|
Euphoria—the most tweeted-about TV show of the decade in the U.S.—has thrust teenage drug use into the cultural spotlight. The HBO show follows 17-year-old Rue Bennett, a sweet but troubled teen played by Zendaya, as she navigates a deepening drug use disorder. It’s not pretty. Rue takes the powerful opioid fentanyl, injects morphine, and drags around a suitcase filled with thousands of dollars worth of drugs (a stash she can’t resist dipping into). Meanwhile, she rips apart her life: tearing through her house, ransacking strangers’ homes, and screaming at the people she loves the most. Yet the show’s season two finale, which aired on Feb. 27, ends on a hopeful note for Rue’s recovery. Here’s what addiction experts who watch the show say that Euphoria gets right about teen drug use and treatment—and where it misses the mark. What Euphoria gets right: Drug use isn’t rare among teensThe show has sparked controversy over how it portrays teen drug use. In January, D.A.R.E.—the Drug Abuse Resistance Education program--criticized the show for “glorify[ing]” high school drug use and making it seem “common and widespread in today’s world.” But drug use is not uncommon among high school students today. In the U.S., about 1.6 million kids ages 12 to 17—6.3% of the adolescent population—had substance use disorder in 2020, according to the Substance Abuse and Mental Health Services Administration (SAMHSA). “That’s a huge problem,” says Dr. Lynn Fiellin, professor of medicine at the Yale School of Medicine and Child Study Center, who is trained in addiction medicine and behavioral health (and who is a fan of the show). The problem seems to be growing, too; in 2020, millions more kids tried drugs for the first time. “Euphoria depicts exactly what is going on,” she says. Rue takes many different types of drugs throughout the show—from marijuana to Xanax—but she most commonly uses opioids. This is a major concern, because opioid use is often deadly in young people: in 2020, nearly 6,000 youth ages 15 to 24 died of an overdose involving opioids in the U.S, amounting to 84% of all drug overdose deaths in that age group, according to National Center for Health Statistics data. The show excels at portraying the “chaos” that can happen when a young person’s substance abuse gets out of control, as Rue’s does, says Fiellin. In the first episode, Rue’s little sister discovers her overdosing in a puddle of her own vomit; the two seasons follow Rue as her drug use continues to wreck her closest relationships. What Euphoria gets wrong: Treatment options aren’t so limitedSomething the program does less well is showing the range of options people have to help them recover from substance use disorder. While psychiatrists and experts agree that Rue—or someone like her—faces a difficult recovery, she hasn’t explored all of her options, or even the best ones. On Euphoria, Rue has participated in two main treatments: inpatient rehab in season one and Narcotics Anonymous (NA)—which, like Alcoholics Anonymous, is a 12-step-model emphasizing spirituality and abstinence from substances. While these programs can help some people, they’re not for everyone, and come with certain drawbacks, psychiatrists say. Rehab programs can vary in quality and be very expensive, while NA can sometimes alienate people who are less religious—like Rue, who declares she doesn’t believe in God. However, NA does enable Rue to develop a powerful connection with her sponsor, Ali Muhammad, who pushes her to change the way she looks at the world. Fiellin says that relationships like this with “folks who are supporting you and listening,” can be essential for recovery. That proved to be true for Rue. Dr. Sulman Aziz Mirza, a psychiatrist who specializes in adult, child and adolescent, and addiction psychiatry (and who watches the show), says he wishes Rue’s storyline would show her trying different options that could help her recover. “There’s just an inevitable [sense] that we’re going to see Rue die” in future seasons, he says. “I’m hoping that at least there’s some acknowledgement that, ‘Hey, there are options there.’” So far, the show has not depicted one of the most successful treatments for opioid-use disorder: medications like buprenorphine. According to Robert Miranda, professor of psychiatry and human behavior at Brown University (who knows about the show’s emphasis on drug use but does not watch it), buprenorphine reduces cravings and withdrawal symptoms by activating the same parts of the brain as opioids, but doesn’t trigger the same “high” or side effects. “I think that’s a missed opportunity to highlight a treatment like buprenorphine,” says Fiellin. Buprenorphine and other similar medications, including naltrexone and methadone, have been found to reduce opioid use, decrease the risk of overdose, and increase the odds that a patient will stay in treatment, according to the National Institute on Drug Abuse. Taking medication for opioid use disorder “can offer an advantage, an often-needed edge,” says Miranda. “It can offer reprieve from the intense cravings and adverse drug withdrawal symptoms that people face—including many teens—while struggling to reduce their drug use.” Therapy is another option that can be especially effective when paired with medication, Fiellin says. Cognitive behavioral therapy, family therapy, and an approach called motivational interviewing have all been shown to help people with opioid use disorder. Motivational interviewing, a counseling approach in which a counselor talks with a patient about the reasons why they need to change and their reasons for doing so, is designed to help people who are ambivalent about seeking treatment. This strategy might make sense for someone like Rue, who walks out of rehab in the series premiere and declares, “I had no intention of staying clean.” Changing behavior can be an especially “hard sell” for a teenager like Rue, says Dr. Kevin Gray, a professor of psychiatry and behavioral sciences at the Medical University of South Carolina, so motivational interviewing programs can help by “driving them toward motivation, rather than waiting for them to be motivated.” Just as different causes lead people to drug use, different motivations can help individuals recover. Mirza says the key is to find the treatments—and health care providers—that work for each person. ”I could be Harvard trained, and I could have degrees and publications and books and everything like that, but if I can’t connect with the kid that’s in front of me, it doesn’t mean anything,” says Mirza. Rue’s long road aheadAt the end of the season two finale, Rue says in a narration that she stayed clean for the rest of the school year. But psychiatrists who watch Euphoria agree that Rue’s longer path to recovery will not be easy—nor would it be if she were a teen in the real world. People like Rue face many obstacles that make it difficult for their condition to improve, or even for them to survive. For many people, drug use disorder is a chronic condition with which they must continue to cope throughout their lives. “There are some young people who get into really serious trouble with substance use who are able to recover quickly and maintain lifelong sobriety,” says Gray, but others struggle with lifelong addiction. “Just like if somebody had hypertension or diabetes, we don’t expect them to enter a treatment, and then stop the treatment and forever be cured.” One of Rue’s triggers for substance use issues is her struggle with anxiety, panic attacks, and other mental health issues, Fiellin points out. Mental illness and drug use can create a “vicious cycle,” she says: mental illness can push people to use drugs, which in turn can make the condition worse. That means it’s especially important to find ways to treat both issues. “Mental health and addiction are so tightly linked, and there’s so much overlap, that you really cannot address one in a vacuum.” The show also hasn’t explored another major risk for Rue and drug users of all ages in the U.S.: the danger of a drug supply that is contaminated by the highly potent opioid fentanyl, which has been linked to a surge in opioid overdose deaths in the U.S. While Rue is shown taking fentanyl intentionally, she is likely to also encounter it mixed in with another drug without her knowledge, which means that she wouldn’t be able to control her dose. Rhana Hashemi, a researcher who promotes harm reduction education in schools, is critical of Euphoria for making the drug supply seem so simple: Rue and other characters don’t question what they’re taking or selling, and there doesn’t seem to be much concern for whether drugs are mislabeled or adulterated. Though they’re not explored in the show, harm-reduction methods, like Narcan and fentanyl test strips, can help make drug use safer. “Most substances have fentanyl, and dosing the fentanyl is really difficult,” says Hashemi. “That’s why it’s so important to never use alone, to test your drugs, and to have Narcan on hand.” One other major challenge for Rue is that she is a teenager. Access to high-quality treatment can be a major problem for adolescents—especially if, like Rue, they live outside of a city and their family isn’t wealthy. That’s compounded by all the other typical challenges of being a teen: dealing with a developing brain, limited impulse control, and the drive to figure out identity. For anyone, being a teen can be difficult. Layering on substance use disorder can make it seem impossible. However, the silver lining is that teens are still growing and maturing, and their youth gives professionals an opportunity to intervene early in their drug use. Even for someone like Rue, “there’s still so much potential,” Gray says. from https://ift.tt/2lCQYs9 Check out https://takiaisfobia.blogspot.com/
