chemical weapons that caught the attention of Ukrainian doctors. As NATO and the U.S. warn that Russia might use such forbidden weapons in Ukraine, there is a growing sense of urgency to prepare. 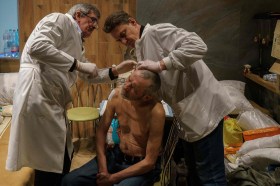
“When Russia started to bomb civilians and residential areas in Ukraine, we lost all illusions that it would stop and would act in the framework of an international humanitarian law,” says Mladena Kachurets, a former deputy health minister of Ukraine and director of the department of personnel development and education at Dobrobut, one of the biggest private clinics in Kyiv. She immediately responded to the Syrian doctors’ idea. “We understood that we have to prepare for the worst, that we have to be ready and cannot ignore a threat of chemical weapons attacks,” Kachurets says. After a successful introductory session brought together a small number of Ukrainian and Syrian doctors by video link, four online lectures were scheduled, open to all medical personnel in Ukraine. The first two took place ten days ago. “There was a huge interest in these lectures, both from doctors and nurses. We advertised the training sessions on social media, and more than 13,000 people expressed their interest. Medical workers from all parts of Ukraine, including medical staff from hospitals in war-torn areas, joined them online,” Kachurets said. Read More: What It Will Take for Ukraine to Win the War “We posted the recordings on Facebook and YouTube so those who were unable to attend live could watch them later. We are now working on Ukrainian translation to make sure every doctor and nurse in Ukraine has access to the lectures.” As of now, the recordings have been watched more than 30,000 times. More are planned, including lectures aimed at the general Ukrainian public. Yuliya Shuklina, MD, a head of otolaryngology department at a big hospital in Kyiv, has been living, along with hundreds of colleagues, on the premises of her hospital since Russia invaded Ukraine, working day and night to treat the wounded and those with chronic diseases. “The war changed all of us,” Dr. Shuklina says, speaking via a videocall during a short break in between treating patients and before a siren, announcing an air raid alert in Kyiv, interrupts our conversation. “In the first days of war, I was very confused. I have 26 years of experience working as an otolaryngologist surgeon, but I have never dealt with sorting of patients and treatment of combat injuries. We are studying and watching a lot of lectures these days.” “‘I studied how to react to a chemical weapons attack at the university, but I forgot it because I never thought I would have to apply it,” she says. “At the session with Syrian doctors, I learned how to determine what kind of a toxin has been used and how to provide help accordingly. This is something very different to a normal injury, when you can determine the impact visually. It is not the case with the victims of a chemical weapons attack, you can’t assess the damage with a naked eye.” “We really appreciate Syrian doctors sharing their first-hand experience. I don’t feel panic anymore hearing about the possibility of a chemical weapons attack. I have an algorithm on how to act. Now I know I will not be confused, I will not be a burden, and will be able to help,” Dr. Shuklina says. “I hope, though, this knowledge will only remain theoretical.” After the sessions Dr. Shuklina went to the hospital management asking them to order antidotes, which vary with the weapon used. “There is a lot of humanitarian assistance, including medicine, delivered to Ukraine these days,” says Kachurets, the former deputy health minister. ”But our doctors are focused on what they need to treat injured people who have multiple trauma, shrapnel wounds, broken limbs. In their lists of necessary supplies, I haven’t seen personal protective equipment to prepare for chemical attacks. I think it should be added to supply lists, and the stockpile of antidotes for different types of toxins must be created in advance.” Kayyali, for his part, is hoping to organize some in-person lectures for Ukrainian doctors in the future. “If there is a safe location somewhere in Ukraine, we would be happy to travel there and do a face-to-face session,’” he says. In the meantime, he has a message for his Ukrainian