How a False Sense of Security and a Little Secret Tea Broke Down Taiwans COVID-19 Defenses5/21/2021 All it took to break down the world’s most vaunted COVID-19 defense was a little secret tea. After almost 18 months of nearly unblemished success keeping the coronavirus pandemic at bay—including the world’s longest streak of case-free days—Taiwan is now in the grip of its first major COVID-19 surge. Total cases, which had been below 1,300 through the entire pandemic, have surged to more than 3,100 in the span of a week. Many offices have sent workers home, the streets of the capital Taipei have cleared out and the government has begun scrambling to secure vaccines to improve one of the worst inoculation rates in the developed world. The outbreak likely began after spilling over from cargo plane crews. However, the bulk of the surge has been traced back to two sources: a local Lions Club International gathering, and tea houses in the red-light district of Taipei’s Wanhua neighborhood. The two clusters were at first thought to be unrelated—until a former president of the Lions Club revealed that he had visited one of the tea houses. The movements of the civic leader in his 60s, nicknamed by Chinese-language media “The Lion King,” show he had at least 115 contacts while potentially infectious—and reveal just how vulnerable the island of 23 million was to a major outbreak. After rapidly imposing world-leading infection control measures, Taiwan slowly began to let down its guard last summer. Crowds of thousands of people were allowed to return to concerts, baseball games and religious festivals. Large meals and family gatherings became increasingly common, and masks became rarer as months passed with no local infections. “Last year, we started to kind of go out, but deal with it in a careful way,” says Freddy Lim, a rockstar turned lawmaker who represents Wanhua in Taiwan’s legislature. “But this year, I think we forgot the part about being careful.” Taiwan’s outbreak is now proving to be a test of whether a society relatively untouched by COVID-19 can effectively put to use the lessons the rest of the world learned the hard way. 
How Taiwan’s COVID-19 defenses failedTaiwan’s fight against COVID-19 began on Dec. 31, 2019—the day the first reports emerged of a mysterious viral pneumonia in Wuhan, China. By Jan. 2, 2020, health officials began screening arrivals from mainland China. Authorities set up temperature checks and stronger border controls in the following weeks—before the World Health Organization had even confirmed that the virus was spread by human-to-human transmission. The self-ruled island, which is claimed by Beijing, implemented strict infection control measures at hospitals and was among the first places to close its borders to nearly all non-residents and order strict quarantines for anyone who did arrive. Masks were distributed to the population and made mandatory in places like mass transit by March. Meanwhile, police closely monitored travelers to ensure they adhered strictly to quarantines and contact tracers pried deeply into infected people’s movements to ensure close contacts were found and isolated. READ MORE: Taiwan Says It Tried to Warn the World About Coronavirus. Here’s What It Really Knew and When All of this meant that by mid-April 2020 Taiwan had only about 400 confirmed cases. At the same time, the U.S. was reporting more than 30,000 infections per day. The success was 17 years in the making, dating back to the 2003 SARS outbreak, which also originated in mainland China and killed dozens on the island, says Dr. Chen Chien-Jen, who served as Taiwan’s Vice President until last May. Chen, an epidemiologist and former health minister, helped to design and lead Taiwan’s COVID-19 control measures. So why did those protocols fail after holding out successfully through the worst of the pandemic? “Life will find its way out, as said in Jurassic Park,” Chen tells TIME. “The virus will always try to replicate, to mutate, and it becomes more and more infectious.” The majority of recent COVID-19 cases reported in Taiwan are the virus variant first found in the U.K., which scientists believe is more easily transmitted. Complicating this is the fact that many patients have only minor symptoms or none at all and don’t know they’re spreading COVID-19 until it’s too late. This appears to be what happened in the “Lion King” case. Dozens of people connected to the Lions Club cluster were infected by one or more carriers who believed it was safe to socialize. But, lax adherence to the island’s safety protocols also played a role. Taiwan’s current community outbreak began in April with cargo plane crews at the Novotel at Taipei’s Taoyuan International Airport. The hotel violated COVID-19 rules by housing quarantined flight crews and non-quarantine guests in the same building. In mid-April, Taiwan also lowered quarantine requirements for non-vaccinated flight crews from five days to just three. At least 29 cases are linked to the Novotel cluster, including hotel staff. Officials say cases in the Novotel cluster, the Lions Club cluster, and the cluster of cases in Wanhua’s red light district were all infected with the same strain of the coronavirus—suggesting they have a common source. Taiwan’s tea shops become a COVID-19 breeding groundChen, now a distinguished professor at the Academia Sinica in Taipei, also concedes that he and others behind Taiwan’s COVID-19 surveillance program never envisioned how the shadowy world of Taiwan’s hostess tea shops would be uniquely vulnerable to spreading COVID-19 like wildfire. Many of the Wanhua tea shops are relatively innocent: clients are mostly older men who have tea with middle-age hostesses who keep them company and make conversation. However, some reportedly operate as fronts for brothels and employ migrant women who are in Taiwan illegally. It’s not hard to see how COVID-19 would ricochet easily through such an environment. The shops are often poorly ventilated and dimly lit. It’s also common for patrons to “bar-hop” from shop to shop and mingle with multiple hostesses and other patrons. “There is no way that you can wear masks in the tea houses, no matter if it is with sex workers or a just normal tea houses because you are eating food, you are drinking tea and you are singing, and so on,” says Lim, the legislator for the area. Combine that with customers who aren’t eager to tell contact tracers—or their own families—that they visited such an infamous area, along with marginalized workers who may be hesitant to come forward, and the red-light district in Wanhua has become the catalyst for more than 1,000 of the infections reported across Taiwan. Chen says health officials didn’t believe the tea houses would be a problem because two previous cases where COVID-19 patients went to other so-called “adult entertainment” venues didn’t result in transmissions. 
Taiwan’s vaccine shortfallThe other major reason that COVID-19 has spiked so quickly in Taiwan is that the virus found virgin immune territory. Very few people have been exposed and thus very few have antibodies. Taiwan’s vaccination rollout has also been almost non-existent. The island received just 300,000 doses of the AstraZeneca vaccine before the outbreak and had been hard-pressed to administer even those, with less than 2% of the population immunized. That’s a number that stands out even in Asia, which has lagged much of the rest of the world in vaccine rollouts. The problem has been both supply and demand. The lack of virus on the island has meant most Taiwanese people see no urgency in getting vaccinated. Incidence of side-effects, including the very rare occurrence of blood clots for the AstraZeneca vaccine, have been heavily reported by local media. A YouGov survey in early May found that just 40% of Taiwanese people said they were willing to be vaccinated—second-lowest among 21 places polled around the world. Since the outbreak, demand for vaccines has increased dramatically.
