|
(BEIJING) — China says it will resume issuing passports for tourism in another big step away from anti-virus controls that isolated the country for almost three years, setting up a potential flood of Chinese going abroad for next month’s Lunar New Year holiday. The announcement Tuesday adds to abrupt changes that are rolling back some of the world’s strictest anti-virus controls as President Xi Jinping’s government tries to reverse an economic slump. Rules that confined millions of people to their homes kept China’s infection rate low but fueled public frustration and crushed economic growth. The latest decision could send free-spending Chinese tourists to revenue-starved destinations in Asia and Europe for Lunar New Year, which begins Jan. 22 and usually is the country’s busiest travel season. But it also presents a danger they might spread COVID-19 as infections surge in China. Travel services companies Trip.com and Qunar said international ticket bookings and searches for visa information on their websites rose five to eight times after Tuesday’s announcement. Top destinations included Japan, Thailand, South Korea, the United States, Britain and Australia. Japan, India, Italy, South Korea and Taiwan have responded to the Chinese wave of infections by requiring virus tests for visitors from China. China stopped issuing visas to foreigners and passports to its own people at the start of the COVID-19 pandemic in early 2020. Read more: China’s Stunning U-Turn on Zero-COVID Takes Xi Jinping From Suffocating Control to Callous Inaction The National Immigration Administration of China said it will start taking applications Jan. 8 for passports for tourists to go abroad. The agency said it will take applications to extend, renew or reissue visas but gave no indication when they might be issued to first-time applicants. China will “gradually resume” admitting foreign visitors, the agency said. It gave no indication when tourist travel from abroad might resume. The changes will “create better conditions for orderly cross-border travel” and “bring more benefits to global economic development,” said a foreign ministry spokesman, Wang Wenbin. China will “work with all countries” to “restore safety and stability to global industrial and supply chains and promote world economic recovery,” Wang said. Health experts and economists expect the ruling Communist Party to keep limits on travel into China until at least mid-2023 while it carries out a campaign to vaccinate millions of elderly people. Experts say that is necessary to prevent a public health crisis. During the pandemic, Chinese with family emergencies or work travel deemed important could obtain passports, but some students and businesspeople with visas to go to foreign countries were blocked by border guards from leaving. The handful of foreign businesspeople and others who were allowed into China were quarantined for up to one week. Before the pandemic, China was the biggest source of foreign tourists for most of its Asian neighbors and an important market for Europe and the United States. The government has dropped or eased most quarantine, testing and other restrictions within China, joining the United States, Japan and other governments in trying to live with the virus instead of stamping out transmission. Read more: One Million Could Die From COVID in China, New Projection Shows. Here’s What to Know Japan and India have begun requiring virus tests for travelers from China. South Korea tests all visitors with elevated temperatures. South Korea says anyone who tests positive will be quarantined at home or in a hotel for a week. South Korean officials said possible additional measures for arrivals from China will be announced Friday. U.S. officials, speaking on condition of anonymity to relate internal discussions, said Washington is considering taking similar steps. Taiwan on Wednesday announced visitors from China will be tested starting Jan. 1. On Monday, the Chinese government said it would scrap quarantine requirements for travelers arriving from abroad, also effective Jan. 8. Foreign companies welcomed the change as an important step to revive slumping business activity. Business groups have warned global companies were shifting investment away from China because foreign executives were blocked from visiting. The American Chamber of Commerce in China says more than 70% of companies that responded to a poll this month expect the impact of the latest wave of outbreaks to last no more than three months, ending in early 2023. The government has stopped reporting nationwide case numbers but announcements by some cities indicate at least tens and possibly hundreds of millions of people might have been infected since the surge began in early October. Experts have forecast 1 million to 2 million deaths in China through the end of 2023. Also Monday, the government downgraded the official seriousness of COVID-19 and removed it from a list of illnesses that require quarantine. It said authorities would stop tracking close contacts and designating areas as being at high or low risk of infection. ___ AP Writers Zeke Miller in Washington and Hyung-jin Kim in Seoul contributed. from https://ift.tt/qyvuYDM Check out https://takiaisfobia.blogspot.com/
0 Comments
Over the past year, the headlines have been dominated by alarming events: the Russian invasion of Ukraine, high inflation, supply chain shortages, and the threat of food insecurity for many nations. But 2022 was also a year of milestones toward a better future, scientific breakthroughs, and stories of hope. Here’s a look at 10 stories of human progress from the last 12 months. 1. We found out that civilization reached peak agricultural landFor nearly all of human history, producing more food required more land. But starting in the early 1900s, and continuing through the next 100 years, four powerful forces—synthetic nitrogen fertilizer, synthetic pesticides, hydrocarbon-powered mechanization, and improved genetic selection—allowed humanity to produce more food from less land. Between 1900 and 2000, agricultural land—that is, the sum of cropland and pastoral land used for grazing livestock— increased dramatically and consistently year after year. But the latest data released in 2022 suggest that while land use for crops is still increasing, total agricultural land use appears to have peaked in the year 2000, and is now in decline. Peak agricultural land use has been driven in large part by changing the way we feed the animals we eat, shifting from grazing livestock to feeding them crops we’ve grown. The change has helped reduce the amount of land that must be converted from wilderness to pasture, which has, in turn, reduced the pressure on wildlife habitat. Progress forward is, however, not progress completed, and to continue to reduce pasture land allocation and turn the tide toward peak cropland, we must continue to improve crop yields. 2. We deployed a malaria vaccine for the first timeBetween the years 2000 and 2020, global malaria deaths declined by roughly 30%; however, in 2021, there were still an estimated 247 million cases and 619,000 related deaths. The hard-won progress thus far has been driven in large part by the expanding use of insecticide-treated bed nets and antimalarial drugs. The most powerful tool in the war against malaria, a safe and effective malaria vaccine, has remained out of reach. But this year, for the first time, the World Health Organization recommended the use of a malaria vaccine: the RTS,S/AS01 Mosquirix shot, which the WHO said should be deployed to protect children living in regions with moderate to high transmission. By April 2022, more than 1 million children in Africa had received the world’s first malaria vaccine. The WHO estimates that the shot could save the lives of roughly 40,000 to 80,000 such children annually. 
In addition, another malaria vaccine, the R21/Matrix-M developed by Adrian Hill and the University of Oxford, also continued to show promise. According to a study published in The Lancet in early December, the vaccine provided 80% protection against the disease in human trials. If approved, the plan is for the R21 malaria vaccine to go into production with the Serum Institute of India, with a target of 200 million doses annually, and may be sold at less than half the price of the RTS,S malaria vaccine. 3. The James Webb telescope brought the universe into focusThrough the end of 2021 and the beginning of 2022, the James Webb Space Telescope had a successful launch, essentially flawless deployment and calibration, and began returning its first images. The next-generation telescope took nearly 26 years and $10 billion to make happen. But it appears the gamble is going to pay off, as Webb brings into focus the way galaxies looked just a few hundred million years after the formation of the universe. The first images from Webb, released in July of 2022, captured the imagination of the world, instilling a sense of both wonder at the magnitude and beauty of space, and also our small and seemingly insignificant place within the greater universe. 