0 Comments
For more than a year, a mask has been as essential at the airport as a boarding pass: you can’t fly without one. But the federal mask mandate for planes, trains, buses, and transit stations including airports is set to expire on March 18, and so far, the government has not announced plans to extend it. That could change. The Transportation Security Administration has extended the face mask requirement several times so far. But as Omicron cases decline nationwide and states drop their own mandates, it’s not clear whether the policy will be renewed again. The U.S. Centers for Disease Control and Prevention on Feb. 25 relaxed its own guidance around masking and currently says indoor masking is not necessary for about 70% of the population. Though that guidance is separate from the travel mandate, it signals a growing acceptance for going bare-faced. For months, airline executives have questioned the need for in-flight mask mandates, arguing that the air filtration systems on planes are effective enough to eliminate virtually all airborne pathogens. Representatives for the nation’s largest flight attendant union, however, have said they expect the mandate to be extended, since COVID-19 is still circulating widely and young children remain ineligible for vaccines. It’s not clear yet whether the Biden Administration will extend the transportation mask mandate. But here’s what the research says about wearing masks on airplanes. How dangerous is flying during COVID-19?Throughout the pandemic, there have been documented instances of SARS-CoV-2 (the virus that causes COVID-19) spreading on planes. Still, in-flight transmission happens less frequently than one might expect with such close quarters and shared air. The authors of a research review published in September 2021, which analyzed 18 prior studies on in-flight spread of SARS-CoV-2, concluded that “transmission of SARS-CoV-2 can occur in aircrafts but is a relatively rare event.” A 2020 study conducted for the U.S. Department of Defense—and carried out by researchers from Boeing and United Airlines, among others—found that aircraft ventilation and filtration systems reduced the risk of airborne SARS-CoV-2 exposure by more than 99%. But the study didn’t account for other modes of transmission, such as direct exposure to larger respiratory droplets expelled by an infected person sitting nearby. It also did not consider the effects of walking up and down the aisles or interacting with other passengers. It’s hard to say exactly how risky it is to fly during the pandemic, because lots of variables affect whether SARS-CoV-2 jumps from one traveler to another: everything from how much virus a traveler is carrying to the length of the flight and the vaccination statuses of other people on board. Research has shown that risk even changes depending on whether an infectious person is talking—and therefore expelling more respiratory particles—or just breathing. The flight may not even be the riskiest part of a trip, adds Dr. Aisha Khatib, who is chair of the International Society of Travel Medicine’s Responsible Travel interest group and has studied SARS-CoV-2 transmission on flights. (The International Society of Travel Medicine’s members include travel industry employees, as well as researchers and medical experts.) There’s plenty of potential for exposure in the airport, such as when people remove their masks to eat or drink at the gate, she says. That alone makes wearing a mask a good idea while traveling. Should I wear a mask on a plane?Right now, it’s required. But you might want to continue masking up on planes even if the mandate expires. Research has shown that wearing a mask in public indoor spaces reduces your risk of later testing positive for COVID-19. On planes, the air is frequently filtered, which helps keep the risk of in-flight transmission fairly low, Khatib says. But that risk drops even lower, she says, when good ventilation is accompanied by precautions including masking, symptom screening (like pre-flight temperature checks), and social distancing. In a paper published in March 2021, researchers developed a model for predicting the infection risk aboard a plane. The most extreme scenario they considered was a 12-hour flight in which passengers were not wearing masks and one infected person was seated in tightly packed economy class. Under these conditions, the authors estimated that other economy passengers had an average infection risk of up to approximately 11%—but for someone seated in very close proximity to the infected person, the risk could rise to 99.6%. If everyone onboard wore a surgical mask, the average risk of infection dropped as low as 3%, the authors added. Importantly, this scenario did not take into account the benefits of vaccination, which likely reduces the transmission risk further—but the findings do suggest that masks can add an extra layer of protection on flights. Another modeling study, published in December 2021, tried to find the best airplane seating arrangement to reduce viral transmission, again by using simulations of airborne spread. If someone on a flight has COVID-19, you obviously don’t want to sit next to them, but you also don’t want to sit behind them, the researchers concluded. “You have to look at not only east-west transmission, but also north-south transmission,” says co-author Sheldon Jacobson, a computer scientist at the University of Illinois at Urbana-Champaign who studies public health and aviation security and has received funding from the U.S. Air Force Office of Scientific Research. Keeping middle seats open and leaving some rows empty was the safest seating arrangement, his team concluded. (Airlines, however, are no longer selling flights at reduced capacities.) Regardless of seating arrangement, masking reduced the chances of transmission onboard by about 30%, according to his team’s model. Of course, theoretical calculations don’t always hold up in practice. In the September 2021 research review that looked at real-world studies of viral spread on planes, the authors concluded, “It is not clear whether the use of masks can prevent transmission of SARS-CoV-2 in flights.” That doesn’t mean masks do or do not work—only that published studies haven’t fully answered the question. It’s also worth noting that all of the studies in that review were published before the emergence of the highly contagious Omicron variant. Still, some real-world data suggest that masks work on planes. “If you look at the studies, most of the in-flight transmission…occurred in flights earlier than March 2020, prior to the enforcement of in-flight mask-wearing policy,” Khatib says. Does wearing a mask on a plane help if no one else wears one?Khatib says the federal travel mask mandate probably should be extended again, but it remains to be seen whether that will happen. “Given that we’re still coming off a huge Omicron surge” and that there have been reports of a new, related variant, “it does seem a little bit premature to lift these mask mandates,” she says. Even if the mandate expires, Khatib says she will continue masking up on flights. Jacobson says he will do the same. Highly protective masks, such as N95s and KN95s, can filter out almost all particles when worn correctly, so they can help keep the wearer healthy even if those around them are unmasked. Some survey data suggest that many people will keep wearing masks, even if they are not required to do so. In a May 2021 survey conducted by the International Air Transport Association, 83% of people said they favored masking on flights, even though the majority of respondents said they did not want mandates in place forever. Regardless of what happens at the policy level, Khatib emphasizes that no one should travel while symptomatic, and recommends that passengers “wear a protective mask that fits well and you’ll wear consistently.” An N95 or KN95 is the most protective option, but if you find them too uncomfortable to wear for long periods of time, choose a surgical or cloth mask you’ll keep on, she says. from https://ift.tt/cdRbKWx Check out https://takiaisfobia.blogspot.com/ WASHINGTON — Nearly half of the 500 million free COVID-19 tests the Biden administration recently made available to the public still have not been claimed as virus cases plummet and people feel less urgency to test. Wild demand swings have been a subplot in the pandemic, from vaccines to hand sanitizer, along with tests. On the first day of the White House test giveaway in January, COVIDtests.gov received over 45 million orders. Now officials say fewer than 100,000 orders a day are coming in for the packages of four free rapid tests per household, delivered by the U.S. Postal Service. Still, the White House sees the program as a step toward a deeper, yet more elastic, testing infrastructure that will accommodate demand surges and remain on standby when cases