Taiwan also waited until after COVID-19 vaccines were authorized by other regulators to begin striking deals to buy them, says Chen. By then, most of the first batches were long snapped up by other governments—many of which had helped fund their development. So while Taiwan has secured some 20 million doses of vaccine from various sources, it is farther back in the line than most developed economies. The government in Beijing, which views Taiwan as a breakaway province that must be reunited with the rest of China, has offered to provide vaccine doses, though Taiwanese officials accused the mainland of trying to sow confusion and discord with the offer. The U.S. has pledged to help once it releases its stockpile of millions of AstraZeneca doses. On Wednesday, 400,000 doses arrived from COVAX, the international vaccine distribution scheme. Taiwan’s two domestically developed vaccines may be more likely to fill the gap. The government has promised to begin rolling them out in July following the completion of Phase 2 safety trials, which have been carried out on 4,000 test subjects for each vaccine. Chen says that unpublished studies of the two vaccines show they provoke similar antibody levels to other vaccines that are already proven effective in fighting COVID-19. The government plans to authorize the vaccines before completing Phase 3 efficacy trials. 
Learning from the world’s mistakesThe government has responded swiftly to the surge in cases: It has opened testing centers in hotspots, restricted the size of gatherings, began enforcing mask mandates with hefty fines, shut down schools and urged residents to stay home. But Taiwan’s most effective weapon in fighting COVID-19 may be its people. Whereas most new surges around the world are met with increasing amounts of pandemic fatigue and lower levels of compliance with social distancing rules, most Taiwanese people have been—if anything—even more cautious than the government. As cases began to spike, people rushed supermarkets, clearing shelves of food and, yes, toilet paper. The usually teeming streets of Taipei are all but empty as most people choose to stay home. Many restaurants voluntarily closed or banned indoor dining, and those who kept their dining rooms open are now largely empty. Beating this COVID-19 wave has become a point of pride. After the government imposed Level 3 pandemic restrictions—one degree below a full lockdown—memes began to circulate on social media that vowed to quash the surge in short order. “Look world, Taiwan will only show you once how to remove a Level 3 alert in two weeks,” reads a popular boast. Ya-chu Chuang, a 28-year-old freelance stenographer, has been working from home, but could not avoid going into her workplace one day this week. When she arrived, she went through a routine that was new to her, but all-too familiar across the world for the last 18 months. She sprayed down her desk with alcohol and did everything she could to keep herself away from others in the office. She feels like it’s her duty to do what she can to help reduce the spread of COVID-19 as quickly as possible. “I know that we’re experiencing what happened abroad about a year ago,” she says. “As long as we all do what we can and follow the instructions, we will be able to overcome this crisis.” from https://ift.tt/3yEXKE2 Check out https://takiaisfobia.blogspot.com/
0 Comments
Everest South Base Camp lies at an altitude of 17,598 feet (5,364 m), but it is no refuge from the global pandemic. The Nepali Sherpas who, in normal times, share the camaraderie of climbers on the world’s highest mountain, now enforce strict social-distancing rules, remaining within their separate camps—indeed, mostly inside their own tents. “We have made a rule not to walk from one camp to another as some climbers have tested positive,” says Phunuru, a Sherpa guide. “If we see somebody new walking around our camp, we immediately start an inquiry.” Officially, there is no coronavirus here. “Around 100 people have scaled Everest last week and rest will be climbing this week,” Rudra Singh Tamang, director general of the Department of Tourism, tells TIME. “Everything is fine.” But many climbers say otherwise. “The COVID situation at [Base Camp] is a total s—storm,” American Gina Marie Han-Lee wrote in a Facebook post in late April. “I had no clue what I was flying into.” Other climbers, from Norway and the U.K., have tested positive and one local doctor—who declined to be named, citing official harassment—told TIME that “two dozen climbers have been evacuated from Base Camp to Kathmandu and they later tested positive at a hospital.” What happens on this remote, majestic mountain poses questions for tourism operators everywhere. Countries are making tentative attempts at reopening, but If the pristine environment at the roof of the world can’t be kept free of COVID-19, what chance is there for the beaches of Cancun, the bustling city squares of Europe, or the shopping malls of Asia, once travelers flock back to them? For poorer nations—and struggling communities like the Sherpas—that are heavily dependent on tourism, the developments at Everest are a bleak warning. 
Nepal’s COVID-19 CrisisTo be sure, the news from Base Camp is the least of Nepal’s worries right now. With the two countries sharing a porous, 1,100 mile (1,770 kilometer) land border, it was inevitable that the devastating wave of COVID-19 afflicting India should spread to its northern neighbor and overwhelm the feeble health care system. On May 20, Nepali authorities reported 8,227 new cases and 190 deaths, with the country’s total case tally approaching 488,700. The rate of 29 COVID-19 cases per 100,000 people in the last week has overtaken India’s 21. “We are running out of oxygen and hospital beds, we have a huge lack of health workers,” says Dr. Samir Adhikari of the Ministry of Health and Population. “Nepal cannot handle this situation anymore.” Even before the pandemic, it struggled to provide health care to its people. The latest available World Bank figures show that the country has less than one doctor per 1,000 people and only one hospital bed for every 3,000. Only 26 of the country’s 185 hospitals had oxygen plants, local media reported at the end of April, and of those not all were in working order. The situation is especially dire in remote areas, where isolated populations have very limited access to basic health care due to high cost and low availability. Given the tragic lack of resources, people are now dying on the streets, in ambulances, at hospital gates, or at home after failing to find treatment, and the disease is spreading virtually unchecked. Daily confirmed cases increased by over ten-fold from mid-April to mid-May, when more than 45% of tests conducted produced positive results. As with India, the holding of political rallies and religious festivals in recent months may have exacerbated the situation. Many Nepalis also believe the virus was spread by Indian workers transiting in Nepal en route to jobs in the Gulf states, when those states banned direct flights from India. For some exhausted front line health workers, the battle is already lost. “We are helpless,” says a despairing Dr. Subhah Panta, emergency medical officer at the Tribhuvan University Teaching Hospital. “People have two choices—go home or go to cremation.” At the hospital, a grieving Yadav Upreti tells TIME that his 50-year-old brother Radha Krishna Upreti died when his cylinder ran out of oxygen. “Radha Krishna was the only income source for the family, and I don’t know who will take care of his two small kids and wife now,” Upreti says. “It’s actually murder by the government, as it’s not able to give us basic treatment.” Many Nepalis accuse the authorities of failing to take the threat of a major outbreak seriously enough. The government has been riven by factional strife and Prime Minister K.P. Sharma Oli lost a vote of confidence on May 10. Besides being preoccupied with political survival, he also reportedly placed too much store in what he saw as the country’s natural defenses against COVID-19. According to local media, the prime minister believed coronavirus would not make much headway in Nepal because of the “strong” immune systems of Nepali people and the country’s “rich Ayurvedic traditions.” He