The focus in 2023 will turn to the telescope’s primary missions: studying the early galaxies of the universe, observing star formation, and observing the chemical properties of planetary systems, inclusive of the solar system in which we reside. This year there were hundreds of ways that Webb could have gone wrong, and only one way for the mission to go right. Against all odds, Webb performed flawlessly. Read more: TIME’s Innovator of the Year for 2022: Gregory Robinson and the James Webb Telescope Team 4. Wild mammals rebounded in EuropeAcross Europe, many wild animals are making a comeback, returning to the region’s oceans, forests, and rivers. A reduction in habitat loss and conservation, along with reintroduction programs, offer hope for a future where many native species to the region can once again flourish. For much of the 20th century, hunting and habitat loss reduced large animal populations throughout the European continent. But over the last 50 years, many species have made an incredible comeback, with stable and self-perpetuating populations of large animals, from whales to bison, rebounding. At least 19 species had an average relative change in abundance greater than 100%, while at the top end of improvements, European bison and Eurasian beaver populations grew by an astonishing 16,626% and 16,705%, respectively. 
5. Farmers in the Philippines harvested the first large-scale genetically engineered “golden” rice cropOne of the best stories of progress this year unfolded quietly in 17 rice fields in the Philippines this October. For the first time in world history, farmers in the Philippines harvested golden rice on a large scale--some 74 tons that had been cultivated over the previous year. That’s relatively insignificant when compared to the annual production of conventional rice for the country, a little over 13 million tons in 2022; it is, however, a milestone for genetically engineered rice. While golden rice has been around for decades, this is the first time it has been made legally available. Golden rice is a powerful tool in the fight against vitamin A deficiency, a condition that claims the eyesight and lives of hundreds of thousands of children annually. In 2009 the WHO estimated that “250,000–500,000 children who are vitamin A-deficient become blind every year, and half of them die within 12 months of losing their sight.” Often, this condition affects children in low- and middle-income regions with a high dependency on standard rice, which lacks vitamin A. Golden rice is a version of the staple grain genetically engineered to produce vitamin A, and in theory, could reduce or eliminate vitamin A deficiencies without requiring a major change in dietary habits. 6. Guinea worm disease reached near-eradication levelsIn 1989, there were 892,055 cases of Guinea worm disease, a dreadful and debilitating waterborne parasitic infection historically endemic to Asia, the Middle East, and Africa. In 2022 there were just 15 cases globally—a decline of 99.998%. This astonishing decline in infection rates was driven not by a new vaccine or breakthrough technology, but through community education programs, effective isolation of infected persons from water sources, expanding access to improved and treated water sources, and basic water filtration. Thanks to these largely low-tech mitigations there is now hope that it may be possible, perhaps within the next few years, to declare the disease truly eradicated, 7. India developed its first cervical cancer vaccineThe Serum Institute of India, the world’s largest vaccine manufacturer, announced the development of India’s first domestically developed and manufactured cervical cancer vaccine—but it’s the price that is the true breakthrough. The newly-developed vaccine will provide broad protection against the human papilloma virus (HPV), types 16 and 18, which are responsible for at least 70% of cervical cancers, as well as types 6 and 11. While there are already two highly effective HPV vaccines available in India—Gardasil, from Merck, and Cervarix, from GlaxoSmithKline—they are both prohibitively expensive for many low-income families in India, with each dose costing Rs 2,800 (about $34) and Rs 3,299 (about $40), respectively. The price point for the new domestically-manufactured HPV vaccine is expected to be between 200 rupees and 400 rupees ($2.42-$4.85), ultimately helping more girls across India access the potentially life-saving shot. The Serum Institute is targeting to produce approximately 200 million doses over the coming two years. 8. Lab-grown meat got the green light from the U.S. FDALab-grown meat has been on the horizon for over a decade, with the world’s first lab-grown burger eaten in 2013. In 2022, the technology had a milestone breakthrough, when California-based Upside Foods’ meat cultivated directly from chicken cells was given a green light from the U.S. Food and Drug Administration. The FDA basically says Upside’s cultivated chicken is safe for human consumption; the next step is to get approval from the U.S. Department of Agriculture. After that, it would be the first lab-grown meat to be sold in the U.S. 
The technology, while still in its infancy, could help transform how we grow and consume meat, providing a sustainable alternative to the modern factory farm. If developers can effectively scale and market lab-grown meat effectively, it could help to offset the high inefficiency losses in using living animals to turn energy into delicious protein, reducing resource consumption and credulity. Read More: Exclusive: We Tasted The World’s First Cultivated Steak, No Cows Required 9. The SARS-COV-2 vaccine saved millions of livesIn light of the hardships experienced by billions of people globally, you would be forgiven for overlooking the silver lining that was the rapid research, development, manufacturing, and deployment of the four primary COVID-19 vaccines. A study published in June in The Lancet concluded that SARS-COV2 vaccination had already prevented between 14-20 million COVID-19 related deaths across 185 countries globally. 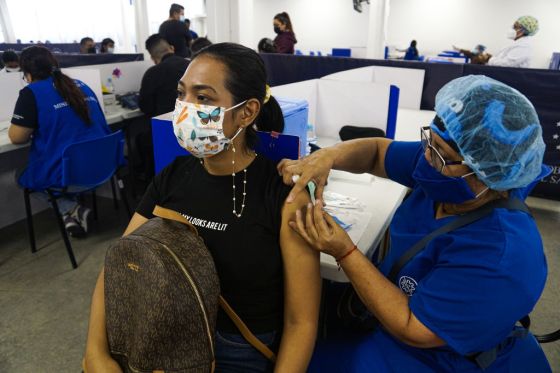
The Commonwealth Fund, a private foundation, estimates that the administration of the roughly 655 million doses covering 80% of the U.S. population has prevented more than 18 million hospitalizations and 3 million deaths. The vaccine deployment saved an estimated $1 trillion in medical costs, to say nothing of the social and emotional devastation it helped avoid. 10. CRISPR for cancer had a major breakthroughThis year has been replete with news of advancement in medical and agricultural applications for the genetic engineering tool CRISPR. Among the most powerful stories about CRISPR was its breakthrough effect in the treatment of a 13-year-old girl suffering from aggressive leukemia that was unresponsive to conventional treatment. The teenager had her immune cells genetically altered via CRISPR to seek out and destroy cancer; she now has no detectable cancer within her body. While it may be too early to hail the new treatment as a readily deployable cure, it’s unquestionably a major breakthrough, possibly a watershed moment in the history of how humanity treats cancer. Doctors and researchers are now working toward engaging another 10 adolescent patients for further trials of the treatment. The breakthrough was part of the larger story of progress in the use of CRISPR for the treatment of cancer, with research advancing on a number of fronts, including most prominently a promising personalized T cell modification which would allow for the body’s own immune system to fight solid cancers, and with the FDA lifting its ban on CRISPR base editing for cancer treatment. from https://ift.tt/bhIc7Fm Check out https://takiaisfobia.blogspot.com/ People who have inflammatory bowel disease (IBD)—which is the umbrella term for Crohn’s disease and ulcerative colitis—often experience a range of symptoms, from intense abdominal cramping and pain to persistent diarrhea and overwhelming fatigue. Living with IBD can significantly disrupt everyday life and make it challenging to maintain physical and mental wellbeing. There’s no cure for IBD—it lasts a lifetime. Like other chronic conditions, IBD can go into remission with effective treatment, but people might still experience occasional flares that make life more difficult. Approximately 1.6 million