wane. “We totally intend to sustain this market,” Dr. Tom Inglesby, testing adviser to the COVID-19 response team, told The Associated Press. “We know the market is volatile and will come up and down with surges in variants.” The White House says Americans have placed 68 million orders for packages of tests, which leaves about 46% of the stock of tests still available to be ordered. Testing will become more important with mask requirements now easing, say some independent experts. “If infection control is still our priority, testing is central,” said Dr. Leana Wen, a former Baltimore health commissioner and commentator on the pandemic. “Four tests per household for one family will only last you one time. There should be enough tests for families to test twice a week.” Inglesby maintains that the pieces are falling into place to accommodate that. Private insurers are now required to cover eight free rapid tests per person, per month. Medicare coverage will start in the spring. The administration has also been making free at-home tests available through libraries, clinics and other community venues. Capacity for the more accurate PCR tests performed by labs has been built up. The White House recently put out a request to industry for ideas on how to sustain and expand domestic testing for the rest of this year. Wen says people still need a guide for when to test and how often. “Right now it is still unclear,” she said. President Joe Biden’s pivot to testing came under duress as the omicron variant gained force just before Christmas. Tests were frustratingly hard to come by, and expensive. The White House is sensitive to criticism that help may have come too late. “There is no question some people found out they were positive from taking one of these tests and were able to keep other people from getting infected,” said Tim Manning, supply coordinator for the COVID-19 response team. Around mid-December, with omicron projections grimmer by the day, White House officials began discussing how to make free tests available for anyone who wanted one. But if the government started siphoning up tests on the market, that would just make the shortage worse. “A critical thing to us was that anything we did had to be done in a way did not create a shortage at retail to the general public,” Manning said. The White House enlisted the Pentagon and parts of the Health and Human Services Department that had worked on the Trump administration’s vaccine development effort to distribute vaccines. Logistics experts scoured the globe for available tests. The Postal Service was designated to take the orders and deliver them. That part proved to be a good call, said Hana Schank, an expert on government technology projects with the New America think-tank. The Postal Service already had a database of every address in the land, and the means to deliver. “At the federal level the only people who have a database connected to a fulfillment engine would be the Post Office,” she said. The project took less than a month to get ready, Manning said. “We said this is not online retail,” he said. “This is emergency response, so we have go to as fast as possible.” To make sure it wasn’t just the tech savvy who would end up getting free tests, the administration targeted a share of deliveries to people in low-income areas. The White House worked with service organizations to get the word out. “We prioritized the processing of orders to the highest social vulnerability zip codes in the country,” testing adviser Inglesby said. One of the service groups was the National Association of Community Health Workers, whose members help people navigate the health care system. Executive director Denise Smith said the group was able to use its website to link more than 630,000 people to COVIDtests.gov. Overall about 20% to 25% of the tests have gone to people in distressed areas, officials said. Now that demand is way down, it’s unclear what will happen to the White House giveaway program. Allowing repeat orders is one possibility. Smith says groups like hers should get any surplus. “We know where the people are,” she said. Although the program is still in its infancy, analyst Lindsey Dawson of the Kaiser Family Foundation believes its legacy may lie in familiarizing more people with testing. “It may get someone comfortable with utilizing the tests, thinking about how they might use testing in their lives,” she said. Savita Sharaf, a retiree from the Maryland suburbs outside the nation’s capital, said she ordered her free tests around the middle of January and got them in early February. She’s tried to conserve them, for added peace of mind. In the stores, she couldn’t find tests for less than $25. “I’m so relieved because I can immediately test myself,” Sharaf said. “If we had a high vaccination rate, it would be a little easier to say let up on this program. But I feel we have to watch for the next month or two, to see what happens.” from https://ift.tt/hZTOuiX Check out https://takiaisfobia.blogspot.com/ As of today, the U.S. Centers for Disease Control and Prevention (CDC) no longer advises mask-wearing in public indoor spaces for most Americans. Using a new method to determine community risk, more than half of U.S. counties—home to about 70% of the nation’s population—do not currently meet the threshold for recommended universal indoor masking, CDC officials said during a press briefing today. (You can search your county’s COVID-19 risk level here.) “With widespread population immunity, the overall risk of severe disease is now, generally, lower,” CDC Director Dr. Rochelle Walensky said during the briefing. The CDC is now focused on preventing severe disease and health care strain, she said, instead of solely stopping new infections. The agency now determines an area’s risk based on its hospitalization rates, health care capacity, and the rate of new cases, instead of just case numbers and test positivity rates. Universal indoor masking is now recommended only for counties that are deemed high risk based on these metrics. Schools can follow the same guidance as the wider community, CDC officials said. (Of course, people may choose to wear masks if they wish, and the CDC advises everyone with COVID-19 symptoms to wear a mask. The CDC also urges Americans to stay up-to-date on their COVID-19 vaccinations regardless of their community’s risk level.) The masking advice does not apply to airplanes, trains, and transit centers, where masking is still required by a national mandate through at least March 18. The change comes just weeks after Walensky said, on Feb. 9, that it was too soon to alter the agency’s mask guidelines given high rates of infection and death, even though some states were ending mandates. Case counts have fallen dramatically since then, dropping from an average of more than 210,000 diagnoses per day to about 75,000 per day as of Feb. 23. Average deaths have also fallen from about 2,500 to roughly 1,500 per day since Feb. 9. The CDC drew widespread criticism in May 2021, when it said vaccinated people in the U.S. no longer needed to wear masks indoors. Many experts called that move premature; indeed, it came shortly before the Delta variant caused cases and hospitalizations to surge over the summer. Omicron caused an even larger spike in cases a few months later. The latest shift in guidance is also sure to be controversial, pitting those who feel it’s time to live with COVID-19 against those who argue it’s too soon to abandon pandemic precautions, given that tens of thousands of people are still infected by the virus every day and vaccines are not yet authorized for the nation’s youngest children. Which side is correct remains to be seen—but during the press briefing, Walensky acknowledged that guidance could change in the future. “We want to give people a break from things like mask-wearing when our levels are low, and then have the ability to reach for them again should things get worse in the future,” she said. from https://ift.tt/ZoDeE3a Check out https://takiaisfobia.blogspot.com/ (Camden, N.J.) — Drugmaker Johnson & Johnson and three major distributors finalized nationwide settlements over their role in the opioid addiction crisis Friday, an announcement that clears the way for $26 billion to flow to nearly every state and local government in the U.S. Taken together, the settlements are the largest to date among the many opioid-related cases that have been playing out across the country. They’re expected to provide a significant boost to efforts aimed at reversing the crisis in places that have been devastated by it, including many parts of rural America. Johnson & Johnson, AmerisourceBergen, Cardinal Health, and McKesson announced the settlement plan last year, but the deal was contingent on getting participation from a critical mass of state and local governments. Friday was the deadline for the companies to announce whether they felt enough governments had committed to participate in the settlement and relinquish the right to sue. The four companies notified lawyers for the governments in the case that their thresholds were met, meaning money could start flowing to communities by April. “We’re never going to have enough money to immediately cure this problem,” said Joe Rice, one of the lead lawyers who represented local governments in the litigation