colleagues: be strong and train more people to provide medical aid. “The war can last long, for years, we Syrians know it. For that reason, you need to train more people, including the general public. People must be trained to treat those affected by chemical weapons and even nuclear weapons,” Kayyali says. “You are dealing with criminals and you can expect anything to happen.” from https://ift.tt/UWuhaDs Check out https://takiaisfobia.blogspot.com/ Telehealth use exploded during the early days of the COVID-19 pandemic, and virtual visits have become common for a wide range of medical services. But this was only possible because of regulations the government relaxed during the public health emergency. Now, as the virus begins to release its grip on the United States, telehealth companies and medical groups are pushing to make these pandemic-inspired changes permanent. Congress recently extended many telehealth changes for five months after the Biden Administration declares an end to the public health emergency, which is currently scheduled to expire on April 16. While it is widely expected that President Joe Biden will extend the public health emergency again, he has been under increasing pressure to unwind pandemic precautions. The congressional extension temporarily eases concerns about a “telehealth cliff” that could abruptly end coverage for virtual treatment, but telehealth lobbyists want to go further. Proponents of telehealth argue that the regulatory changes have done away with outdated, cumbersome limitations and that expanding telehealth improves access and convenience for patients. But some policymakers still have questions about the quality of care telehealth can deliver, the cost of expanding it further, and the potential for fraud in virtual care. “Given how much we still do not know about telehealth with respect to cost, outcomes, quality— whether it is adding costs to the Medicare program or saving Medicare dollars—we believe it would be premature to make these expansions permanent,” says James Matthews, executive director of the Medicare Payment Advisory Commission (MedPAC), which advises Congress on Medicare. MedPAC will collect data in 2021 and 2022 so that it can study what “more of a steady state” of telehealth use looks like compared to 2020 when many people avoided leaving their homes, says Mathews. Telehealth existed before the pandemic, but federal regulations “didn’t really allow for widespread use of the tool,” says Jacqueline Marks, a senior manager at Manatt Health. Among other restrictions, Medicare would only cover telehealth visits for seniors who lived in rural areas and who accessed their virtual visits at qualifying sites, not in their own homes. It also limited the types of providers who could offer telehealth and did not pay providers the same for virtual visits as for in-person ones. Because private insurers and Medicaid programs often follow Medicare’s lead, medical providers could only get reimbursed for telehealth visits in limited circumstances. Once Congress loosened these rules in 2020, telehealth use skyrocketed. Medicare patients used telehealth 88 times more during the first year of the pandemic than they had previously, according to a report from the Department of Health and Human Services Office of Inspector General. Telehealth claims for non-seniors also increased, and telehealth companies saw an influx of cash. Last year, equity funding to telehealth reached nearly $18 billion, according to CB Insights, a 57% increase from 2020. “There is no doubt that telehealth saves lives,” Department of Health and Human Services Secretary Xavier Becerra said at a press conference this month. “We would be really closing our eyes to a new form of quality health care if we did not expand authorities for telehealth to be available to Americans.” Telehealth has rare bipartisan support and some powerful champions in Congress. But with concerns about quality, cost, and potential fraud lingering, the industry is ramping up its lobbying efforts to make sure that its gains don’t slip away. And in the meantime, millions of Americans are wondering what their health care will look like in the future. “This has changed our entire healthcare ecosystem forever,” Marks says. “I think everyone’s just trying to figure out right now, how do we go forward?” 