people in the U.S. have Crohn’s or ulcerative colitis, and about 70,000 new cases of IBD are diagnosed in the U.S. each year. Here’s what seven patients with the disease wish doctors knew when it comes to helping them manage the condition more effectively. We want you to be upfront about gaps in knowledgeResearchers have learned a lot about IBD, including risk factors such as smoking, family history of the condition, and antibiotic use—but there’s still much to learn about why someone develops IBD. One of the biggest questions patients tend to have is: What caused this? And more often than not, doctors simply don’t have the answer. Being clear about that would be helpful, says Georgia resident Lisamarie Monaco, 49, who was diagnosed with IBD in 2002. “I wish our doctors knew the actual cause of IBD,” she says. “But until then, it would be nice to have more transparency and directness about what isn’t known.” Talking about new research gives us hopePart of the discussion around how much is left to discover could focus on what’s being done to find new treatments, adds Brooke Abbott, 39, a Los Angeles resident who had surgery in 2012 to have her colon removed for IBD management. “Hearing about clinical trials and research advances is super important because even if that doesn’t affect the patient directly, it gives us hope that work is being done,” she says. “We take comfort in knowing there might be something coming down the road that might make a difference.” Such conversations could also lead to patient involvement in clinical trials, she says. Clinical trials aren’t always centered on medications, Abbott notes; some examine things like the value of mental-health support or stress relief. “Many of us are eager to be part of what’s moving IBD management forward, not just controlling our symptoms on an individual basis,” Abbott says. “People with IBD are very connected to each other for support, so we’re interested in improving not just our lives, but those of others with this condition, too.” Even if patients aren’t a match for clinical trials, making them feel included in the process would be empowering, adds Connecticut resident and IBD patient Kelly Owens, 34, whose work as a clinical researcher has helped her understand how it feels to contribute to scientific progress. “We need to change the narrative and refocus our collective efforts on advancing the research and translation of novel therapeutics into clinical practice,” she says. “It’s not enough to focus only on disease awareness initiatives. We’re all aware. Now we need action.” Read More: How to Maintain Your Social Life When You Have IBD Be aware of potential racial biasAbbott’s journey from IBD diagnosis to management has been difficult, she says: It took almost 12 years for her to find a care team that wasn’t dismissive of her symptoms. In the past, doctors have implied that she was a drug seeker because she was having intense pain, or that she was “wiping too hard” when a bowel movement would fill the toilet with blood. “As a Black woman, I do think the gaslighting was pretty dominant in my care for a long time,” she says. “It’s extremely frustrating to be debilitated by this disease and then told it’s no big deal, or that I couldn’t possibly have IBD unless one of my parents was Jewish.” While IBD risk is higher among the Ashkenazi Jewish population, such a statement implies that most Black people don’t develop the condition. In actuality, researchers at Johns Hopkins Medicine have concluded that Black people are at significant risk for IBD since they have a genetic marker related to the disease—it’s the same gene variant that makes them four times more likely to develop lupus than white Americans. According to research in the American Journal of Gastroenterology, Black people also tend to have less access to IBD specialists, experience higher rates of disease complications, and visit the ER more often due to intense IBD symptoms. Abbott hopes that greater awareness of issues like these could lead more doctors to reflect on whether they’re operating from a position of unconscious bias, or if they can do more to address bias within their health-care systems. We crave in-depth discussion about nutritionFor six years after his IBD diagnosis in 2003, Sanjiv Devraj felt like he should have his own permanent room at the hospital. The 52-year-old Atlanta resident experienced frequent pain, weakness, and bleeding as a result of his severe ulcerative colitis. He asked his doctors what he should be eating, but received scant information. “I often felt defeated,” he recalls. “Given that this is a disease affecting the digestive system, I wanted my doctors to talk more about nutrition, but that wasn’t covered in our appointments. I felt forced to do my own research.” Through a process of trial and error with an array of foods, he finally found a nutritional path that not only gave him more energy overall, but also kept him out of the ER. “I do wish I’d had more support through this process, and perhaps some research into how certain foods affect gut health,” he says. “More of a focus on building a healthy gut through foods, and also through other lifestyle habits like exercise and sleep, would be a conversation I think anyone with IBD would love to have.” Even just chatting about why it’s important to find out which foods trigger symptoms is helpful, says Delaware resident Marianne Sarcich, 56, who was put on a specific eating plan called the low-FODMAP diet when she was first diagnosed. That approach involved eliminating many foods and then adding them back into her diet; the strategy made it very clear which foods sent her IBD into a flare, such as gluten, garlic, and onions. It would also be useful for doctors to mention that IBD patients may not need to avoid trigger foods forever, Sarcich adds. Part of the way both Devraj and Sarcich navigated through diet changes has been to re-introduce problematic foods occasionally and see if they’re still on the “avoid” list. For example, Sarcich says she experienced symptoms with a huge array of foods when she was first diagnosed—but over the years, the list has dwindled to just a few culprits. She believes that if doctors kept track of the effects of these lifestyle habits in the same way as managing medication outcomes, it could make for more meaningful care. Stress management should be a larger part of treatmentAlthough stress is not considered a cause of IBD, it can be a major trigger for symptoms, many people with IBD have found. Research backs that up: A 2019 study in Frontiers in Pediatrics found that for both children and adults, psychological stress is associated with relapses, since it can have significant and negative effects on the digestive system. Another study, published in a 2018 edition of the Proceedings of the National Academy of Sciences, suggests chronic stress can also lead to progression of IBD, which means what may have started with mild symptoms could worsen over time if there’s no stress management. Because of that, incorporating stress relief into an overall treatment plan could be a crucial way to keep the disease controlled, says 32-year old Texas resident Samantha Plevney. “When you’re stressed and sick, this can be really hard to manage emotionally,” she says. “I wish my doctors knew how much of a toll this disease takes and how hard it is to maintain a normal life with everyday commitments along with appointments, regular medications or infusions, and the stress of symptoms flaring up. Maybe they do know, but if that’s the case, I wish they talked more about it.” Being under so much stress can feel isolating, Plevney adds, and there have been several appointments during which she tried to articulate that she no longer felt like she was really living—only just existing. For example, when she’s experiencing flares, she’s not able to go out with her friends or eat foods she loves. She also has to manage her condition while caring for her family and juggling a career. “This disease goes way beyond physical symptoms—it can be incredibly stressful, and addressing that should be part of treatment,” she says. Read More: These Environmental Factors Increase the Risk of IBD Mental-health needs should be better addressedStress is just one mental-health concern that can be sparked by IBD. There’s also anxiety over flares, potential embarrassment about