has since walked back his position and was quoted on May 17 as saying “But now, (I realized) a normal immune system could not resist this.” With a rudimentary health system and an ill-prepared government, it’s unsurprising that no part of the country has been spared, whatever the elevation. In the humid, far western lowlands of the country, with a tropical and subtropical climate, Kailali forms as great a contrast as can be had to the mountainous, snow-covered Nepal of the popular imagination. At the district’s Tikapur Hospital, 26 COVID-19 patients died in a week due to a lack of oxygen. There are no available beds. “I have been giving phone treatment to more than 50 patients,” sighs Dr. Ramesh Prasad Upadhyay. “That’s what I can do for now.” Vaccination is not an immediate solution. Only 7% of Nepal’s 30 million people have been jabbed. Two million doses were ordered from India’s Serum Institute, the world’s largest producer of vaccines. But because of the crisis in India, New Delhi ordered a halt to vaccine exports, leaving Nepal a million doses short. As coronavirus tears through an unprotected population, the cremation teams work overtime. TIME counted 12 cremations during a brief, 30-minute visit to the Pashupati cremation center in Kathmandu. One of them was of Mohat Singh’s mother. “We can’t cremate her according to the proper rites,” he says, distraught, watching from a distance as Nepali troops carried out the grim task. “Two of my brothers are in isolation. COVID has destroyed our family.” At the Sukraraj Tropical and Infectious Disease hospital in Kathmandu, Dr. Sher Bahadur Pun, chief of the clinical research unit, says “Ninety-nine percent of people are dying from COVID because they did not get treatment.” Outside, 39-year-old Shanta Bhattarai says she has been waiting four days for admission. “It’s been five days since I tested positive,“ she tells TIME. “I have a fever and can’t breathe. Will I survive?” 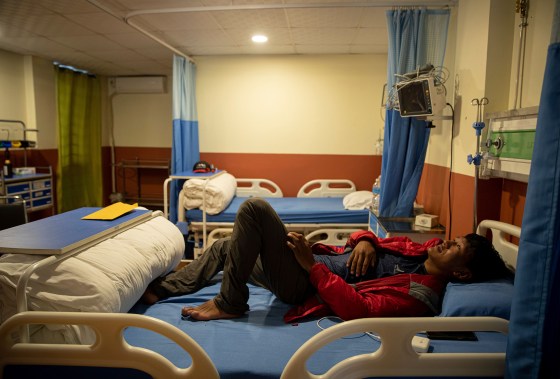
Tourism, Sherpas and the PandemicThe disastrous outbreak has meanwhile put any thought of economic recovery on hold. With eight of the ten highest mountains in the world, Nepal has long been an irresistible destination for serious mountaineers, rock climbers, and trekkers. Tourism is the largest industry, employing 800,000 people, and is the country’s main source of foreign exchange. In 2019, Nepal welcomed 2 million visitors, who parted with $724 million. Small wonder that the government began making strenuous attempts to reopen to adventurers at the end of last year, approving a record number of 408 Everest expeditions for 2021. Many climbers traveled to the country believing that Nepal’s first wave, in the second half of 2020, represented the peak of infections, and reasoned that they would be avoiding the riskier cities. Erlend Ness, a Norwegian climber who became the first person to test positive at Everest, wrote on Facebook that “the fact that I was going up in the mountain short time after arriving Kathmandu felt safe.” He wasn’t alone. This season, Base Camp has been crowded with some 1,300 climbers, Sherpas and support staff. For visitors and locals alike, Everest is the jewel in the crown. With mountaineers needing to pay $11,000 each for a climbing permit—to say nothing of the revenue generated by accommodating, transporting, guiding and feeding international expeditions—the lofty peak is Nepal’s single most lucrative attraction. Fees alone have generated nearly $4.2 million this year, according to information posted to Twitter by Mira Acharya, the director of the mountaineering division at the Department of Tourism. Much of that wouldn’t be possible without the Sherpas (the name derives from the words Shyar, or “East,” and Pa, or “People,” in their language). The ethnically Tibetan group numbers some 150,000 and is famed for producing elite mountaineers who have made immeasurable contributions to Himalayan exploration. But, even at the best of times, they struggle. “Basically, I earn $6,000 to $8,000 a year, which is just enough to live on” says one, Daring Sherpa, who has a family to support and like many of his community uses Sherpa as a last name. “If I don’t work this year, I won’t even be able to pay for food.” By “work,” he means mountaineering. There are hardly any other jobs in the uplands. Food costs five times what it does in Kathmandu because of the remoteness of the area and health facilities are scant. A sick Sherpa either has to walk into town or spend as much as $3,000—potentially half a year’s income—for a helicopter evacuation to the capital. “Sixty percent of Sherpas are working as guides because we don’t have other job options and because we are not formally educated,” Panaru Sherpa tells TIME. “Not all Sherpas are happy with climbing Everest,” he adds as one who has summited 12 times. “We are doing it for a living.” With the coronavirus now rampaging through Nepal, many are having sleepless nights as expeditions think about pulling the plug. Austrian expedition operator Furtenbach Adventures did so on May 15. To climb “with these massively increasing [COVID-19] numbers,” said its principal Lukas Furtenbach, “would be irresponsible.” Dadoma Sherpa’s 56-year-old husband, Dorje Sherpa, is still at work on the mountain—but “I haven’t been able to sleep after I heard that COVID reached Base Camp,” she tells TIME. “I’m trying to call my husband, but his phone isn’t reachable. One half of my heart says call him back home, and the other half says ‘If I call him back home, what are we going to eat?’ We have two kids studying. We will not be able to pay for their education if he comes home.” At Gorakshep, a collection of basic lodges that is the last stop on the trek up to Base Camp, hotel owner Pasang Sherpa understands the desperation. “If Sherpas don’t get work this year, they may die from hunger,” he says. Given the importance of Sherpas to the business of mountaineering, and the crucial role Himalayan expeditions play in Nepal’s economy, the ripple effects will be felt far beyond the snow-capped peaks. Perhaps this is the reason for the air of grim determination hanging over Base Camp, where a 19-year-old Sherpa guide has become one of the latest climbers to be stricken with a cough and a fever. “Even if it is COVID, I can’t go back home,” she says, asking not to be named. “I have to finish my mission.” from https://ift.tt/3bGVbHq Check out https://takiaisfobia.blogspot.com/ On May 20, the U.S. Food and Drug Administration extended the time that Pfizer-BioNTech’s COVID-19 vaccine can be stored in the refrigerator. The vaccine, which people get in two doses, still needs to be shipped frozen at ultra-cold temperatures in the companies’ special thermal shipping container. Doses can be kept frozen in these containers for up to 30 days as long as dry ice is used to maintain temperatures of around -70°C (-94°F). Once thawed, the vaccine doses can now be kept in a refrigerator for up to one month. Previously, the emergency use authorization issued by the FDA only allowed the vaccine to be stored, thawed, in a refrigerator for five days. The longer refrigeration time was authorized by the FDA after the agency reviewed data provided by Pfizer-BioNTech showing the vaccine remained stable and viable under refrigerated conditions for up to one month. More pharmacies, doctors’ offices and smaller health centers have access to refrigeration than they do the ultra-cold freezers required for longer term storage of the Pfizer-BioNTech vaccine, so the FDA’s decision will give those who are now administering vaccines more flexibility in managing their doses. The FDA also recently allowed children as young as 12 to get vaccinated, and the federal government is shipping vaccines directly to pediatricians’ and doctors’ offices to increase access to vaccinations for everyone who is eligible for the shot. The companies are also working on a version of their COVID-19 vaccine that does not need to be frozen at all but can be shipped and stored under refrigerated conditions. from https://ift.tt/3oC5KRE Check out https://takiaisfobia.blogspot.com/ On April 27, 2021, the U.S. Centers for Disease Control (CDC) eased its guidelines on wearing masks outside, saying fully vaccinated people did not need masks outdoors unless they were in a