that led to the settlement. “What we’re trying to do is give a lot of small communities a chance to try to change some of their problems.” While none of the settlement money will go directly to victims of opioid addiction or their survivors, the vast majority of it is required to be used to deal with the epidemic. The need for the funding runs deep. Kathleen Noonan, CEO of the Camden Coalition of Healthcare Providers, said a portion of the settlement money should be used to provide housing to people with addictions who are homeless. “We have clients who have a hard time staying clean to make it in a shelter,” she said. “We would like to stabilize them so we can help them recover.” Dan Keashen, a spokesman for Camden County government, said officials are thinking about using settlement money for a public education campaign to warn about the dangers of fentanyl. They also want to send more drug counselors into the streets, put additional social workers in municipal courts and pay for anti-addiction medications in the county jail. Read More: Why Prescription Opioids Aren’t Only a Problem for White Americans Officials across the country are considering pumping the money into similar priorities. California Gov. Gavin Newsom’s proposed budget calls for using $50 million of the state’s expected $86 million share this year for youth opioid education and to train treatment providers, improve data collection and distribute naloxone, a drug that reverses overdoses. In Florida’s Broward County, home to Fort Lauderdale, the number of beds in a county-run detoxification facility could be expanded from 50 to 70 or 75, said Danielle Wang French, a lawyer for the county. “It’s not enough, but it’s a good start,” she said of the settlement. With fatal overdoses continuing to rage across the U.S., largely because of the spread of fentanyl and other illicitly produced synthetic opioids, public health experts are urging governments to use the money to ensure access to drug treatment for people with addictions. They also emphasize the need to fund programs that are proven to work, collect data on their efforts and launch prevention efforts aimed at young people, all while focusing on racial equity. “It shouldn’t be: ready, set spend,” said Joshua Sharfstein, a former secretary of the Maryland Department of Health who is now a vice dean of public health at Johns Hopkins University. “It should be: think, strategize, spend.” In a separate deal that also is included in the $26 billion, the four companies reached a $590 million settlement with the nation’s federally recognized Native American tribes. About $2 billion is being set aside for fees and expenses for the lawyers who have spent years working on the case. New Brunswick, New Jersey-based Johnson & Johnson has nine years to pay its $5 billion share. The distributors — Conshohocken, Pennsylvania-based AmerisourceBergen; Columbus, Ohio-based Cardinal Health; and Irving, Texas-based McKesson — agreed to pay their combined $21 billion over 18 years. To reach the maximum amounts, states have to get local governments to sign on. The settlements go beyond money. J&J, which has stopped selling prescription opioids, agrees not to resume. The distributors agree to send data to a clearinghouse intended to help flag when prescription drugs are diverted to the black market. The companies are not admitting wrongdoing and are continuing to defend themselves against claims that they helped cause the opioid crisis that were brought by entities that are not involved in the settlements. The requirement that most of the money be used to address the opioid crisis contrasts with a series of public health settlements in the 1990s with tobacco companies. In those cases, states used big chunks of the settlement money to fill budget gaps and fund other priorities. Read More: Older Americans Are the Ignored Victims of the Opioid Epidemic The amount sent to each state under the opioid settlement depends on a formula that takes into account the severity of the crisis and the population. County and local governments also get shares of the money. A handful of states — Alabama, New Hampshire, Oklahoma, Washington and West Virginia — have not joined all or part of the settlement, mostly because they have their own deals or are preparing for trial. In Camden, Lisa Davey, a recovery specialist for Maryville Addiction treatment Center, was at a needle exchange this week handing out naloxone, a drug that reverses overdoses, and asking people if they wanted to start treatment. Davey said she wants to see detoxification and treatment programs receive more funding to keep people in them for longer. As it is, she said, users can detox and be back out on the streets in search of drugs within days. “They need more time to work their recovery,” she said. A man picking up clean needles who asked to be identified only as Anthony P. said he was 46 and had struggled with addiction since he was a teenager. He said he’d like to see an effort to cut off fentanyl and related synthetic opioids that are driving overdose death rates from the drug supply. “Fentanyl’s got to go,” he said. Martha Chavis, president and CEO of Camden Area Health Education Center, which runs the needle exchange, said one need is offering services like hers in more places. Now, users from far-flung suburbs travel into Camden to get clean needles and kits to test their drugs for fentanyl. The settlement with J&J and the three distributors marks a major step toward resolving the vast constellation of lawsuits in the U.S. over liability for an epidemic that has been linked to the deaths of more than 500,000 Americans over the past two decades. Other companies, including business consultant McKinsey and drugmakers Endo, Mallinckrodt and Teva, have reached national settlements or a series of local ones. OxyContin maker Purdue Pharma and a group of states are in mediation through U.S. Bankruptcy Court to try to reach a nationwide settlement. The crisis has deepened during the coronavirus pandemic, with U.S. opioid-related deaths reaching a high of more than 76,000 in the 12 months that ended in April 2021, largely because of the spread of fentanyl and other lab-made drugs. A recent report from a commission by the Lancet medical journal projected that 1.2 million Americans could die of opioid overdose between 2020 and 2029 without policy changes. John F. Kelly, a professor of psychiatry in addiction medicine at Harvard Medical School, said he wants to see money from the settlements go not just for treatment, recovery and support efforts but also to build systems designed to prevent this sort of epidemic from happening again. “Some kind of national board or organization could be set up … to prevent this kind of lack of oversight from happening again — where industry is allowed to create a public health hazard,” he said. from https://ift.tt/OZGhmuq Check out https://takiaisfobia.blogspot.com/ COVID-19 Killed My Grandfather. But My Dad Was Too Busy Treating COVID-19 Patients to Grieve Him2/24/2022 In early February, I got the call I’d dreaded for months: my 82-year-old grandfather, Charlie Law, had died. I’d tried to prepare myself as best as I could; Grandpa had Parkinson’s disease and dementia, and he had been in physical and mental decline for about four years. Still, I hadn’t seen my grandparents in person for two of those years because of the pandemic. Once the initial waves of shock and sadness had washed over me, I was surprised to find I was angry. Losing my grandfather was inevitable, but it felt as if the disease that finally took his life—COVID-19—was not. Although my grandfather was vaccinated and boosted, his dementia had confined him to a nursing home, which meant that he was at the mercy of the assisted living facility and the surrounding community to protect him from the virus. While I’d accepted that my grandpa didn’t have long to live, and I knew that he was suffering, I’d hoped (naively, maybe) that he’d slip away in his sleep. COVID-19 had robbed him of even that. Shortly after Grandpa passed, I asked my dad, Dr. Kevin Law—a doctor specializing in pulmonology and critical care at Robert Wood Johnson University Hospital Hamilton in New Jersey—about how he is coping with losing his father to COVID-19. He has helped lead his hospital’s response to the pandemic through surge after surge for the last two years and has treated about 1,200 patients with COVID-19 at the hospital. Grandpa getting COVID and suffering was the thing I was hoping wouldn’t happen. KEVIN LAW: I had an educated guess that he was going to get a life-threatening infection this winter: either a urinary tract infection, pneumonia, or COVID. I wasn’t there, but I really don’t think he suffered. Maybe that’s my mind playing tricks on me, but I’ve seen patients like this. When they’re very infirm, they become unconscious and go quickly. I know my mom had some anger about it and felt like he hadn’t been protected at the nursing home. But I’d like to think that the institution did its due diligence to protect the patient. Unfortunately, this latest iteration of COVID is very infectious. If you’re susceptible, I don’t think there’s any escaping it, whether you’re out in public or in an institution. Has being on the front lines of the pandemic made it harder for you to cope with Grandpa’s decline? KL: I don’t think I was as present for my parents as I would have been ordinarily, and that that was frustrating. I’m very busy, they’re in another part of the country, and at times it’s been risky to travel. I was surprised that you worked on the day that Grandpa passed. lt must have been hard for you. KL: For your own mental health, you have to learn how to separate work, play, and personal life. I compartmentalize. You have to be able to do your job. You learn over time—as hard as it is, sometimes—to not let it interfere with your professional functioning. If I did, it would be very difficult to function. A lot of people said I should have taken the day off, I should have taken a week off. I certainly contemplated that, but it would have just been way too much for the people I work with. They would have been overwhelmed. I have pretty complicated feelings about the circumstances of Grandpa’s death, because like you, I expected he would pass anyway. But it just feels bad that people didn’t try harder to stop the virus from spreading. KL: Over time, I learned not to waste a lot of energy on people’s behavior that I can’t change. I try to work on it with individuals, and I do get frustrated at times, dealing with individuals that don’t have a good explanation for why they’re not getting vaccinated. The fact that some people are going to be resistant to it is just human nature, and there’s nothing I can do to change that. I do see people who, even though they’re not doing well, are still happy with their decision that they weren’t vaccinated, which is a remarkable thing to me. Or they’re willing to accept their fate, such as it is. How have patients been treating you recently at this point in the pandemic? KL: I see a lot of impatience. I see a general lack of understanding. I don’t think they have as much empathy for us when we’re fatigued or working hard or late or running behind. I think people were very sympathetic at first, and I don’t think they are anymore. They have to understand that a lot of us are still in that same position. We’re still working much harder than we normally would. Even though most of us are vaccinated, we’re still putting our livelihoods and our health at risk. We’re really still working for the public and individuals. If they have some anger or frustration over this whole thing, it shouldn’t be targeting medical workers. How do you deal with your own anger at people for not getting vaccinated? How do you take care of yourself? KL: There are times when I have empathy fatigue: when I don’t feel as empathetic as I would normally feel for a sick, infected patient if they’re not vaccinated. I have plenty of empathy for people who did get vaccinated but got sick in spite of it. Anger is a strong word. It’s more frustration and the feeling of impotence over the situation at times. The time I most feel it is when we’re very busy in the hospital. I’ve seen 30 hospitalized COVID patients in a single day, sometimes 35. It wears you down. Maybe my experience helps me to handle the pain of my dad’s death a little better. And it helps minimize my anger and frustration. I think that some of the anger that people have about the virus, and the restrictions that have been placed on them, are somehow transferred onto physicians, nursing staff, and hospital workers. When I feel like somebody is targeting me or displacing their anger, this is something that I can call upon to kind of defuse that situation. I say, “Listen, I lost my dad to this as well. So on some level, I understand what you’re feeling.” from https://ift.tt/Is4NG9y Check out https://takiaisfobia.blogspot.com/ Over two years since the first cases started appearing in Wuhan, China, there is much we don’t know about the origins of SARS-CoV-2, the virus causing COVID-19. But a quick resolution to that question is possible: scientists could find bats in a cave somewhere in China or in southeast Asia and trace a chain leading from those bats to the COVID-19 outbreak in Wuhan. Realistically, however, recent history offers little promise for this to happen quickly. For example, about 14 years elapsed between the identification of HIV as the virus that caused AIDS and a demonstration of its modern transition to humans from a specific group of chimpanzees, although this had been suspected some years earlier. About a decade passed from the time of the 2003-4 epidemic of SARS and definitive delineation of the origin of its causal coronavirus, and seven years passed before the 2009-10 influenza pandemic was shown to have originated in Mexican swine. The alternative possibility to a natural origin—a laboratory leak—will be difficult to definitively prove or disprove. More importantly, focusing on origins begs a question were there really major health policy or research directional changes for previous pandemics when the origins were determined? Take HIV for instance: we learned the chimp to man transmission occurred in rain forests, but we did not interrupt visits or human life in rain forests. We learned HIV likely came to cities because of population movements and increased prostitution, and then became global by changes such as frequent travel by large numbers, increased sexual contacts, blood and plasma medical use, and IV drug addiction. Needless to say, public policy changed little. SARS origin was learned but we now have SARS-CoV-2. The great influenza pandemic may have originated in WW I army barracks, but we moved on to WW II and did not stop soldiers being in barracks. In short, knowing origins made little difference in how we treated and dealt with the disease—in most if not all cases. Yet the World Health Organization (and much of the scientific community) initially agreed with the Trump Administration’s claim that understanding the origin of SARS-CoV-2 was of vital immediate importance. The administration’s concern was, plausibly, less a matter of dispassionate interest in science but more an effort to open a new front in the U.S. response to a rising China, or an effort to divert attention from a delayed and chaotic U.S. response to the pandemic. Those who advocate for an intensive effort to discover the origins of SARS-CoV-2 assert there would be value in terms of establishing public or public health policy based on that understanding. Just what should be done differently to counter Delta or, now, Omicron by understanding the origin of SARS-CoV-2 better? Knowing origins could bring closure to the ongoing politically charged debate and contribute importantly to scientific understanding. We doubt, however, that knowledge of origins would change anything about how we should respond to the challenges of SARS-CoV-2, or how we would prepare for a future pandemic. We can act now on the assumption that either hypothesis (nature or laboratory leak) could be correct. Here is where the origins discussion now stands: One idea is that there was a natural origin; bat to man directly or through an intermediary animal. The other is that the cause was research error. Scientists studying bats in the field could have become infected themselves or have brought infected bats back to the laboratory. Then by accidental release the virus spread. It is also possible that “gain-of-function” research could have created SARS-CoV-2, followed by its accidental release. Early expression of support for the gain-of-function hypothesis concerned CGG, one of the codons specifying the amino acid arginine for its insertion into the virus’s newly forming spike protein thereby enabling a human protease (furin) to more efficiently cut the coronavirus spike protein which can facilitate infection. Nobel Laureate David Baltimore has expressed the view that CGG coding for arginine was so exceptional it would be suggestive of man-made origins, but this proves unconvincing. Other coronaviruses, such as ones causing the common cold, do have the CGG codon for arginine, albeit only a limited number in the so-called beta subgroup to which SARS-CoV-2 belongs. President Biden gave agencies of the U.S. intelligence community (IC) 90 days to assess the likelihood of natural causes versus research error, and they reported their findings in late August. While one agency concluded that research error was more likely, four other agencies concluded that likelihood lay with natural causes, and the summary conclusion of the National Intelligence Council (NIC) likewise favored the natural origins hypothesis although both the individual agencies and the NIC placed only low to moderate confidence in their conclusions. The declassified version of the IC report also pointed to the Chinese government’s “…frustration [that] the international community is using the issue to exert political pressure on China…” as a reason why further Chinese cooperation in establishing origins remains unlikely. While research error remains a possibility, we doubt that a definitive answer will be soon coming. That said, evidence increasingly accumulates in favor of the natural origins hypothesis, and earlier assessments that pointed toward a laboratory leak, like the furin hypothesis discussed above, have weakened with scrutiny. We return to the question of how much it really matters. We know how to respond to each scenario for origin. There is a very limited number of directions to take, and prudence dictates that each should be taken.