symptoms, discouragement with treatment options that aren’t working well, and the frustration that comes with managing a chronic illness. A 2021 study in the journal Frontiers in “I wish doctors were more aware of how to help with the mental side of IBD, especially when it causes embarrassing feelings,” says Ohio resident Cassie Mahon, 39. “I also wish doctors would make it easier for shy people to speak with them about symptoms that are hard to talk about.” For example, she adds that one-on-one conversations may be challenging for some patients, but that’s not the only way to support mental health. Doctors could be proactive by putting together a printed list of mental-health resources and offering virtual visits for patients with IBD—even just leaving home can be overwhelming and full of anxiety when symptoms are intense, Mahon says. Looking into support networks, both online and in-person, could be another important step for patient support, she adds. Like care for any kind of condition, chronic or not, simply listening can also go a long way, adds Plevny, particularly when a patient is talking about feeling down or defeated. “There’s something to be said for finding a doctor who will listen when you say your mental health is being negatively impacted, and who trusts your knowledge of your body and mind,” she says. “That helps me, and would help anyone, be better able to manage this disease.” from https://ift.tt/CfcIxE1 Check out https://takiaisfobia.blogspot.com/ How did U.S. exercise trends go from reinforcing white supremacy to celebrating Richard Simmons? That evolution is explored in a new book by a historian of exercise, Natalia Mehlman-Petrzela, author of the book Fit Nation: The Gains and Pains of America’s Exercise Obsession, out Jan. 2023. Nowadays, at the beginning of every New Year, many Americans hit the gym to work off their holiday feasts. This momentum usually starts to fade in mid-January, according to a 2019 analysis of data on fitness tracking apps by Bloomberg. But such new year’s resolutions are pretty new—as is the concept of exercise as a way to improve bodily health. “It’s really not until the 1980s that you start to have a consensus that everybody should be doing some form of exercise,” says Mehlman-Petrzela, a professor at the New School in New York City. That’s partly the result of the women’s movement of the 1960s and 1970s, which fought for Title IX, allowing girls to play school sports. That pushed back on notions that girls and women aren’t capable of doing vigorous exercise because they’re fragile. Perfect for reading on the treadmill or stationary bike, the below conversation with Mehlman-Petrzela outlines the earliest ideas on exercise, delves into the history of various popular workouts, and the outsize influence of Richard Simmons. Your book Fit Nation starts out by talking about how fat was something to aspire to and that was a sign of wealth and healthiness. How did Americans go from a mentality of “fat is good” to “skinny is better?” One of the things I set out to do in this book is to look at the change in how we think about our bodies and what’s considered attractive. Until the 1920s or so, to be what would be considered today fat or bigger, was actually desirable and actually signified affluence—which is like the polar opposite of today, when so much of the obesity epidemic discourse is connected to socio-economic inequality and to be fat is often to be seen as to be poor. How did that happen? Well, in a moment when actually there wasn’t a lot of access to caloric foods, to be fat showed that you could afford these things that were out of the reach of most people and also you could afford to rest, like you weren’t out there doing manual labor all day. As that caloric food became more accessible, and as more people were doing sedentary white-collar work and had access to cars and leisure, somebody who could resist those caloric foods, exercise, and have a thin body, was seen as more desirable. Read more: The history behind New Year’s resolutions to exercise more What’s the most surprising thing you learned in your research? It was super interesting reading the reflections of fitness enthusiasts in the early 20th century. They said we should get rid of corsets, corsets are an assault on women’s form, and that women should be lifting weights and gaining strength. At first, you feel like this is so progressive. Then you keep reading, and they’re saying white women should start building up their strength because we need more white babies. They’re writing during an incredible amount of immigration, soon after enslaved people have been emancipated. This is totally part of a white supremacy project. So that was a real “holy crap” moment as a historian, where deep archival research really reveals the contradictions of this moment. Your book talks about how, at one point, America’s focus was on exercising so we could have a population that was ready to go to war. What is health and fitness culture training us to do? How has that expectation evolved over time? During the New Deal [of the 1930s], the Civilian Conservation Corps would recruit out-of-work or impoverished, scrawny men to go work in the forest and on public works projects. One of the ways that they marketed this was “it puts muscles on your bones.” That really picked up during the Cold War. Right after World War II, you start to have more concern about Americans getting soft, this idea that the things that made America great—like cars and TV sets—were actually taking a toll on Americans’ bodies. Presidents Eisenhower and Kennedy went on a mission to make exercise look wholesome and patriotic and focus on shifting the purpose of exercise to being a good citizen and defending your country. In the 1980s, there’s a huge boom in the fitness industry, connected to this “work hard, play hard” mentality. I was also really moved speaking to gay men who had lived through HIV/AIDS and talked about how they exercised to display that they had a healthy body at a moment when there was so much homophobia. Some gyms became like community centers, sharing medical information, almost like mutual aid societies. Another big turning point is 9/11. You see a boom in the CrossFit mentality of almost like militarized fitness and girding yourself and your body for a fight—not necessarily, by the way, in the 1950s/1960s way of fighting for the U.S. Army—but more like “you need to know how to perform functional fitness to protect yourself if things go wrong.” At the same time, you see [an emphasis on] wellness, self care and healing and being meditative in an increasingly traumatic and unpredictable world. Read more: The big business of being a Peloton instructor What era of fitness are we in now? Gym usage is rebounding rapidly since the pandemic [lockdown ordinances], but now it’s also really efficient for a lot of people to exercise at home. What’s so unfortunate about the pandemic is how much it accelerated fitness inequality. You can go home and be on your Peloton if you can afford it, if you have the space for it, but not everyone can. I was meeting with somebody who’s very active in the New York City pickleball world, and you have all of these adults who want to do this inclusive recreational thing, and they’re competing with children who want to go out and skateboard and do basketball. Those are wonderful things, and we don’t have the public space to accommodate them. Did you find an exercise that people don’t do now, but they did do in a certain period of history, that’s just comical to think about? “Reducing machines” are a really good example of an exercise machine that just went away. Well into the 1960s, women were not encouraged to do any kind of strenuous exercise, but they were of course encouraged to do whatever it took to be beautiful and slim. So you would either lie down like on a bed or stand with a belt around you, and the machines would shake your fat. They were meant to enhance circulation but also to shake away cellulite. Reducing machines were everywhere; people would buy them for their houses. There was one called the “magic couch” that every woman wanted for Christmas. The idea that all bodies can exert themselves and work hard—including women’s bodies— is a really positive development, and it’s one of the reasons that you don’t see those passive exercise machines anymore. 