crowd of strangers. Public health experts largely supported the new guidance. SARS-CoV-2, the virus that causes COVID-19, is mostly transmitted through the air in the form of droplets or aerosols and fresh air disperses these. While outdoor transmission can occur, especially during contact-sports, studies suggest indoor transmission is around 19 times more common than outdoor transmission. The CDC was signaling where we ought to be focusing our efforts at preventative measures: indoor settings, especially poorly ventilated spaces with lots of unmasked, unvaccinated people. Yet, just 16 days later, on May 13, the CDC made a sudden about-turn. Without giving any warning, it abruptly changed its guidance on indoor masking, released mere days before the Occupational Safety and Health Administration (OSHA), the federal agency that oversees workplace safety, was to meet to review COVID-19 guidance for workplaces. CDC’s latest guidance seems to have given OSHA the ammunition it needed to ignore the science pointing to the risk of indoor aerosol transmission, as its website encourages employers to follow the CDC’s mask guidance. Employees in particular are now going to be in prolonged indoor contact with unmasked people, and in some areas of the country as many as 60% of people remain unvaccinated—and there’s no way to know for sure that all of those going maskless have, in fact, gotten their shots. When an indoor mask mandate was in place, employers were forced to protect their employees and customers. That protection has now gone. The CDC’s baffling, whiplash-inducing decision has caused immense frustration among those on the frontline working on U.S. pandemic control. In theory, the CDC’s new guidance was aimed only at those who are fully vaccinated, who are highly unlikely to catch or transmit the virus. While it makes scientific sense for vaccinated people to stop masking indoors, the guidance gave states the green light to drop indoor mask mandates for everyone. That’s the wrong approach at this stage. Maryland, Virginia, North Carolina, Ohio and Michigan immediately ended their indoor mask mandates in the wake of the new CDC guidance, as did major chain stores like Walmart, Trader Joe’s, and Costco. These states and companies are ceding their power to implement population- and business-wide policies that protect the health of all, and instead are just hoping for the best: that the unvaccinated will still wear masks indoors to protect themselves and others from illness, long COVID, and death. But hope is a weak public health strategy. The Biden Administration and the CDC have adopted a new rhetoric of personal responsibility that does not match the reality of the pandemic today. The government is abandoning its responsibility to keep the population healthy. It has eliminated guidance meant to protect the public’s health and placed the onus on individuals to protect themselves. Vaccination is being promoted as the only nationwide approach to prevent COVID-19. Instead of adopting a population-based strategy, in which we as a community would work together in solidarity to drive down transmission by universal masking indoors, Biden and the CDC are telling individuals that it is up to them to lower their risk. The CDC director now says “your health is in your hands” and President Biden says “The choice is yours.” It is hard to understand the CDC’s sudden, unexpected shift towards an individualized, vaccination-only stance. The implication is that vaccines are now available to all and its up to people to get them, but the reality of the U.S. vaccination efforts is that just one third of Americans are fully vaccinated. Coming only four weeks since eligibility for vaccination was extended to all aged 16 years and older, it makes one wonder if the CDC has forgotten that it takes two to six weeks (depending on which vaccine is used) for a person to become fully vaccinated. Read More: Anthony Fauci Is Finally Getting to Do His Job It is simply not the case that anyone who wants the vaccine can easily get their shots. For example, a recent survey by the Kaiser Family Foundation found that Latinx adults in the U.S. are around twice as likely as white adults to say they want to get vaccinated as soon as possible. Yet a high proportion of Latinx adults face an array of access barriers, including fear of jeopardizing their jobs by taking time off to get vaccinated, concerns they may be challenged over their immigration status, or worries that they will have to pay for the doses because they’re not sure if it’s free for everyone (it is) or not. Fewer resources have been targeted towards offering vaccination to the most vulnerable counties, those characterized by “high poverty rates, crowded housing and poor access to transportation, among other factors,” according to Amy Harmon and Josh Holder at the New York Times. As a result, there is a widening gap in the vaccination rate between the most and least vulnerable counties. What is particularly frustrating is that some states had established sensible roadmaps that tied the future easing of masking and social-distancing rules with specific indicators of progress in curbing the pandemic. And some of those have abandoned these careful plans given the new CDC advice. For example, North Carolina’s governor, Roy Cooper, and the state’s director of Health and Human Services, Mandy Cohen, had assured North Carolinians that the indoor mask mandate would remain in place until two thirds of residents had received at least one dose. But on May 14 Governor Cooper tore up this roadmap and ended the mandate (only 40% of people in the state have had at least one shot). In addition, there has been almost no time for the childhood vaccination campaign to get going. On May 12, the CDC’s Advisory Committee on Immunization Practices approved the use of the Pfizer-BioNTech COVID-19 vaccine in adolescents aged 12-15 years old. It is difficult to understand why just one day later the CDC changed its mask guidance. Given that most of the U.S. population still remains at risk, why was the CDC in such a rush to change its stance on masks? It is confusing and contradictory for the CDC to simultaneously acknowledge aerosol spread (which it belatedly and finally did on May 7) while also loosening protections against such spread. The new guidance is also confusing when it states that fully vaccinated people must still wear masks in homeless shelters, prisons, airports and bus stations. If the agency believes that fully vaccinated people are now safe around others indoors, why do they still need masks in these settings but not inside offices, workplaces, gyms, churches, stores or other indoor settings? The CDC clearly jumped the gun with its new guidance. It will leave vulnerable people—especially essential workers—unprotected and could increase their risk of infection. from https://ift.tt/3yjLloF Check out https://takiaisfobia.blogspot.com/ As conflict between Israel and the Palestinian militant group Hamas continues to claim lives in the Gaza Strip, health experts are calling attention to another potential crisis: a worsening COVID-19 outbreak in the area. The number of COVID-19 infections in Gaza was “just leveling off, and then this hit,” a United Nations official told the New York Times on May 16. “It is a grim situation.” On May 3, before the conflict began, Doctors Without Borders warned of an “extraordinary” rise in COVID-19 cases in Gaza, the strip of land between Israel and Egypt that is governed by the militant group Hamas and is home to about 2 million Palestinians. Mostly spared in the early months of the pandemic, the COVID-19 outbreak in Gaza worsened considerably in April, driven by spread of the more transmissible B.1.1.7 variant. Between March and April, new COVID-19 diagnoses in Gaza rose from less than 1,000 each week to more than 1,000 each day, according to Doctors Without Borders. It’s not clear how many people are being infected each day now. Violence between Israel and Hamas—which has so far killed more than 200 Palestinians and 12 Israelis, according to CBS News—has also all but shut down COVID-19 testing and care in Gaza, making it near-impossible to get an accurate picture of the outbreak.. “The number of positive cases is really underestimated. It doesn’t reflect the