There is much scientific interest in understanding the origins of SARS-CoV-2. And, let’s be honest, it would be nice to know. At the same time knowing origins may add little to what we already know in terms of addressing Delta, Omicron and whatever might come next. The best way forward may be to minimize the distraction of a politicized attempt to assess origins while, instead, investing in long-term international collaborative endeavors on SARS-CoV-2 and in preparation for future epidemics and pandemics. from https://ift.tt/ZMXVe6C Check out https://takiaisfobia.blogspot.com/ COVID-19 vaccines are unlikely to trigger a rare inflammatory condition linked to coronavirus infection in children, according to an analysis of U.S. government data published Tuesday. The condition, formally known as multisystem inflammatory syndrome in children, involves fever plus symptoms affecting at least two organs and often includes stomach pain, skin rash or bloodshot eyes. It’s a rare complication in kids who have had COVID-19, and very rarely affects adults. The condition often leads to hospitalization, but most patients recover. First reported in the United Kingdom in early 2020, it is sometimes mistaken for Kawasaki disease, which can cause swelling and heart problems. Since February 2020, more than 6,800 cases have been reported in the U.S., according to the Centers for Disease Control and Prevention. As part of COVID-19 vaccine safety monitoring, the CDC and U.S. Food and Drug Administration added the condition to a list of several potential adverse events of special interest. A few cases reported in people with no detectable evidence of coronavirus infection prompted researchers at the CDC and elsewhere to undertake the new analysis, which was published Tuesday in the Lancet Child & Adolescent Health. The possibility that the vaccines could somehow prompt the condition is only theoretical and the analysis found no evidence that it did, said co-author Dr. Buddy Creech, a Vanderbilt University pediatric infectious disease specialist who is leading a study of Moderna shots in children. “We don’t know what the exact contribution of the vaccine to these illnesses is,’’ Creech said. “Vaccine alone in absence of a preceding infection appears not to be a substantial trigger.’’ Read More: Why You Should Vaccinate Your Kids Against COVID-19 The analysis involved surveillance data for the first nine months of COVID-19 vaccination in the U.S., from December 2020 through August 2021. During that time, the FDA authorized Pfizer’s COVID-19 shots for ages 16 and up; expanded that in May to ages 12 through 15; and authorized Moderna and Johnson & Johnson shots for ages 18 and up. More than 21 million people aged 12 to 20 received at least one vaccine dose during that time. Twenty-one of them developed the inflammatory condition afterward. All had received Pfizer shots, the analysis found. Fifteen of the 21 had laboratory evidence of a previous COVID-19 infection that could have triggered the condition. The remaining six had no evidence of a previous infection, but the researchers said they could not conclude definitively that they’d never had COVID-19 or some other infection that could have led to the inflammatory condition. Kids with COVID-19 often have no symptoms and many never get tested. The results suggest that the inflammatory condition may occur after vaccination in 1 in 1 million children who have had COVID-19, and in 1 in 3 million who have no detectable evidence of previous COVID-19 infection. Most kids who had COVID-19 don’t develop the post-infection illness, but it is estimated to happen at a significantly higher rate than both of those post-vaccination figures. In April to June 2020, the rate was 200 cases per million in unvaccinated infected people aged 12-20 in the U.S. “Their findings overall are quite reassuring,’’ Dr. Mary Beth Son of Boston Children’s Hospital wrote in a commentary accompanying the study. Dr. Adam Ratner, a pediatrician-scientist at New York University Langone Health, said the results show that chances are “super rare” for the shots to prompt an immune response that could lead to the inflammatory condition. By contrast, there’s strong evidence that vaccination protects kids from getting COVID-19 as well as the condition, Ratner said. from https://ift.tt/rgeRoh1 Check out https://takiaisfobia.blogspot.com/ Pregnancy-related deaths for U.S. mothers climbed higher in the pandemic’s first year, continuing a decades-long trend that disproportionately affects Black people, according to a government report released Wednesday. Overall in 2020, there were almost 24 deaths per 100,000 births, or 861 deaths total—numbers that reflect mothers dying during pregnancy, childbirth or the year after. The rate was 20 per 100,000 in 2019. Among Black people, there were 55 maternal deaths per 100,000 births—almost triple the rate for whites. The report from the National Center for Health Statistics does not include reasons for the trend and researchers said they have not fully examined how COVID-19, which increases risks for severe illness in pregnancy, might have contributed. The coronavirus could have had an indirect effect. Many people put off medical care early in the pandemic for fear of catching the virus, and virus surges strained the health care system, which could have an impact on pregnancy-related deaths, said Eugene Declercq, a professor and maternal death researcher at Boston University School of Public Health. Read More: The U.S. Death Rate Rose Significantly During the COVID-19 Pandemic He called the high rates “terrible news’’ and noted that the U.S. has continually fared worse in maternal mortality than many other developed countries. Pregnancy-related deaths per 100,000 births climbed from 44 in 2019 to 55 in 2020 among Black people and from 13 to 18 among Hispanics. The 2020 rate among whites, 19 per 100,000 births, was essentially unchanged. Reasons for those disparities are not included in the data. But experts have blamed many factors including differences in rates of underlying health conditions, poor access to quality health care and structural racism. “This is incredibly sad news and especially scary for Black women,’’ said Dr. Laura Riley, OB-GYN chief at Weill Cornell Medicine in New York. Dr. Janelle Bolden, an assistant OB-GYN professor at Northwestern University’s Feinberg School of Medicine, said the report is not surprising. “The pandemic has uncovered the disparities in access to care, healthcare quality and delivery. It has also laid bare the lack of support for public health and social agencies that many people rely on for basic needs,” Bolden said. “These disparities and inadequacies lead to poor care and worse outcomes.” The U.S. maternal mortality rate has more than tripled in 35 years. A decade ago, it was 16 deaths per 100,000 births. It has climbed along with rising rates of obesity, heart disease and cesarean sections, which all increase risks for people giving birth. from https://ift.tt/V0UaFRk Check out https://takiaisfobia.blogspot.com/ In the 40 years that Jennie Kahn has worked as a registered nurse, the last two have been by far the most grueling. A lot of that is due to COVID-19, which transformed health care facilities, including Thomas Health’s hospital system in Charleston, West Virginia, where Kahn works, into triage centers and forced nurses to take on an extraordinary amount of personal risk and heartache. It’s no mystery why some 18% of health care workers quit their jobs between Feb 2020 and Sept 2021, according to a Morning Consult poll. But another reason these past two years have been so punishing, Kahn says, is that hospital nursing staffs have been subject to extraordinary churn as thousands of nurses have quit their staff positions to become contract travel nurses, where the pay is often two to four times higher. This rapid turnover has triggered a costly feedback