How did running become a popular exercise in the 1970s? It’s often hailed as a great equalizer, an exercise everyone can do with hardly any gear required? Did you find that to be the case? It became popular among environmentalists, people who were imagining what it would be like to be in a culture that was not centered around cars. The sneakers back then were pretty rudimentary—old work shoes with rubber soles. But it’s important to point out that access was never totally equal, if you lived in a neighborhood that didn’t have safe streets or streets that were not well lit. Women were catcalled. People of color were thought to be committing a crime. The “running is for everybody” discourse still quite often leaves out the fact that depending on where you live and the body that you live in, it can be a very different kind of experience. Read more: 3 things you didn’t know about running Your book has so many interesting stories about the origins of various workouts. I learned that Pilates can be traced all the way back to World War I, when its founder, Joseph Pilates was detained on the Isle of Man and created resistance contraptions out of hospital beds to help prisoners of war keep up their muscle strength. How can the influence of Pilates be seen in today’s fitness culture? That sets the foundation for the idea that exercise isn’t an indulgent little hobby some people have; it’s actually something that can keep you healthy. Joseph Pilates came to the United States, developing this system that he first called “Contrology,” and he became really an important part of the dance and performance community. And that did a lot to raise the bar on what fitness represented because, as I talk about at length, a lot of the cultural associations with fitness were like dank gymnasiums and big muscular men heaving weights. It sounds like Pilates made exercise seem like something that could be graceful too. Yes, Pilates’ studio on Eighth Avenue in Manhattan was [patronized by] opera stars and ballet dancers who are working on their bodily strength, so that did a lot to sanitize and upgrade the reputation of fitness. A lot of people embraced exercise as something that could make them look like a dancer. Read more: Here are the health benefits of Pilates 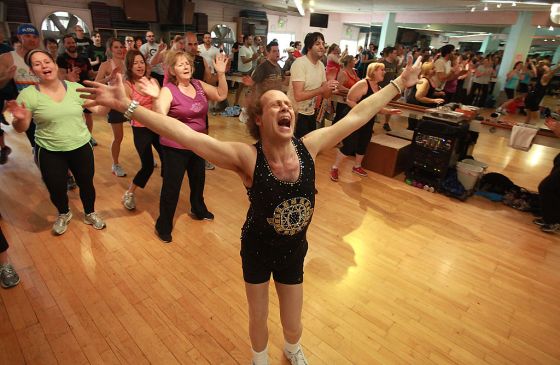
Going into this book, the only famous fitness instructor I had heard of was Richard Simmons. How influential was he? He’s really important in terms of shifting who was welcome in gyms. One of the reasons that he ended up starting his own studio is that he went to this very famous studio Gilda Marx, and he absolutely loved aerobics, but he was asked not to come back because women didn’t feel comfortable working out with a man who was singing and so emotive during his workout. And I think he opened a studio where everybody felt welcomed there, including fat people, who felt like they couldn’t step foot into a health club or a studio to take an aerobics class because no one looked like them there. Today, you see quite a few fat people in the fitness industry, who are operating from a better perspective, which is that your body size does not necessarily dictate your fitness level. We should not presume that because you are fat, that you are not fit or that you want to lose weight. And I think that we probably couldn’t have had that without Richard Simmons. What’s the future of fitness? I would love for the future of fitness not only to be about [WiFi] connected treadmills and luxury clubs where people can go hang out and drink green juice after their workout, but rather for a collective public investment in making fitness and recreation available to everybody and much more accessible than it currently is. We do agree as a culture, for the most part, that exercise is good for you, but our policy environment has not caught up with that. We should acknowledge that that’s one of the few things that we can agree on in our culture, and then have a kind of bipartisan shared investment in better physical education, better recreation [spaces] for kids and adults. from https://ift.tt/kmK2Jid Check out https://takiaisfobia.blogspot.com/ Federal guidelines say U.S. adults should get at least 75 minutes of vigorous physical activity, or 150 minutes of less-intense activity, each week. But over the past few years, a slew of studies have promoted the benefits of getting much, much less exercise than that. One 2022 study found that squeezing in just three one-minute bursts of vigorous activity each day could lead to a longer life. Another study, also published in 2022, linked 15 minutes of weekly physical activity to extended longevity. A 2019 paper went even further, arguing that just 10 minutes of weekly movement could help you live longer. These results are tantalizing—but also may seem a little too good to be true, given long-standing activity guidelines that recommend getting roughly 10 times as much exercise to stay healthy. “There are probably people out there who are looking at this and saying, ‘Well, I’m not sure I buy that,’” says Stephen J. Carter, an assistant professor of kinesiology at the Indiana University Bloomington School of Public Health who researches exercise and aging. “But maybe we ought to be thinking about exercise differently.” Any amount of movement is better than none, Carter says, and it takes surprisingly little to benefit your health. How short bursts of activity benefit your healthWhen you put stress on your body through exercise, even for a short time, you trigger physiological changes, says Malia Blue, an assistant professor of exercise and sport science at the University of North Carolina at Chapel Hill. Even small doses of activity can increase blood flow and improve the body’s ability to regulate blood-sugar levels. Over time, these changes could reduce your risks for conditions such as diabetes, heart disease, and stroke, Blue says. When your muscles are active, they also release compounds that can improve the health of organs throughout your body, says Kevin Murach, an assistant professor at the University of Arkansas who researches muscle biology. Plus, by getting up and moving—even for just a minute—you’re interrupting sedentary time, Blue says. Research has shown that sitting too much is bad for your health, and that replacing virtually any amount of sedentary time with movement is beneficial. “There’s a kind of a twofold [benefit]: if you break up your sedentary time and you increase your physical activity, you’re going to see health benefits from both,” Blue says. People who exercise in hopes of losing weight or training for a specific athletic event probably won’t get dramatic results with a few minutes per day. But that doesn’t mean you aren’t benefiting from those short spurts of movement. “People want that instant gratification and frankly, that’s just not possible with exercise,” Carter says. “You might not look like the YouTuber” leading your workout after a five-minute class, “but you’re doing yourself a bit of good.” Studies back that up: One widely cited research review from 2014 demonstrated that cardiorespiratory fitness is a better predictor of mortality than body mass index. That finding shows exercise can benefit your health at any size. The benefits also extend beyond your physical body, as many studies have shown that movement benefits mental well-being. The benefits can be hard to quantifyMurach agrees that even a little exercise can improve your health, but he says it’s important to be cautious when interpreting studies on bite-sized workouts. Often, studies capture only a snapshot of time rather than participants’ entire lives, Murach says. Some studies also don’t do a great job of teasing out whether exercise caused certain health benefits or is simply correlated with them. “I’m sure there is a benefit,” Murach says. “But if you’re doing a minute of exercise a day, is that going to be the silver bullet for extending your lifespan?” That’s harder to know for certain, he says. Another complicating factor is that people start from different baselines. For someone who is entirely sedentary, adding even a short amount of exercise per week might be a fairly dramatic change. But for someone who is already exercising sporadically, it will likely take more than a few extra minutes to achieve additional health boosts. Intensity and duration matterAll exercise isn’t equal, either. Sprinting at all-out intensity for five minutes will have a different effect on your body than taking a leisurely five-minute stroll. That’s not to say light or moderate activity isn’t beneficial. In the London Transport Workers Study, which began in the 1940s, researchers found that train conductors had lower rates of coronary heart disease than drivers, seemingly because they had more active jobs. Those results—and many studies performed in the decades since—suggest that even moderate activity that might not be consider traditional “exercise,” like housework or walking, can have a positive impact. But intensity does matter, especially if you’re only moving for a short time. Compared to more moderate activities, vigorous moves that get the heart pumping, like running or doing jumping jacks, more efficiently trigger physical benefits, Carter says. Two of the strongest exercise-related predictors of longevity--grip strength and aerobic capacity—may improve modestly after short workouts, but likely take longer, more intense bouts of movement to improve significantly, Murach says. Large studies have shown that the benefits of exercise compound as you do more, so there’s no reason to stop at a few minutes if you have the time and ability to continue. The good news is that activity is both variable and scalable. Your vigorous workout may be someone else’s light workout—but as long as your heart rate is up and your breathing is a bit labored, you’re doing your body good, Carter