reality,” says Ely Sok, who leads Doctors Without Borders’ mission in the Palestinian territories of the West Bank, the Gaza Strip, and East Jerusalem. “We are expecting the number of severe cases requiring hospitalizations will increase.” Health services in Gaza were already lacking prior to the most recent violence. Even during times of relative peace, medical centers there are often “overstretched” and limited by frequent power outages, the UN says. Limitations on imports and movement across the border also frequently led to supply and medication shortages, and there are often not enough doctors to meet demand. In recent days, Israeli airstrikes have reportedly destroyed Hala Al Shwa Primary Healthcare Centre, which provided COVID-19 testing and vaccinations to Gaza residents; damaged the road leading to al-Shifa Hospital in Gaza City; and temporarily forced Gaza’s only laboratory for processing COVID-19 tests to close. Dr. Ayman Abu Elouf, who ran COVID-19 response at al-Shifa, was reportedly also killed in a bombing. All COVID-19 vaccinations have been halted in Gaza, according to the UN, and the nearly 60,000 Palestinians displaced by the conflict are in many cases huddling together in makeshift shelters that could become super-spreader sites. “It really harms the whole functioning of the medical system there,” says Hadas Ziv, head of projects and ethics at the nonprofit Physicians for Human Rights, based in Jaffa, Israel. “COVID-19 is somewhat pushed aside because there are wounded and dead. Limited capacity to deal with COVID is now non-existent, almost.” Now, due to the deadly combination of bombing injuries and COVID-19 cases, hospital beds are running out and doctors are scrambling to keep up. Electricity, water and sanitation systems are also damaged in many areas, further compromising care. Just across the border, Israelis are living in a different reality. More than 60% of Israel’s population has gotten at least one vaccine dose. COVID-19 cases have dropped low enough for the country to suspend outdoor mask mandates and resume many pre-pandemic activities. In Gaza, by contrast, only about 2% of people have received a dose. Gaza and the West Bank have received about 60,000 vaccines from the World Health Organization-backed COVAX facility and are still waiting on some 100,000 more, but additional shipments aren’t coming any time soon. Even if they did, Ziv says, there wouldn’t be adequate infrastructure to store and distribute them during the conflict. “Even if now they get the vaccines, it will be difficult to handle a big operation and keep them refrigerated,” she says. “It’s impossible to both deal with an armed conflict and the virus.” Security concerns, both for patients and providers, also make it near-impossible to offer all but the most critical care, Sok says. “You can do whatever you want, but if the patient cannot access it because of the shelling, it’s completely useless,” he says. “Only a cease-fire will solve the security issue.” from https://ift.tt/33TRVnZ Check out https://takiaisfobia.blogspot.com/ When Dr. Anthony Fauci arrived at 1600 Pennsylvania Ave. for his first White House press briefing under the new Biden Administration, he could see things would be different. It was the day after the Inauguration, and President Joe Biden was eager to get the country’s COVID-19 response back on track. Five minutes before he addressed the public, Fauci spoke with the new President. “He said, ‘I want you to just go and tell the science, explain to people that if we make mistakes, we’re going to fix the mistakes and we’re not going to dwell on the mistakes. Let science be communicated to the public.’” Not such a radical position, but it was a lifeline for Fauci, who had become renowned as a target of the ire of President Trump and his supporters—mostly just for being an unwavering advocate for science and the facts. Jen Psaki, the new White House press secretary, asked, “‘O.K., what do you want to talk about, and how long do you want to be up there?'” says Fauci. And that was it. “I said what I wanted to say. She didn’t check with the President or prompt me about what I was going to do. I just did it,” says Fauci. “It was a really good feeling, because it was really showing that science is going to rule.” That rule has produced results. Biden pledged to administer 100 million doses of COVID-19 vaccine in his first 100 days in office; an invigorated, combined federal and state effort achieved that goal in 58, leading to a new target of 200 million doses, which was also met a week ahead of schedule and led to the latest sprint to vaccinate 70% of American adults with at least one dose by the Fourth of July. Cases are still higher than they should be, at under 30,000 new infections a day on average, but are starting to come down as more people get vaccinated. Nearly two-thirds of Americans now approve of Biden’s handling of the pandemic, according to an ABC News-Ipsos poll. As the Biden team’s chief medical adviser, much of the credit goes to Fauci, director of the National Institute of Allergy and Infectious Diseases (NIAID)—Fauci’s advice has been a part of every COVID-19-related decision made by the Biden Administration, beginning even before Biden took office, when the then-President-elect asked Fauci about requiring masks on all federal properties for 100 days in an effort to hold back the surge of new infections last winter. Every day since, Fauci has been asked about everything from whether the second dose of vaccines can be safely delayed, as the U.K. decided to do in January, to whether vaccines are still providing enough protection against new variants. That wasn’t the case during most of Fauci’s tenure on the White House Coronavirus Task Force under Trump. “Having been on the playing field, as it were, during both administrations,” says Fauci, ”having the ear of [this] President is manifestly totally different than what it was before.” For scientists, truth is a given. It may come in different forms—as raw data churned out from a computer model, tables of statistics from a clinical trial of a new drug, or handwritten data scrawled in a lab notebook validating a new theory. But at their core, all scientific tools are rooted in objective and immutable facts. And throughout 2020, just when we needed it most, scientific truth was under fire as never before. Defending that truth fell on the slight but sturdy shoulders of a fast-talking career civil servant with an unmistakable Brooklyn accent. For Fauci, sharing science is an integral part of practicing it; he believes the power of science is tied to its accessibility. When he became the voice and symbol of scientific integrity in a world turned upside down by an invisible virus, Fauci conducted a master class in scientific diplomacy, and invited the world to watch. We witnessed his live demonstrations on how to stay true to the facts despite the disruptive and often vindictive interventions of a President refusing to acknowledge the gravity of COVID-19. “Tony Fauci is a remarkably effective spokesperson for the truth,” says his boss, Dr. Francis Collins, director of the National Institutes of Health. For those who know him, even if only by reputation, Fauci’s appointment to the White House Coronavirus Task Force at the end of January 2020 was a beacon of reassurance through what ultimately became a dark and disturbing year. The entire U.S. public-health system—including the Centers for Disease Control and Prevention (CDC) and the Food and Drug Administration (FDA), which normally lead the world in actions and advice on virus control—was largely sidelined as Trump systematically dismissed science in favor of political grandstanding. Week after week, Trump commandeered pandemic press briefings, downplayed the extent of the disease on social media, painted a rosier-than-reality picture of the U.S. response and mused on unproven and even dangerous “treatments,” from hydroxychloroquine to sunlight and bleach. Fauci took every opportunity he could find to provide a different voice, even as his own was turning raspier from the constant media appearances, press briefings and private meetings with Administration health officials to explain, educate and share what scientists knew and what they didn’t know about the viral threat. 