loop: hospital administrators, facing shortages in staff nurses, spend a mint hiring contract nurses, which makes them less able or willing to increase their staff nurses’ pay. So more staff nurses quit to become contract nurses, thus further lowering nurse supply and driving demand for contract nurses. “It is a vicious cycle,” says Kahn, the hospital system’s chief nursing officer. Meanwhile, contract nursing agencies have increased their prices. The advertised pay rate for travel nurses has surged 67% from January 2020 to January 2022, according to Prolucent Health, a workforce management tool for healthcare companies, while some staffing agencies such as AMN Healthcare, told TIME that pay rates for travel nurses at facilities they work with rose by 164% from the fourth quarter of 2019 to the fourth quarter of 2021. Some of these agencies’ profit margins top 20%. Some hospital administrators, many of which saw their facilities’ profits shrivel during COVID, say they’ve reached a crisis point and are calling on Congress and the Biden Administration to step in. They argue that contract nursing agencies are exploiting circumstances resulting from COVID-19 to pad their own pockets. The agencies say their prices are merely a reflection of growing demand. Nurses, meanwhile, argue that hospital administrators, who are somehow finding a way to pay premium rates for contract nurses, could have avoided the mass nurse exodus by paying their staff nurses better and improving working conditions from the start, and that a fragmented nursing force with quick turnover is bad for patients’ health. The solution is not straight-forward. Health care facilities, desperate to keep nurses on staff, may have to improve salaries and working conditions, but at many facilities, that’s easier said than done. At long-term care centers, bottom lines are dictated by Medicare and Medicaid reimbursement, and at many small and medium-sized hospitals, the cost of personal protective equipment and patient loads have fluctuated dramatically since March 2020. “This is not anything that any health system can sustain for a long period of time,” says Kahn. “If the rates do not decrease or if travel nursing is not reduced somewhat, hospital systems are going to have to find alternative ways to provide patient care.” An explosion of temporary staffingTravel nurses have been around for decades and became more widespread in the 1980s, as nursing shortages grew, but it’s really the pandemic that changed the landscape of the profession. In some healthcare settings, contract nurses are now almost as prevalent as staff nurses. Jeffrey Tieman, president and CEO of Vermont Association of Hospitals and Health Systems (VAHHS), says that prior to COVID-19, his system used travel nurses “as a stop gap”; now he says they’re “in every department of the hospital every day of the week.” The same is true of Thomas Health, Kahn says. When she first became the hospital system’s chief nursing officer in 2019, the acute care team didn’t rely on traveling nurses at all; these days, about 40% of her acute care nurses are on temporary contracts. The financial fallout of this trend for hospitals’ and nursing homes is staggering. Due largely to the increase in contract nurses, Thomas Health is now roughly 100% over its previous staffing budget, the hospital system tells TIME. Between Fiscal Years 2020 and 2021, VAHHS’s outlay for contract nurses increased $29 million, or 35%, the group says. “As the pandemic picked up and dragged on, the need for nurses intensified when the supply of nurses diminished,” Tieman says. Depending on contract nurses also creates logistical problems, says Deb Snell, a registered nurse and the president of the Vermont Federation of Nurses & Health Professionals. “It is difficult when you have new people coming in every 12-13 weeks, and orienting them to your floor, making sure they know where equipment is, where meds are, who to call for a problem,” she says. “It’s constant turnover.” Struggling to fill empty roles and way over budget on staffing, VAHHS reached out to Vermont Congressman Peter Welch for help coming up with a solution, and on Jan. 24, Welch and Morgan Griffith of Virginia wrote a letter to the White House, cosigned by nearly 200 other members of Congress. The letter urges the Biden Administration to investigate the extent to which contract nursing agencies are exploiting the pandemic to drive their profits by engaging in anticompetitive activity. “We are writing because of our concerns that certain nurse-staffing agencies are taking advantage of these difficult circumstances to increase their profits at the expense of patients and the hospitals that treat them,” the letter says. Days later, the American Hospital Association and the American Health Care Association/National Center for Assisted Living, the major nursing home trade group, threw their support behind Welch and Griffith, calling on the Administration to help prevent the travel agencies “from exploiting our organizations’ desperate need for health care personnel.” Travel nurses, meanwhile, were incensed. On social media and message boards, they begged supporters to call their members of Congress to defend them and their pay schedules. “Wait, what? They want to cap travel nurse pay but they won’t cap CEO and executive pay? Well… I guess they know who their true masters are, and it sure as hell ain’t the voters,” wrote one Reddit user. 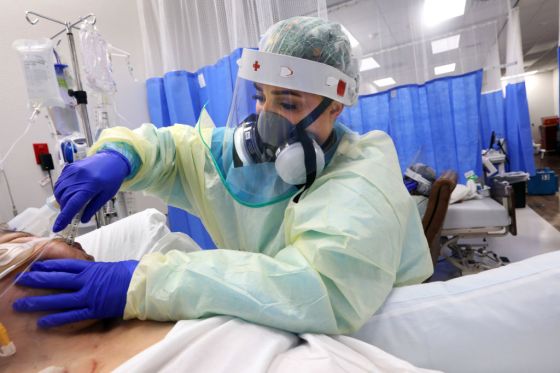
“It’s just because they can get away with it”Welch says capping contract nurses’ take-home pay was never the intention of his letter. “I never have and never would propose a cap on nursing pay,” he says. “Nurses are the frontline, and they’re overworked, they’re underpaid, and they legitimately point out how the executives get fat salaries while they have to do all this work.” Instead, he says, one big reason for the financial burden on hospitals is the fees that nurse staffing agencies charge to assign travel nurses to health care settings that need them. Proculent Health, the workforce management tool used by healthcare companies, estimates that hospitals and other healthcare facilities are billed an additional 28% to 32% above the wages the agencies pay contract nurses. Welch argues these agencies may be exploiting the pandemic’s circumstances at the expense of hospitals, health centers, and the patients who seek care at them. “The fee that the agency charges is not related to any additional work they do, or any value added,” Welch tells TIME. “It’s just because they can get away with it.” AMN Healthcare Services reported its gross profits were $434 million in the fourth quarter of 2021, up 109% from a year prior, according to an annual earnings report. Its net income, which takes into account all business related expenses and taxes it had to pay, was $116 million, an 1100% increase. Another healthcare staffing agency, Cross Country Healthcare, saw its revenue increase 93% between the third quarters of 2020 and 2021. It also reached $1 billion in annual revenue for the first time in the company’s history in 2021. In recent months, private equity firms have begun acquiring contract healthcare staff agencies at a rapid clip, signaling to Welch that investors believe there is even more money to be made off the travel nurse industry in years to come—which would put hospitals under even greater strain. One of the largest healthcare staffing agencies, Medical Solutions, was purchased by two private investment firms in August. Favorite Healthcare, another large staffing group, was bought by a private equity-owned staffing firm in January. “Three of the 10 largest staffing agencies—and probably more—were purchased by private equity right around the time that the pandemic began,” Welch says. Staffing agencies argue that the higher prices health care facilities are paying are driven primarily by the higher wages the agencies