says. You can also build intensity over time, research suggests. Perhaps you start by taking short walks a few times a day, then ramp up to more vigorous movement, done for longer stretches, as you get stronger, Blue says. The takeaway is that some exercise is always better than none, and every additional bit adds up. “It’s pretty shocking, the amount of health benefit you can get from even short little bouts of exercise,” Murach agrees. “It may not be the thing that makes you lose 30 pounds, but it can improve your health in some capacity—your physiological health as well as your mental health.” from https://ift.tt/sXe87pg Check out https://takiaisfobia.blogspot.com/ BEIJING (AP) — Chinese authorities are going door to door and paying people older than 60 to get vaccinated against COVID-19. But even as cases surge, 64-year-old Li Liansheng said his friends are alarmed by stories of fevers, blood clots and other side effects. “When people hear about such incidents, they may not be willing to take the vaccines,” said Li, who had been vaccinated before he caught COVID-19. A few days after his 10-day bout with the virus, Li is nursing a sore throat and cough. He said it was like a “normal cold” with a mild fever. China has joined other countries in treating cases instead of trying to stamp out virus transmission by dropping or easing rules on testing, quarantines and movement as it tries to reverse an economic slump. But the shift has flooded hospitals with feverish, wheezing patients. The National Health Commission announced a campaign Nov. 29 to raise the vaccination rate among older Chinese, which health experts say is crucial to avoiding a health care crisis. It’s also the biggest hurdle before the ruling Communist Party can lift the last of the world’s most stringent antivirus restrictions. China kept case numbers low for two years with a “zero-COVID” strategy that isolated cities and confined millions of people to their homes. Now, as it backs off that approach, it is facing the widespread outbreaks that other countries have already gone through. The health commission has recorded only six COVID-19 fatalities this month, bringing the country’s official toll to 5,241. That is despite multiple reports by families of relatives dying. China only counts deaths from pneumonia or respiratory failure in its official COVID-19 toll, a health official said last week. That unusually narrow definition excludes many deaths other countries would attribute to COVID-19. Experts have forecast 1 to 2 million deaths in China through the end of 2023. Read more: What China’s Zero-COVID Policy Means for the Pandemic—in China and the Rest of the World Li, who was exercising at the leafy grounds of central Beijing’s Temple of Heaven, said he is considering getting a second booster due to the publicity campaign: “As long as we know the vaccine won’t cause big side effects, we should take it.” Neighborhood committees that form the lowest level of government have been ordered to find everyone 65 and older and keep track of their health. They are doing what state media call the “ideological work” of lobbying residents to persuade elderly relatives to get vaccinated. In Beijing, the Chinese capital, the Liulidun neighborhood is promising people over 60 up to 500 yuan ($70) to get a two-dose vaccination course and one booster. The National Health Commission announced Dec. 23 the number of people being vaccinated daily had more than doubled to 3.5 million nationwide. But that still is a small fraction of the tens of millions of shots that were being administered every day in early 2021. Older people are put off by potential side effects of Chinese-made vaccines, for which the government hasn’t announced results of testing on people in their 60s and older. Li said a 55-year-old friend suffered fevers and blood clots after being vaccinated. He said they can’t be sure the shot was to blame, but his friend is reluctant to get another. “It’s also said the virus keeps mutating,” Li said. “How do we know if the vaccines we take are useful?” Read more: Bivalent COVID-19 Boosters Help Keep Older People Out of Hospitals, CDC Says Some are reluctant because they have diabetes, heart problems and other health complications, despite warnings from experts that it is even more urgent for them to be vaccinated because the risks of COVID-19 are more serious than potential vaccine side effects in almost everyone. A 76-year-old man taking his daily walk around the Temple of Heaven with the aid of a stick said he wants to be vaccinated but has diabetes and high blood pressure. The man, who would give only his surname, Fu, said he wears masks and tries to avoid crowds. Older people also felt little urgency because low case numbers before the latest surge meant few faced risk of infection. That earlier lack of infections, however, left China with few people who have developed antibodies against the virus. “Now, the families and relatives of the elderly people should make it clear to them that an infection can cause serious illness and even death,” said Jiang Shibo of the Fudan University medical school in Shanghai. More than 90% of people in China have been vaccinated but only about two-thirds of those over 80, according to the National Health Commission. According to its 2020 census, China has 191 million people aged 65 and over — a group that, on its own, would be the eighth most populous country, ahead of Bangladesh. “Coverage rates for people aged over 80 still need to be improved,” the Shanghai news outlet The Paper said. “The elderly are at high risk.” Du Ming’s son arranged to have the 100-year-old vaccinated, according to his caretaker, Li Zhuqing, who was pushing a face-mask-clad Du through a park in a wheelchair. Li agreed with that approach because none of the family members have been infected, which means they’d be more likely to bring the disease home to Du if they were exposed. Health officials declined requests by reporters to visit vaccination centers. Two who briefly entered centers were ordered to leave when employees found out who they were. AP researcher Yu Bing and video producers Olivia Zhang and Wayne Zhang contributed. from https://ift.tt/7IBbhZN Check out https://takiaisfobia.blogspot.com/ It is fortunate that, in a majority of cases, kidney cancer is caught before spreading to other parts of the body. For these patients, treatment usually involves a nephrectomy, which is the surgical removal of one or both of the kidneys. The goal of the surgery is to prevent the cancer from metastasizing. Unfortunately, many people who undergo a nephrectomy for high-risk disease—between 20% to 50%, according to recent estimates—will eventually go on to develop metastatic cancer. Until recently, there wasn’t much a person’s care team could do in this situation to stop the cancer from coming back. Reliably effective “adjuvant” immune therapies—something added to surgery to prevent the cancer’s return—had not yet been identified. But in 2021, the New England Journal of Medicine published the results of a groundbreaking clinical trial. The trial involved roughly 1,000 people undergoing nephrectomy who were at high risk for cancer recurrence. About half of the people took a placebo pill, while the other half took a kidney cancer drug called pembrolizumab. Pembrolizumab is an immune checkpoint inhibitor—a type of immunotherapy drug that stimulates the immune system to fight cancer cells. After two years of follow-up, the people in the trial who took the immunotherapy drug were significantly less likely to have had a cancer recurrence than those taking the placebo. A few months later, the U.S. Food and Drug Administration (FDA) approved pembrolizumab as a form of adjuvant therapy. “This was a win-win situation,” says Dr. Toni Choueiri, one of the leaders of that trial and director of the Lank Center for Genitourinary Oncology at the Dana-Farber Cancer Institute in Boston. Not only did the people involved in the trial benefit from the drug, but the experiment’s findings also helped expand the medical community’s knowledge of the disease and its arsenal of weapons. Clinical trials like the one Choueiri led are happening all the time across the country. They are a necessary step—and usually the final step—in the development of new medicines for the treatment of kidney cancer. But they don’t always involve drugs. Clinical trials are also used to vet the effectiveness of new surgical techniques, new diagnostic procedures, and anything else that could improve the lives of people with kidney cancer. While some trials break new ground, others examine small changes to the existing standards of care—such as adjusting the dose of a drug up or down, or changing the way treatment side-effects are managed. In all cases, a trial’s results help shape the way every person who develops kidney cancer is treated, and so their importance cannot be overstated. Here, Choueiri and other kidney cancer specialists detail the latest developments in the trial landscape. They also explain who is eligible to participate in clinical trials, how enrollment in a trial works, and how trials have helped revolutionize the field of kidney cancer medicine. Mapping the current trial landscapeKidney cancer doesn’t respond well to conventional cancer treatments, such as standard radiation or chemotherapy. As recently as 2005, there was only one type of medication—an immunotherapy medicine called interleukin-2—that had FDA approval for the curative treatment of kidney cancer. Thankfully, the situation today is much different. “We now have more than a dozen FDA-approved drugs, and every single one of them has been approved and is available because of randomized clinical trials,” says Dr. James Brugarolas, director of the Kidney Cancer Program at the University of Texas Southwestern Medical Center in Dallas. Brugarolas is involved in translational