Through contradictions, confrontations and even personal insults from Trump, Fauci refused to engage, focusing instead on the facts. And even with a new President, the attacks on him have continued. Republican members of Congress like Senator Rand Paul and Representative Jim Jordan have accused Fauci of engaging in “theater” and of quashing civil liberties by supporting public-health measures like mask-wearing in public. When he can get a word in edgewise, Fauci sticks to his message that everything the government is recommending is scientifically justified, but it’s often a struggle. “You don’t really have a conversation with Senator Paul,” he says. “In one interchange, he was speaking at me, through me and under me and making statements mostly based on incomplete data or selected, cherry-picked data.” Where others might have stepped down, or at least considered it, Fauci never thought twice. “It’s kind of like General Patton during World War II saying, ‘I’m tired of this, I’m going to walk away.’ Your entire life you trained as a general to lead an army in a big war. It doesn’t matter what happens to you—you’re not going to walk away from it,” he said during one of several interviews conducted with TIME over the course of the past year. “You train as an infectious-disease person and you’re involved in public health like I am, if there is one challenge in your life you cannot walk away from, it is the most impactful pandemic in the last 102 years.” “People have asked me over the years—multiple times—‘Tony, what keeps you up at night? What’s your worst-case scenario?’” It’s nine months into the pandemic, and Fauci is sitting in a conference room in Building 31 on the National Institutes of Health (NIH) campus in Bethesda, Md., in front of the blue backdrop boasting the NIH-NIAID logos that has become a familiar site on his numerous virtual briefings and interviews. “We are living right now through my worst-case scenario.” Because of the pandemic, most of the staff at the NIAID, which Fauci has directed for 36 years, is working remotely. Fauci conducts almost all his briefings that way, which has the added benefit of allowing him to squeeze in more opportunities to communicate with other public-health experts and the public since he’s not traveling from in-person meeting to in-person meeting. Since January, he has represented the scientific community in press briefings on the pandemic response three times a week, along with Dr. Rochelle Walensky, the newly appointed CDC director; Andy Slavitt, the White House senior adviser on the COVID-19 response; and Jeff Zients, the White House coronavirus response coordinator. The regular briefings are Biden’s idea, Fauci says. In them, Fauci has (with the help of slides) clarified everything from why people couldn’t assume that if they were vaccinated they were immune from getting infected with the virus to breaking down why two doses of the vaccines are important to what impact variant strains are having on vaccine immunity. It’s all science, but that doesn’t mean it’s what everyone wants to hear. Fauci remains a target of frustration over what many feel are overly restrictive public-health measures such as social distancing, mask wearing and an unprecedented closure of businesses. And threats against his life and his family, which reached a peak last year, mean a rotating team of security guards continues to shadow him. “Unfortunately, the necessity still remains,” he says. “I still get threats.” What most draws the ire of detractors is not the evolving nature of scientific knowledge itself, but its consequence: changing advice to the public—which some interpret as uncertainty or even incompetence on the part of the public-health experts who impart it. The COVID-19 pandemic, Fauci says, “confirmed what I learned with other outbreaks, and that is that you really have to be humble and modest enough to know that you’re learning as you go along. What you see in January and February maybe triggers recommendations, guidelines and conclusions that all of a sudden, as you learn more and more, you realize that maybe you weren’t 100% correct. It’s the whole idea of the evolution of understanding.” He admits that health experts were wrong about two major things: the early assumption that only people with symptoms could spread the disease, and the belief that the virus couldn’t remain in the air long enough to float an appreciable distance. But they were willing to admit those mistakes and amend their advice based on what they learned. “One problem is that the American public thinks science is better than it is,” says Dr. Otis Brawley, former chief medical officer of the American Cancer Society and now professor of oncology and epidemiology at Johns Hopkins University. “They don’t realize it evolves over time. The only thing I wish Dr. Fauci had done—and he did say this, but maybe he didn’t say it loudly enough—was that we are early in this disease. We are going to learn. Some rules are going to change as we learn. If he had warned people of that more loudly, maybe he would have an easier time now.” As members of Congress accuse him of draconian and inconsistent responses to the pandemic, Fauci says he is not deterred. The “enormity of the problem, and the potential positive impact you can have by staying in the game” gives him the fortitude to weather the constant assaults meant to weaken his resolve, he says. Brawley, who like Fauci was educated in the Jesuit tradition, credits Fauci’s commitment to serving others to the sense of obligation they were taught. “Almost every individual in that position has to make a decision,” says Brawley. “At what point do I announce I can’t deal with this anymore and leave? There is the argument that one should stick with it and take the abuse because you are still having some influence and there may be big, big questions in the future where you really need to be there to make your voice heard. We were taught that sometimes you have to accept the hit to yourself for the greater good.” For Fauci, learning the necessity of self-sacrifice came during the early days of fighting another worldwide epidemic in the 1980s and 1990s: HIV. Then as now, he found himself at the bull’s-eye of vitriol and blame, at that time from activists in the AIDS community. He was the symbolic white coat of an indifferent government that wasn’t willing to address an epidemic that largely affected marginalized populations including gay men, IV drug users and sex workers. As director of NIAID, which oversaw testing of new AIDS drugs, Fauci was the natural scapegoat. “There was a very slow-moving research effort with nothing really to help people [with HIV],” says Mark Harrington, co-founder and executive director of Treatment Action Group (TAG), an AIDS advocacy organization, whose members, then known as ACT UP, organized an infamous “Storm the NIH” protest in 1990 during which he and other advocacy leaders were arrested. “Fauci was the one in charge, and nobody else was. There was nobody else we could have gone to.” The late Larry Kramer, the AIDS advocate notorious for his caustic style, wrote a commentary in 1988 in the San Francisco Examiner calling Fauci an “idiot” and a “murderer” for not being flexible enough to modify the way new drugs were tested so scientists could produce more tangible results sooner. “I thought, Whoa, if you wanted to gain my attention, you definitely gained my attention,” Fauci says of the screed. At the time, only people who participated in clinical trials could benefit from experimental drugs that were still unproven when it came to safety and effectiveness. ACT UP and other activist groups pushed Fauci to consider allowing people not in studies to access experimental drugs, as long as they understood and consented to the risks involved. “Several of the activists were saying, ‘Tony, take a deep breath and just think about it. What the hell is wrong with somebody taking a drug who can’t be on a clinical trial?’ I thought about it, and they were right,” says Fauci. The practice evolved into what is now known as “compassionate use.” Last year, that program gave thousands of severely ill COVID-19 patients access to the antiviral medication remdesivir before it was approved by the FDA in October, and possibly saved lives. The COVID-19 vaccine trials piggybacked off another HIV-era innovation that Fauci helped to orchestrate: the AIDS Clinical Trials Group (ACTG), a network of researchers and institutions that conduct studies of promising HIV drugs and is run by NIAID. Under Fauci’s direction, for the first time in NIAID history activists were invited to help design and recruit volunteers for the trials. Because of their connection to the HIV community, these advocates became an invaluable resource for the scientists trying to understand what to prioritize and how to effectively structure studies. The community-based programs established by the ACTG were critical in enrolling people in the COVID-19 vaccine trials from minority communities disproportionately affected by the disease and who would benefit most from an effective vaccine. Harrington recalls that even in the early days of the HIV epidemic, Fauci “was hearing and learning to understand what we were saying.” It’s a behavior Fauci has nurtured since his childhood in Brooklyn, where his father owned a pharmacy in Dyker Heights. On evenings and weekends, young Fauci would deliver neighbors’ prescriptions on his Schwinn. He rode the subway and bus into Manhattan to attend a Jesuit high school on the Upper East Side, where, he says, “the motto was service to others.” His studies there pulled him in two very different directions. “I wanted to understand society and history and how civilizations evolved,” he says. “I also became fascinated with science and by the fact that you could discover unknown things. And that you could solve problems in a way that is sound and irrevocable.” That led him to an unusual undergraduate degree at Holy Cross in premed and Greek classics—a nod to his growing interest in both the straightforwardness of science and the humanism of his Jesuit education. After graduating, Fauci went to medical school at Cornell, and as the country became more deeply involved in the Vietnam War, the newly minted M.D. chose to serve in the U.S. Public Health Service, to fulfill his military obligation. He was promptly assigned in the early 1970s to the National Institutes of Health and NIAID, where he would spend the rest of his scientific career. Fauci quickly became engrossed in the immune system, a bit of a scientific backwater and black box at the time. But there was something about infectious diseases and the way the body fought them that proved irresistible to him. “Infectious diseases had characteristics that fit with my fundamental personality profile—they’re acute, and they either kill you or you get better,” he says. “There is very little intermediate there. You can prevent them and you can treat them, and something about that was, bang, bang, bang, that I really liked.” All the while, Fauci continued to treat patients as a physician-scientist. When he saw the enormous cost the COVID-19 pandemic was having on doctors, nurses and first responders on the front lines, Fauci wasn’t just empathizing from afar. “Being somebody who has been in the trenches in the early years, taking care of very sick HIV-infected individuals, before we even knew what the virus was—I’ve been there,” he says. “So, when I see the health care providers today, doing their work without hesitation, that gives me a good feeling about who we are.” That sincerity hasn’t been lost on those on the COVID-19 front lines. As he left work late in the evening last Dec. 24—his 80th birthday—more than a dozen members of the Bethesda–Chevy Chase rescue squad and the National Institutes of Health fire department serenaded him with “Happy Birthday.” Fauci jumped in front of them for a socially distanced selfie. 
More than a year into the pandemic, Fauci remains energized by the challenge. When he talks about the first COVID-19 vaccine to enter human trials—in large part thanks to his early investment in the project—his passion is undeniable. “[It’s] a great example of how you can go from something that somebody is working on as a basic scientist for five or 10 years, and it ultimately gets to the point where it becomes translatable in a really important situation such as this pandemic,” he says. Fauci gives much of the credit for the speed at which the first COVID-19 vaccine moved into human testing to Dr. Barney Graham, deputy director of NIAID’s Vaccine Research Center, which was originally created as a joint program between NIAID, the National Cancer Institute and the NIH Office of AIDS Research, but is now under Fauci’s direction at the NIAID. Since 2013, Graham had been working out the genetic formula for generating just the right configuration needed for a potent respiratory syncytial virus (RSV) vaccine. He was still at it when the novel coronavirus dubbed SARS-CoV-2 pounced on the world. In December 2019, as more cases of the mysterious pneumonia in Wuhan, China, started to pile up, Fauci recalls, Graham was confident he could apply what he’d learned to create a vaccine against the new coronavirus. “Barney said, ‘Get me the damn sequence, that’s all I need,’” Fauci says. On Jan. 10, that sequence materialized on an open genetic database. “It took Barney about 50 seconds to … pull out the spike protein” and figure out the sequence coding for the correct formation of the protein that would become the target for five of the six COVID-19 vaccines that the U.S. government helped to develop or, in Pfizer-BioNTech’s case, purchased early on. (Today, three of those have received FDA authorization.) But at that point, it was up to Fauci to decide if the world even needed a COVID-19 vaccine. “We’re talking about January, and nobody is excited about this,” he says. The first U.S. case had not yet been reported, and there was still a naive sense among the Trump Administration that maybe the virus would simply go away after burning out overseas. Fauci’s experience with HIV, however, had taught him prudence, since that epidemic too began with a handful of cases that ballooned into millions. It was likely, he knew, that the early reports that SARS-CoV-2 couldn’t spread easily from person to person were “nonsense,” he says. He gave Graham the green light, and a million dollars, to start building the vaccine. He reasoned it was worth a try since SARS-CoV-2 was the third coronavirus to plague the world, and previous efforts to develop shots against one of them, MERS, were shut down when cases dwindled. A successful COVID-19 vaccine wouldn’t just pay off now; it could be useful as a foundation for fighting any other coronavirus that might emerge down the road. Plus, this time, Fauci was excited about a new technology that relied on the genetic material called mRNA, which was being used by one of NIAID’s partners, Moderna, a biotech company in Massachusetts. The mRNA technology shaved months off the typical vaccine-development timeline. About three months after the genetic sequence of SARS-CoV-2 was published, Pfizer and BioNTech scientists submitted a request to the FDA for emergency-use authorization of their mRNA-based vaccine, after studies showed it was 95% efficacious in protecting people from COVID-19 disease. Fauci received the news directly from Pfizer CEO Albert Bourla on Nov. 8 as he was enjoying a Sunday beer and a socially distant chat with a neighbor in the backyard. “He said, ‘Tony, are you sitting down? You are not going to believe the results; they’re unbelievable,’” says Fauci, who also wasn’t expecting nearly such a success. A week later, Moderna reported similar results, and the two vaccines became the first to receive emergency-use authorization in the U.S. They remain the bedrock of the country’s vaccination program. “This [mRNA] technology will revolutionize vaccinology,” says Fauci. “The HIV people are really interested in it now.” In many ways, Fauci’s 2021 is radically different from his 2020. In others it’s exactly the same. Aside from the three weekly press briefings he attends, Fauci also fields four or five calls a day from Jeff Zients, who conveys questions from the President or seeks advice on policies the Administration is considering. Looking toward the next year, Fauci says we shouldn’t be so focused on the specific number of people who need to be vaccinated to reach herd immunity. Instead, he says, we should keep concentrating on vaccinating as many people as quickly as possible. On that front, after a surge of people rolling up their sleeves over the winter and early spring, the U.S. may now be hitting a