pay nurses to meet the demand. In 2020, 75% of revenue nurse staffing agencies made went to wages and the costs of employing nurses, including payroll taxes, worker’s compensation and unemployment insurance payments, and other benefits, says Toby Malara, vice president of government relations for the American Staffing Association (ASA), a trade group for the staffing industry. He adds that most of the association’s nurse staffing agencies have seen their profits remain “relatively stable” during the pandemic. Nurses worry about pay cuts — for good reasonMany nurses are worried that heightened government scrutiny will result in lower take-home pay for them — and that anxiety is not necessarily unfounded. Some states already cap nurse pay under certain situations, or are considering legislative action to do so. Minnesota, for example, caps contract nurses who work in nursing homes. The most that an RN can earn per hour during non-holidays is $62.36, according to documentation provided by the state’s Department of Health. Massachusetts caps pay for RNs at hospitals around $120 per hour. At nursing home facilities, the state caps an RN’s pay around $79 per hour, the state’s Executive Office of Health and Human Services says. Other states including Kansas, Ohio, Oregon, Illinois and Pennsylvania are now considering legislation to cap nurse pay in some cases. Pennsylvania state Rep. Timothy Bonner has introduced a bill to establish maximum rates for employees of travel nursing agencies in his state that would be no higher than 150% of the average statewide pay rate for similar jobs. “[Staffing] agencies have seized on the pandemic and the critical need for workers,” he wrote in a letter to his statehouse colleagues, according to the Lewistown Sentinel, “and have raised their hourly rates to 100 percent, 200 percent or even 400 percent above the current median wage rate.” The White House referred TIME’s questions about how regulatory action against the contract nursing industry would work to the Federal Trade Commission, which did not return a request for comment. Many nurses say arbitrary pay caps are unfair. The problem is not high pay, they say; it is that there aren’t enough nurses to do an increasingly challenging job for relatively low wages. And while the pandemic exacerbated nurse shortages nationwide, the problem long preceded COVID-19’s added pressures. “Things were already getting tight even prior to the pandemic,” says Snell in Vermont. “Nurses have known and seen this coming for a while. We just couldn’t get people to listen.” Part of the issue is demographics. The median age of RNs in 2020 was 52, according to a recent survey from the National Council of State Boards of Nursing, and with baby boomers retiring, more nurses will need replacing. But there’s no lack of interest. Enrollment in baccalaureate and higher-degree nursing programs increased in 2020, according to the American Association of Colleges of Nursing, and nurse practitioner graduates have swelled in recent years too. Nursing schools could be training even more graduates, experts say, but the cost of nursing school can be a barrier for students, and schools are also experiencing a shortage of nursing instructors. But the largest factor, according to nurses unions and professional groups, is how low the pay is compared to how difficult the work environment is. “There is no nursing shortage in the United States. There is a shortage of nurses who are willing to work in these conditions,” says Michelle Mahon, a registered nurse who is assistant director of nursing practice at National Nurses United (NNU), the largest nurses union in the country. “This is something that’s been created by health care employers over a very long period of time.” NNU has frequently criticized hospitals for adopting what it says are policies of chronic understaffing in order to help their bottom line. High patient-to-nurse ratios deteriorated patient care and put nurses at increased risk of workplace injuries and infections before COVID-19, Mahon says. Then when the pandemic swept in, hospitals that had prioritized cutting costs were unprepared. Health care doesn’t operate like a free marketWhile some nurse unions have been able to demand raises from large hospital systems during the pandemic, health facilities that see primarily patients who have government health insurance are often more limited in what they can pay. Nursing homes are overwhelmingly paid by Medicaid and Medicare, so they say the rates they can pay nursing staff are largely determined by how much the government programs reimburse per patient, and hospitals in low-income areas can face similar situations. About 70% of the costs of operating a nursing home are related to labor, according to Clif Porter, senior vice president of government relations at AHCA/NCAL. But even as facilities have had to pay two to three times normal wages to hire temporary nurses during the pandemic, their reimbursement rates have not kept pace. “I can’t pass on inflation to my customer,” he says. “This creates a situation where our expenses exceed our revenue. It’s just that simple. And that’s just not sustainable.” Porter says that he doesn’t want maximums for what nurses can make, but floats the idea of a cap on agency profits or regulations that stipulate how much of what a staffing agency charges it must pass on to its workers. “If the legislation were to directly impact the [agency] overhead, we don’t believe that nurses salaries would be impacted,” says Ernest Grant, president of the American Nurses Association. But the ANA does not support any effort to lower nurse wages, and Grant added that the concern over price gouging has “become quite a distraction.” Mahon agrees, saying the idea of investigating these staffing agencies will not solve the staffing crisis. Even if the health care facilities are not happy about the rates these staffing agencies are charging, she notes, they have found the money to pay them. “If there was serious reflection and introspection and desire to solve [the nursing shortage], it would be focused inward by this industry,” Mahon says. More nurses, better treatmentNurses groups’ say there are other solutions that could retain and attract a larger workforce. NNU would like to see minimum staffing ratios, enhanced workplace safety measures, and increased funding for nursing education, for example. The ANA has also promoted ideas including improving nurse hours and mental health support, adjusting the Centers for Medicare and Medicaid Services payment methods, and removing barriers that make it difficult for nurses to practice. “We really need to address it once and for all, and not just cap it off at this particular time,” Grant says. Desperate to retain staff, Thomas Health, where Jennie Kahn works, has increased bonus pay, instituted recruitment bonuses, expanded its tuition repayment programs and started offering its staff free meals at hospital cafeterias. The University of Vermont Medical Center, meanwhile, just agreed to raise its nurse’s wages by 20% over two years, with 10% being implemented now and an additional 5% coming in October 2022 and an additional 5% coming in October 2023. Though Snell says the raises are a positive step toward retaining staff, she’s not certain it is sufficient to stop the bleeding. A study released in October by the American Nurses Foundation reports 21% of nurses nationwide said they planned to resign from their jobs within the next six months. Another 29% said they were considering leaving. University of Vermont Medical Center is not immune. “We have a lot of nurses leaving our hospital to go travel,” she says. “I’m hoping the 10% right now will be enough to maybe keep some of them in place.” from https://ift.tt/UPkeoRm Check out https://takiaisfobia.blogspot.com/ |
Authorhttps://takiaisfobia.blogspot.com/ Archives
April 2023
Categories |
 RSS Feed
RSS Feed