research, which aims to bring scientific discoveries made in the lab or in animal models into the realm of human medicine. Some of his recent work has involved a transcription factor called HIF-2. A transcription factor is basically a protein molecule that controls the activity of a gene, and HIF-2 regulates a gene that affects the growth of kidney cancer tumors. For years, there was speculation that blocking the activity of HIF-2 could stop or slow the growth of kidney cancer. However, because of HIF-2’s unusual structure, typical drugs could not bind to it. HIF-2 was basically “undruggable,” Brugarolas says. But several years ago, researchers at UT Southwestern identified a cavity in an HIF-2 protein that could be exploited with specially designed drugs. Brugarolas has helped develop those drugs, which are called HIF-2 inhibitors, and a series of clinical trials has demonstrated that they are effective for several types of kidney cancer. “Very few cancer drugs target transcription factors, so this is a new paradigm,” he says. Brugarolas notes that clinical trials on HIF-2 inhibitors are ongoing, and similar trials are looking at many other novel drug treatments. Like other forms of cancer, kidney cancer isn’t really one disease, he says. It’s more accurate to call it a family of related cancers that have diverse characteristics. Some of his other work, including clinical trials he’s led, has examined these characteristics to determine how certain patient groups will respond to certain therapies. While some clinical trials examine groundbreaking new treatments, others involve new cocktails of existing drugs. This sort of “combination therapy” is an especially active area of kidney cancer research, says Dr. Eric Jonasch, a kidney cancer specialist and professor of genitourinary medical oncology at MD Anderson Cancer Center in Houston. A handful of combinations have already received FDA approval. “More combinations are coming down the pipeline, and not just doublets, but triplets.” Not all the trial work is concerned with drug treatments. “There have been advancements in surgical techniques, such as robotic surgery,” Jonasch says. A specialized type of radiation therapy is another promising area of research. “The ability to focus radiation while minimizing collateral damage has significantly improved,” he says. Radiation could offer improvements over broader “systemic” treatments for people with kidney cancers that have metastasized. “It could even treat kidney tumors themselves without surgery,” he adds. The benefits of all this trial work are significant—and quantifiable. “Kidney cancer is a disease where, maybe 15 years ago, someone diagnosed with stage 4 disease had just one year to live, and now the average is closer to five years,” Choueiri says. The next decade is sure to bring more substantial improvements in the lives and longevity of people with kidney cancer. But to get there, clinical trials need participants. Read More: Coping With the Side Effects of Kidney-Cancer Treatment The benefits of participating in a clinical trialThe precise risks and rewards of clinical trial participation will vary from one patient—and trial—to the next. But broadly speaking, experts say there are two compelling reasons for people with kidney cancer to take part in this type of medical research. “Number one, trial participation may give patients the opportunity to access therapies that might not otherwise be accessible to them,” Jonasch says. In nearly all cases, the cost of these therapies—which can be considerable—will be picked up by the companies or institutions running the trial. For those who may be concerned about trying an experimental treatment, Jonasch says that every clinical trial must be approved by a review board—an unaffiliated group of experts who scrutinize the proposed trial to ensure that participants are not exposed to undue risks. “Because of how ethical boards function today, you’re very likely going to get something that is either equivalent or superior to standard care,” he says. Research in the Journal of the National Cancer Institute has found that people with cancer who participate in clinical trials tend to fare slightly better than those who don’t. Especially for those with advanced cancers with a poor prognosis, trial participation can be beneficial, that study found. It’s not an exaggeration to say that taking part in a clinical trial has meant the difference between life and death for some participants. “I have a lot of patients who were involved in clinical trials of small-molecule [drugs] or immunotherapies who, if they had gotten the standard of care back then, would not be alive right now,” Choueiri says. Another benefit to trial participation is the impact its findings have on the cancer community. “You’re contributing to the expansion of our knowledge of the disease, and you’re helping in the development of therapies that will benefit other patients,” Jonasch says. One of the tragedies of cancer is that, in many cases, it robs the world of all the good someone may have done had their life not been disrupted or cut short by the disease. “For many patients, life has been significantly undermined by cancer, and they may appreciate the opportunity to help other people who have the same disease,” Brugarolas says. Read More: The Latest Breakthroughs That Could Improve Kidney Cancer Treatment How to take part in a clinical trialThe first step is to ask your care team if you may be a good candidate for a clinical trial, Choueiri says. Referral from a cancer specialist or physician is the most common route to trial enrollment. However, you may also have to do a little research on your own. “The entire field of oncology, not just kidney cancer, is expanding at a rate where it’s very hard to know everything that’s going on,” Choueiri says. If you’re not being treated at a major research hospital or health system, your care team may not be aware of trials that could benefit you. There are a variety of ways to find trials on your own. “Visit ClinicalTrials.gov,” Jonasch suggests. This is a comprehensive database of clinical trials taking place in the U.S. and in other parts of the world. You can search it based on your type of cancer and your location, and it could help you find trials that are worth flagging to your doctors. Jonasch also recommends connecting with kidney cancer patient advocacy organizations, such as the Kidney Cancer Association and the International Kidney Cancer Coalition, to ask about clinical trials. “These groups can be a tremendous resource for navigating these waters,” he says. Finally, he says there is an especially great need for more trial participation among people of color, who are not always appropriately represented in this work. He blames problems of access and recruitment for these shortfalls. “We’re not getting it right yet, but there are efforts underway to ensure we’re reaching out to communities that may not have access to clinical trials,” he says. “It’s extremely important that we have representative diversity to ensure we understand the effects in all patient groups.” Clearly, there’s a lot going on in the trial space for kidney cancer. It’s a safe bet that more breakthroughs may soon follow. from https://ift.tt/TmVOB8I Check out https://takiaisfobia.blogspot.com/ A recent Consumer Reports investigation struck fear into the hearts of chocolate lovers everywhere. After testing 28 dark chocolate bars, scientists detected the heavy metals lead and cadmium in all of them. For 23 of the chocolate bars, eating just an ounce would put an adult above the daily upper threshold recommended for heavy metals in food by public-health officials in California, which the authors said they chose because it is the most protective standard available. Experts say, however, that this report offers just one small window into a larger problem. Heavy metals are detectable in many different foods, and limited testing and a lack of labeling requirements leave consumers in the dark. But there are steps you can take to limit your exposure and protect your family. What are the risks of eating foods containing heavy metals?Some metals, like iron, are essential for your health. Others, like lead and cadmium, serve no useful purpose for the body in any amount and are toxic in large quantities, according to the U.S. Centers for Disease Control and Prevention (CDC). No level of lead, for instance, is considered safe, but it becomes more dangerous as it accumulates in the body. The gravest risks are for children, since their bodies are small and still developing. According to the CDC, lead exposure can affect nearly all organ systems, but is particularly dangerous for the central nervous system, which includes the brain. A blood concentration as low as 10 µg/L can slow children’s neural development. In both children and adults, lead can also affect memory and cause conditions like anemia, stomach issues, and high blood pressure. Exposure to cadmium over a long period, meanwhile, can lead to stomach problems and may damage kidneys, in both children and adults. The recent finding that lead makes its way into popular chocolate bars didn’t surprise Dr. Robert Wright, a professor of environmental medicine at the Icahn School of Medicine at Mount Sinai. Some contamination is inevitable. Since dark chocolate is not a staple food and therefore, you (and especially children) are probably not eating it that much to being with, Wright says he wouldn’t discourage enjoying it in moderation (although he suggests that parents not feed their kids the brands that Consumer Reports says have the most lead and cadmium). Wright adds that he hopes that dark chocolate’s time in the headlines will lead companies to take a closer look at why some bars have more heavy metals than others. Why are there heavy metals in food?Many heavy metals, including lead and