An increase in lobbyingTelehealth has a wide array of advocates on both sides of the aisle pushing for its expansion, even in a time when Congress is often struggling to pass bills amid a fierce partisan divide. Lawmakers like Democratic Senator Brian Schatz of Hawaii and Republican Senator Tim Scott of South Carolina have each championed bipartisan telehealth legislation, and everyone from digital health companies to hospitals, physicians, insurers, and non-health related employers want to see telehealth stick around. Traditionally, telehealth hasn’t had a unified lobbying powerhouse. While groups such as the American Hospital Association (AHA), the American Medical Association (AMA) and Pharmaceutical Research and Manufacturers of America (PhRMA) are used to spending millions of dollars each year to lobby for their preferred issues, the American Telemedicine Association spent a more modest $120,000 on lobbying last year. But those other interest groups have increased their lobbying on telehealth during the pandemic, uniting to leverage diverse factions behind similar goals. They want the loosened telehealth rules made permanent, and they also want Medicare to continue to pay for telehealth visits at the same level as it pays for in-person visits, to extend coverage for both video and audio-only telehealth visits, and to allow providers to practice across state lines beyond the pandemic. In December 2021, major players such as the AMA and AHA teamed up with Teladoc, AARP, and corporate giants like Amazon, Walmart, and CVS to form a new coalition called Telehealth Access for America, aimed at pushing for more permanent expansions of telehealth. In January, the American Telemedicine Association, which is also part of the coalition, launched its own advocacy arm called ATA Action to increase its advocacy efforts. Kyle Zebley, executive director of ATA Action, said the group’s lobbying footprint will grow this year as it coordinates priorities among those with wide ranging interests. “You can expect us to be significantly more invested in the direct technical lobbying efforts,” he says. Challenges aheadBut for all the support being expanding telehealth, some lawmakers and industry experts are wary of making sweeping changes to how Americans see their doctors without more data. One of the most important areas experts want to evaluate is the quality of care that telehealth delivers. “What has been the impact on quality? Have there been any concerns? Has it improved quality? We don’t really know,” says Ateev Mehrotra, associate professor of health care policy and medicine at Harvard Medical School. The omnibus package in which Congress gave telehealth changes a five month extension also directed MedPAC to study telehealth expansion, and the commission plans to look at questions around quality as part of its work. To see how telehealth affects patient outcomes, Mathews says MedPAC will aim to compare hospitalizations and emergency department visits from 2019 when there was less telehealth use to those visits in 2022 and 2023. Collecting this data would likely require telehealth to stay around for a year or two beyond whenever the public health emergency ends. MedPAC’s report is due in June of 2023, but MedPAC favors a temporary extension for at least that time rather than permanent rule changes. If Congress continues temporary extensions until then, that could be “frustrating” for telehealth companies and providers, says Thomas Ferrante, a health care lawyer at Foley & Lardner and a member of the firm’s telemedicine team. “That’s very hard for long term planning, it’s very hard for an allocation of capital resources. And it’s hard to really message to your patients,” he says. Telehealth advocates argue the push for more data needs to be balanced with an imperative for speed. “What we don’t want to do is study this thing to death and leave people out, forget the human component, tell the people who are using it, who are benefiting from it, that they have to sit on the sidelines while we crunch some more numbers,” says Claudia Tucker, senior vice president of government affairs at Teladoc. Concerns about cost also present a barrier. MedPAC is researching whether telehealth is taking the place of in-person visits, or if it’s supplementing them, which could add costs to the government program, Matthews says. And MedPAC will also be studying potential fraud in telehealth use for Medicare patients. Other congressional advisers have raised concerns too. The Congressional Budget Office found in December 2020 that ending geographic restrictions for coverage of mental health through telehealth would add costs to Medicare, and the Government Accountability Office told the Senate Finance Committee last spring that expanding telehealth could lead to higher costs and potential fraud. But even if the public health emergency and its flexibilities end this year, the telehealth advocates see Congress’ five month extension as a chance to keep making their case in every way they can. Health care company Amwell