cadmium, appear naturally in soil, and they make their way into the food supply from the ground. But some have been added to the environment by human activity globally, including pollution caused by farming, industry, and transportation. For instance, lead was used in gasoline in the U.S. for decades until it was banned in 1996, and it spread through the atmosphere and settled on the ground, where it remains in the soil to this day, says Wright. “There are measurable amounts [of heavy metals] in pretty much all foods,” he says, “simply because there are metals in our soil.” The FDA has cautioned the public about the potential for unsafe amounts of heavy metals in other foods, including mercury in fish and arsenic in rice. Mercury is commonly found in fish due in part to runoff from natural causes, like volcanic eruptions, and as a waste product of certain human activities, like burning coal for fuel, burning municipal waste, and as runoff from industrial processes like electrical equipment manufacturing. Rice, meanwhile, tends to absorb arsenic from the soil and water in which it grows. Arsenic also occurs naturally, as part of the earth’s crust, and as a result of human activities, like pesticide use. So, should I stop eating dark chocolate?There are two main reasons not to fixate on chocolate, says Katarzyna Kordas, an associate professor of public health at the University at Buffalo. First, the reality is that heavy metals are probably present in trace amounts in many different foods. While the FDA tests a limited number of foods each year, including a few hundred annually for the Total Diet Study, it does not test food from specific brands or stores, and manufacturers are not required to disclose heavy metals on food labels. “There have been calls for better labeling and more transparency about what is in manufactured products. To do this, companies would need to test their products regularly and both make this information available and act on it to reduce heavy metals to the extent possible,” says Kordas. “It should not just be up to individuals to figure this out.” But in the meanwhile, it doesn’t really make sense to harp on one food type. And that leads to Kordas’ second reason for not giving up on dark chocolate: if you do, you may miss out on the health benefits that have been connected to moderate consumption on the stuff. For example, studies show that the flavonols in dark chocolate can promote heart health. How can I protect myself and my family from heavy metals in food?It’s key to note that heavy metals can accrue in the body not just from food, but also from exposure to contaminated water, the air, and household and consumer products, says Wright. In other words, no matter what you do about your diet, it’s unlikely you will completely avoid them. But, you can definitely take steps to reduce your risk of dangerous levels of exposure. Kordas says that instead of trying to avoid certain foods, for most people, it’s best to aim for a diet that contains a wide variety of foods, and to avoid eating a ton of any one food, Doing so “would lower our chances of sort of consuming too much of any one metal.” A healthy, balanced diet is also thought to offer protection from heavy metals. If your body is deficient in heavy metals that are healthy in low amounts—like zinc and copper—it may absorb too many dangerous heavy metals like lead and cadmium, says Wright. And the CDC recommends that children eat diets rich in calcium, iron, and vitamin C, all of which can keep the body from absorbing lead. Overall, a healthy diet also makes bodies stronger, says Wright, and will promote the development of your child’s brain, which will help to counteract the effects of negative factors in their environment. from https://ift.tt/ZSdBbXA Check out https://takiaisfobia.blogspot.com/ Companies Are Adding Sesame to Foods. Its an Unintended Consequence of a New Allergen Label Law12/21/2022 A new federal law requiring that sesame be listed as an allergen on food labels is having unintended consequences—increasing the number of products with the ingredient. Food industry experts said the requirements are so stringent that many manufacturers, especially bakers, find it simpler and less expensive to add sesame to a product—and to label it—than to try to keep it away from other foods or equipment with sesame. As a result, several companies—including national restaurant chains like Olive Garden, Wendy’s and Chick-fil-A and bread makers that stock grocery shelves and serve schools—are adding sesame to products that didn’t have it before. While the practice is legal, consumers and advocates say it violates the spirit of the law aimed at making foods safer for people with allergies. “It was really exciting as a policy advocate and a mom to get these labels,” said Naomi Seiler, a consultant with the Asthma and Allergy Foundation of America whose 9-year-old daughter, Zoe, is allergic to sesame. “Instead, companies are intentionally adding the allergen to food.” The new law, which goes into effect Jan. 1, requires that all foods made and sold in the U.S. must be labeled if they contain sesame, which is now the nation’s ninth major allergen. Sesame can be found in obvious places, like sesame seeds on hamburger buns. But it is also an ingredient in many foods from protein bars to ice cream, added to sauces, dips and salad dressings and hidden in spices and flavorings. Advocates for families coping with allergies lobbied for years to have sesame added to the list of major allergens. Congress in 2004 created labeling requirements for eight: milk, eggs, fish, shellfish, tree nuts, peanuts, wheat and soybeans. More than 1.6 million people in the U.S. are allergic to sesame, some so severe that they need injections of epinephrine, a drug used to treat life-threatening reactions. Cases of sesame allergy have been rising in recent years along with a growing number of foods that contain the ingredient, said Dr. Ruchi Gupta, a pediatrician and director of the Center for Food Allergy & Asthma Research at Northwestern University. “Sesame is in so many things that people don’t really understand,” said Gupta, who called the move to add sesame to products “so disappointing.” “In families that do have a sesame allergy, it is truly challenging,” she said. Under the new law, enforced by the Food and Drug Administration, companies must now explicitly label sesame as an ingredient or separately note that a product contains sesame. In the U.S., ingredients are listed on product packaging in order of amount. Sesame labeling has been required for years in other places, including Canada, Europe, Australia and New Zealand. If the ingredients don’t include sesame, companies must take steps to prevent the foods from coming in contact with any sesame, known as cross-contamination. Food industry experts said the new requirements aren’t simple or practical. “It’s as if we’ve suddenly asked bakers to go to the beach and remove all the sand,” said Nathan Mirdamadi, a consultant with Commercial Food Sanitation, which advises the industry about food safety. Some companies include statements on labels that say a food “may contain” a certain product or that the food is “produced in a facility” that also uses certain allergens. However, such statements are voluntary, not required, according to the FDA, and they do not absolve the company of requirements to prevent cross-contamination. Instead, some companies have taken a different approach. Officials at Olive Garden said that starting this week, the chain is adding “a minimal amount of sesame flour” to the company’s famous breadsticks “due to the potential for cross-contamination at the bakery.” Chick-fil-A has changed its white bun and multigrain brioche buns to include sesame, while Wendy’s said the company has added sesame to its French toast sticks and buns. United States Bakery, which operates Franz Family Bakeries in California and the Northwest, notified customers in March that they would add a small amount of sesame flour to all hamburger and hot dog buns and rolls “to mitigate the risk of any adverse reactions to sesame products.” Although such actions don’t violate the law, the FDA “does not support” them, the agency said in a statement. “It would make it more difficult for sesame allergic customers to find foods that are safe for them to consume,” the statement said. Some large companies previously have added other allergens to products and updated their labels. In 2016, Kellogg’s added traces of peanut flour to some cookies and crackers, prompting protests. That’s frustrating and scary for parents like Kristy Fitzgerald of Crookston, Minnesota. She learned last spring that Pan-O-Gold Baking Co., which supplies breads to schools, health centers and grocery stores across the Midwest, was adding small amounts of sesame to its products, including those served at her daughter’s school. Six-year-old Audrey, in the meantime, has outgrown her allergy to sesame. Bob Huebner, food safety/quality assurance manager for Pan-O-Gold, told Fitzgerald in a string of emails that the company was forced to add sesame to the product and the label. “The unfortunate reality is that our equipment and bakeries are not setup for allergen cleanings that would be required to prevent sesame cross-contamination and was not an option for us,” Huebner wrote in an email to Fitzgerald. Huebner replied to an email from the AP but did not respond to questions about the company’s practices. Fitzgerald started an online petition protesting the move to add sesame. “At some point, someone is going to feed an allergic child sesame,” Fitzgerald said. “It makes me think the laws need to change to show that this is not an acceptable practice.” from https://ift.tt/GVE51wJ Check out https://takiaisfobia.blogspot.com/ |
Authorhttps://takiaisfobia.blogspot.com/ Archives
April 2023
Categories |
 RSS Feed
RSS Feed