has conducted polling about consumer interest in telehealth that it aims to use in its advocacy, and Teladoc says it has received interest from patient advocacy groups that want to help push for expanding telehealth policies. “People have tasted what it feels like when health care can work on their own terms in their environment,” says Dr. Roy Schoenberg, president and CEO of Amwell. “Because these technologies so profoundly changed the experience of the American patient, I think this is a very, very different kind of dynamic. I don’t think you can stop it at this point.” from https://ift.tt/7YMwRtH Check out https://takiaisfobia.blogspot.com/ Two years into the pandemic, the Biden Administration has launched a virtual hub to help Americans find COVID-19 prevention and treatment resources—including masks, tests, and vaccines—in their communities. The website, COVID.gov, consolidates several existing initiatives into what President Joe Biden described during a press briefing on March 30 as a “one-stop shop.” The site includes links for ordering free at-home rapid tests; locating free, high-quality N95 masks; finding vaccines and treatments; and assessing current COVID-19 risk levels in specific counties, based on U.S. Centers for Disease Control and Prevention metrics. “The bottom line: no longer will Americans need to scour the internet to find vaccines, treatments, tests, or masks,” Biden said during the briefing. “It’s all there.” One of the website’s central features is its promotion of Biden’s “test-to-treat” program, which is designed to improve access to antiviral drugs that can reduce the severity of disease for high-risk people. In theory--though not always in practice—the program enables someone who tests positive at a pharmacy or health center to receive treatment on the spot, for free. COVID.gov includes a site locator for facilities taking part in the test-to-treat program, including retail pharmacies, community health centers, and clinics affiliated with Veterans Affairs and the Indian Health Service. COVID.gov is available in English, Spanish, and Simplified Chinese. The same resources are also available in additional languages through the Administration’s telephone hotline at 1-800-232-0233. While announcing the website’s launch, Biden again implored Congress to authorize extra pandemic funding. A Congressional spending bill passed in March did not include additional money for COVID-19 relief, and the shortfall has forced the Biden Administration to cut back on treatment and vaccine purchases, Biden said. The government has also had to curtail a program that reimburses providers who test or treat people without insurance, meaning some uninsured people now have to pay out-of-pocket for COVID-19 tests. Barring extra funding, the same will soon be true of some fees associated with getting COVID-19 vaccines. Biden warned during the press briefing that supplies of COVID-19 drugs, vaccines, and tests may run out in the coming months without more money. “We’re already seeing the consequences of Congressional inaction,” he said. “This isn’t partisan; it’s medicine.” After his remarks, Biden received a fourth COVID-19 vaccine, just a day after the U.S. Food and Drug Administration authorized second mRNA boosters for adults ages 50 and older and certain immunocompromised individuals. “It didn’t hurt a bit,” he said. from https://ift.tt/nwDbcLk Check out https://takiaisfobia.blogspot.com/ (Grand Portage, Minn.) — To administer this COVID test, Todd Kautz had to lay on his belly in the snow and worm his upper body into the narrow den of a hibernating black bear. Training a light on its snout, Kautz carefully slipped a long cotton swab into the bear’s nostrils five times. For postdoctoral researcher Kautz and a team of other wildlife experts, tracking the coronavirus means freezing temperatures, icy roads, trudging through deep snow and getting uncomfortably close to potentially dangerous wildlife. They’re testing bears, moose, deer and wolves on a Native American reservation in the remote north woods about 5 miles from Canada. Like researchers around the world, they are trying to figure out how, how much and where wildlife is spreading the virus. Scientists are concerned that the virus could evolve within animal populations—potentially spawning dangerous viral mutants that could jump back to people, spread among us and reignite what for now seems to some people like a waning crisis. The coronavirus pandemic has served as a stark and tragic example of how closely animal health and human health are linked. While the origins of the virus have not been proven, many scientists say it likely jumped from bats to humans, either directly or through another species that was being sold live in Wuhan, China. And now the virus has been confirmed in wildlife in at least 24 U.S. states, including Minnesota. Recently, an early Canadian study showed someone in nearby Ontario likely contracted a highly mutated strain from a deer. “If the virus can establish itself in a wild animal reservoir, it will always be out there with the threat to spill back into the human population,” said University of Minnesota researcher Matthew Aliota, who is working with the Grand Portage Reservation team. E.J. Isaac, a fish and wildlife biologist for the reservation that’s home to the Grand Portage Ojibwe, said he expects the stakes to get even higher with the start of spring, as bears wake from hibernation and deer and wolves roam to different regions. “If we consider that there are many species and they’re all intermingling to some extent, their patterns and their movements can exponentially increase the amount of transmission that could occur,” he said. Into the wildTheir research is meant to ward off such unwelcome surprises. But it carries its own set of risks. Seth Moore, who directs the reservation biology and environment department, recently almost got bitten by a wolf. And they sometimes team with a crew from the Texas-based company Heliwild to capture animals from the air. One chilly late-winter afternoon, the men climbed into a small helicopter with no side doors that lifted above the treetops. Flying low, they quickly spotted a deer in a forest clearing. They targeted the animal from the air with a net gun and dropped Moore off. Wind whipped at his face as he worked in deep snow to quickly swab the deer’s nose for COVID, put on a tracking collar and collect blood and other biological samples for different research. The men capture moose in much the same way, using tranquilizer darts instead of nets. They trap wolves and deer either from the air or on the ground, and trap bears on the ground. They knew of the young male bear they recently tested because they had already been tracking it. To get to the den, they had to take snowmobiles to the bottom of a hill, then hike a narrow, winding path in snow shoes. When Kautz crawled part-way into the den, a colleague held his feet to pull him out quickly if necessary. The team also gave the animal a drug to keep it sleeping and another later to counteract the effects of the first. To minimize the risk of exposing animals to COVID, the men are fully vaccinated and boosted and get tested frequently. The day after testing the bear, Isaac packed their samples to send to Aliota’s lab in Saint Paul. The veterinary and biomedical researcher hopes to learn not just which animals are getting infected but also whether certain animals are acting as “bridge species” to bring it to others. Testing may later be expanded to red foxes and racoons. It’s also possible the virus hasn’t reached this remote location—yet. Since it’s already circulating in the wilderness of Minnesota and nearby states, Aliota said it’s only a matter of time. Looking for mutantsClose contact between humans and animals has allowed the virus to overcome built-in barriers to spread between species. To infect any living thing, the virus must get into its cells, which isn’t always easy. Virology expert David O’Connor likens the process to opening a “lock” with the virus’ spike protein “key.” “Different species have different-looking locks, and some of those locks are not going to be pickable by the key,” the University of Wisconsin-Madison scientist said. But other locks are similar enough for the virus to enter an animal’s cells and make copies of itself. As it does, it can randomly mutate and still have a key that fits in the human lock. That allows it to leap back to humans through close contact with live animals, scientists believe. Although spillback is rare, it only takes one person to bring a mutated virus into the realm of humans. Some think the highly mutated omicron variant emerged from an animal rather than an immune-compromised human, as many believe. Virologist Marc Johnson of the University of Missouri is one of them, and now sees animals as “a potential source of pi,” the Greek letter that may be used to designate the next dangerous coronavirus variant. Johnson and his colleagues found strange coronavirus lineages in New York City sewage with mutations rarely seen elsewhere, which he believes came from animals, perhaps rodents. What scientists are most concerned about is that current or future variants could establish themselves and multiply widely within a reservoir species. One possibility: white-tailed deer. Scientists found the coronavirus in a third of deer sampled in Iowa between September 2020 and January 2021. Others found COVID-19 antibodies in a third of deer tested in Illinois, Michigan, New York and Pennsylvania. Infected deer generally have no symptoms. Testing in many other wild species has been limited or absent. “It’s possible that the virus is already perhaps circulating in multiple animals,” said virology expert Suresh Kuchipudi of Pennsylvania State University, an author of the Iowa deer study. If unmonitored, the virus could leave people “completely blindsided,” he said. Can it be stopped?Ultimately, experts say the only way to stop viruses from jumping back and forth between animals and humans—extending this pandemic or sparking a new one—is to tackle big problems like habitat destruction and illegal wildlife sales. “We are encroaching on animal habitats like we have never before in history,” Aliota said. “Spillover events from wild animals into humans are, unfortunately I think, going to increase in both frequency and scope.” To combat that threat, three international organizations—the United Nations Food and Agriculture Organization, the World Organization for Animal Health and the World Health Organization—are urging countries to make COVID surveillance in animals a priority. In Grand Portage, Aliota’s collaborators continue to do their part by testing as many animals as they can catch. With icy Lake Superior sparkling through the evergreens, Isaac slipped his hand beneath the netting of a deer trap. A colleague straddling the animal lifted its head off the snowy ground so that Isaac could swab its nostrils. The young buck briefly lurched its head forward, but kept still long enough for Isaac to get what he needed. “Nicely done,” his colleague said as Isaac put the sample into a vial. When they were finished, they gently lifted the trap to let the deer go. It bounded into the vast forest without looking back, disappearing into the snowy shadows. from https://ift.tt/j3FLxiv Check out https://takiaisfobia.blogspot.com/ Two years after the pandemic began, we finally have a good understanding of how COVID-19 is transmitted: some infected people exhale virus in small, invisible particles (aerosols). These do not fall quickly to the ground, but move in the air like cigarette smoke. Other people can get infected when breathing in those aerosols, either in close proximity, in shared room air, or less frequently, at a distance. But the journey to accepting the overwhelming scientific evidence of how COVID-19 spread was far too slow and contentious. Even today, the updated guidance and policies of how to protect ourselves remain haphazardly applied, in part because of one word: “airborne.” This fundamental misunderstanding of the virus disastrously shaped the response during the first few months of the pandemic and continues to this day. We still see it now in the surface cleaning protocols that many have kept in place even while walking around without masks. There is a key explanation for this early error. In hospitals, the word “airborne” is associated with a rigid set of protective methods, including the use of N95 respirators by workers and negative pressure rooms for patients. These are resource-intensive and legally required. There was a shortage of N95s at the beginning of the pandemic, so it would have been difficult, if not impossible, to fully implement “airborne” precautions in hospitals. Due to its specific meaning in hospitals and longstanding misunderstanding about how airborne transmission actually happens and underappreciation of its importance, public health officials were wary of saying the word, even though it would have been the clearest way to communicate with the public about transmission and how to control it. As one article put it, “They say coronavirus isn’t airborne–but it’s definitely borne by air.” Because the word “airborne” was off-limits, it felt like we showed up to a basketball game thinking it was a boxing match. During a press conference in February 2020, the Director-General of the World Health Organization said, “This is airborne, corona is airborne,” although a few minutes later, he corrected himself, “Sorry, I used the military word, airborne. It meant to spread via droplets or respiratory transmission. Please take it that way; not the military language.” In March, W.H.O. denied outright that Covid-19 was airborne, posting on social media, “FACT: #COVID19 is NOT airborne,” and calling it “misinformation.” We and our colleagues, scientists and engineers who have studied airborne particles for our entire careers, met with W.H.O. in April 2020 to express our concern that airborne transmission was important in the spread of COVID-19. W.H.O. vehemently rejected our suggestion and painted us as trespassers who did not understand what was happening in hospitals. Likewise, the U.S. Centers for Disease Control studiously avoided using the word and instead tied itself in knots trying to describe transmission. Eventually we started to be heard, but the initial period of the pandemic, when stopping the virus was more feasible, and when everyone was paying sharp attention and was willing to adapt new protective behaviors, was lost. Protections that are nearly useless for this virus, such as surface disinfection and handwashing became deeply ingrained. Billions were spent on plexiglas barriers that may increase transmission. Gradually over the past two years, the two agencies have recognized transmission of the virus through the air, and in December 2021, W.H.O. finally used the word “airborne” on one webpage to explain how COVID-19 spreads between people, although the organization’s social media posts continue to completely avoid the word. The word remains verboten for C.D.C. We are accustomed to talking freely about diseases that are waterborne, foodborne, bloodborne, or vector-borne. If even President Trump knew in February 2020, “You just breathe the air, and that’s how it’s passed,” why wasn’t the public told clearly the virus was airborne? According to conventional wisdom in the medical community, colds and flus were spread mainly by large droplets, and there was a very high bar to prove a disease was airborne. Historically, airborne transmission has been associated with long distances, beyond a range of 6 feet. Such occurrences are difficult to prove for a rapidly spreading virus, as our observations at that point were limited by rules restricting contact tracing to those within 6 feet due to long standing practice. Read More: How to Clean Indoor Air Properly Against COVID-19 Ideas about how transmission works have been dominated by observations in hospitals, which tend to have excellent ventilation and therefore a lower risk of airborne transmission. Good ventilation removes the virus from the air and prevents it from accumulating over time, reducing the likelihood that someone will breathe in enough of it to become infected. As the pandemic evolved and we and our colleagues endeavored to show that all evidence pointed toward airborne transmission, public health leaders began to acknowledge that it could occur in special situations, namely those with poor ventilation. What they might not have realized is that, relative to hospitals, nearly all other buildings—homes, schools, restaurants, and many workplaces and gyms—would qualify as such special situations. In these buildings, indoor air might be replaced with outdoor air once or twice per hour, whereas in hospitals the ventilation rate is at least 6 air changes per hour in patient rooms and 15 in operating rooms. We have studied viruses in the air long enough to understand that “airborne” is a trigger word in healthcare, yet we found it maddening that the word was off-limits during a pandemic. It was okay to talk about aerosols but not to say “airborne” or explain “like smoke,” even though it would have been far more effective for communicating with the public. To the general public, the word simply means something that is in the air, like a kite or pollen. The situation is like trying to explain a carcinoma diagnosis to a patient without using the word “cancer.” Using the word earlier in the pandemic would have facilitated the implementation of more effective mitigation strategies, such as Japan’s 3Cs—avoid close contact, avoid crowds, and avoid closed, poorly ventilated settings—instead of focusing so much on 6-foot distancing and surface cleaning. It also might have reduced resistance to masks. The field of medicine should not have a monopoly on the word airborne. One way to reduce the chance for confusing communication in the future is to change the designation of different categories of precautions for infection prevention and control in hospitals. Rather than affixing specific words to the current categories—contact, droplet, and airborne—hospitals could assign numerical levels (e.g., 1, 2, 3, 4…) for different sets of precautions, such as those used for biosafety procedures in laboratories. This would avoid the association of certain words with regulatory requirements, freeing the words for general use. From the outside, it is easy for us to see that a traditional, medical-centric approach has contributed to a sclerotic response to the airborne spread of Covid-19. We realize this sounds self-serving, but we need to recognize that broader expertise beyond medicine is required for public health, and certainly for combating an airborne virus. We, the two authors, know almost nothing about what happens to a virus when it’s inside your body nor how to treat it, but we do know how a virus behaves in the environment—whether indoors or outdoors—and how to remove it. This is the domain of environmental engineering, mechanical engineering, atmospheric science and aerosol science, fields devoted to understanding the movement and control of gases and particles in the environment. This type of expertise has been sidelined in our pandemic response. We are thrilled to see the White House recognizing airborne transmission and the importance of indoor air quality through the Clean Air in Buildings Challenge as part of the National COVID-19 Preparedness Plan. While this is a good start, regulations and more funding will be needed to achieve clean air in all our buildings and fully realize its benefits in the long run. And because building operations are responsible for about 30% of greenhouse gas emissions, we must figure out how to do this efficiently. We can’t let “airborne” be a dirty word. Instead, increased public attention to the air we breathe is an opportunity to dedicate science, technology, and policy tools to ensure that the air in our buildings is clean and healthy. from https://ift.tt/rqWjtkY Check out https://takiaisfobia.blogspot.com/ |
Authorhttps://takiaisfobia.blogspot.com/ Archives
April 2023
Categories |
 RSS Feed
RSS Feed