wall of vaccine hesitancy. “It’s a difficult question, and I don’t think there is an easy answer,” he says about ways to reach people who aren’t eager to get vaccinated. “We just have to keep trying to get the message out based on the evidence and the data. We can’t give up.” Fauci won’t feel comfortable saying we’re near the beginning of the end of the pandemic until new infections start to come down “somewhere south of 10,000 a day” from the current 33,000 infections a day on average. But unlike last year, he now sees a path toward that goal because of vaccinations. He hasn’t forgotten the terrible toll that COVID-19 has taken on American families, often reminding people that as rosy as things may look now with the vaccines that are available, COVID-19 has claimed more than 585,000 lives in the U.S. alone. The worsening situation in India is another stark reminder of the danger of becoming complacent. When I ask whether he thinks we’ll be able to put COVID-19 behind us, or whether it will look more like a flu that comes back in slightly different forms each year, he responds with typical frankness. “I’d love to give you a confident answer to that. But I have to be totally honest—I don’t know,” he says. “Even if we get the infection rate very, very low in our country, with the overwhelming majority of people vaccinated, there will always be the threat of new variants coming in because there will be active virus in other parts of the world. I think at least in the next couple years we are going to have to be really careful about the virus returning.” That could mean annual booster shots of the vaccine, which both Pfizer-BioNTech and Moderna are already studying. It also means Fauci will continue to be busy. He’s still not getting much sleep these days, but he still doesn’t mind. “The aggravation and stress of being at odds with the [Trump] Administration—that’s stressful.” Under Biden, he says, “I’m putting in more hours and working harder, quite frankly, but it’s in the realm of not being attacked and in the realm of being supported, which makes a big difference.” His role as the country’s chief medical adviser will ensure that his legacy will be felt long after this pandemic fades away. The communication skills that have made him an effective translator of science for the lay public is already lighting sparks of inspiration in the next generation of potential physicians and scientists. In the past year, applications to medical schools have jumped, in some cases by as much as 18% over the previous year—no doubt in part because lockdowns are finally giving people the time to consider and complete the involved applications, and in part because of the selfless example of frontline medicine throughout the pandemic. But also, as admissions officers are learning from students who cite Fauci as a role model, because of the so-called Fauci effect. That comes as no surprise to Dr. Luke Messac, an emergency-medicine resident at Brown University who cares for COVID-19 patients. When he was a junior at Harvard, Messac emailed Fauci on the off chance the NIAID director would answer a few questions about his role in orchestrating the President’s Emergency Plan for AIDS Relief, one of the most robust and productive HIV-treatment programs in the world. Not only did Fauci respond, but he invited Messac to his office in Bethesda, where they spent over an hour discussing the topic. When Messac sent Fauci the finished paper, Fauci responded with a glowing review and asked if he could cite some of the conclusions in his future talks. In July 2020, Messac shared his experience, and Fauci’s response, on Twitter and was overwhelmed by the positive reaction. “I thought it might help people to better understand who he was behind the spotlight when people weren’t looking,” Messac says. For Fauci, the idea that a new generation of young people may benefit from careers in science or public health as much as he did is the silver lining of the past year, worth the personal insults and the loss of privacy. “If I’m doing anything to get young people to seriously consider the field of medicine, then I feel really good about that,” he says. “The idea that some young man or woman may decide to go into medicine because they see what I’m doing, that pleases me as much as anything else.”
from https://ift.tt/33PL7I2 Check out https://takiaisfobia.blogspot.com/ WASHINGTON — President Joe Biden said Monday that the U.S. will share an additional 20 million doses of COVID-19 vaccines with the world in the coming six weeks as domestic demand for shots drops and global disparities in distribution have grown more evident. The doses will come from existing production of Pfizer, Moderna or Johnson & Johnson vaccine stocks, marking the first time that U.S.-controlled doses of vaccines authorized for use in the country will be shared overseas. It will boost the global vaccine sharing commitment from the U.S. to 80 million. “We know America will never be fully safe until the pandemic that’s raging globally is under control,” Biden said at the White House. The announcement comes on top of the Biden’s administration’s prior commitment to share about 60 million doses of the AstraZeneca vaccine, which is not yet authorized for use in the U.S., by the end of June. The AstraZeneca doses will be available to ship once they clear a safety review by the Food and Drug Administration. Biden also tapped COVID-19 coordinator Jeff Zients to lead the administration’s efforts to share doses with the world. “Our nation’s going to be the arsenal of vaccines for the rest of the world,” Biden said. He added that, compared to other countries like Russia and China that have sought to leverage their domestically produced doses, “we will not use our vaccines to secure favors from other countries.” The Biden administration hasn’t yet said how the new commitment of vaccines will be shared or which countries will receive them. To date, the U.S. has shared about 4.5 million doses of AstraZeneca vaccine with Canada and Mexico. Additional doses of the Pfizer vaccine manufactured in the U.S. have begun to be exported as the company has met its initial contract commitments to the federal government. The U.S. has faced growing pressure to share more of its vaccine stockpile with the world as interest in vaccines has waned domestically. “While wealthy countries continue ramping up vaccinations, less than 1 percent of COVID-19 vaccine doses globally have been administered to people in low-income countries,” said Tom Hart the acting CEO of the ONE Campaign. “The sooner the US and other wealthy countries develop a coordinated strategy for sharing vaccine doses with the world’s most vulnerable, the faster we will end the global pandemic for all.” More than 157 million Americans have received at least one dose of a COVID-19 vaccine, and 123 million are full vaccinated against the virus. Biden hopes the U.S. will have 160 million people fully vaccinated by July Fourth. Globally, more than 3.3 million people are confirmed to have died from the coronavirus. The U.S. has seen the largest confirmed loss of life from COVID-19, at more than 586,000 people. from https://ift.tt/3fonT0P Check out https://takiaisfobia.blogspot.com/
My dad, who was always intuitive, told us he saw that my little sister’s depression had returned when he printed photographs he’d taken of her. “I could see it in her eyes, like a ghost,” he said. It was an observation born of love and experience, not science, but not wrong. Until recently, major depression has felt like a ghost disease–invisible but devastating. It’s a disorder that still affects millions every year–one in four of us will suffer a depressive episode in their lifetime. Despite those numbers and the fact that humans have been documenting and speculating about it for millennia, we’re only beginning to understand its biology. How differently would we think about depression if we could visualize it, track it and fight it the way we do cancer or the novel coronavirus? Thanks to some astounding new research, we’re getting closer to finding out. In April, a team at the Indiana University School of Medicine published news about a promising new blood test that can reveal how severe a patient’s depression may be, the risk of developing severe depression, and even the risk of future bipolar disorder. This breakthrough using RNA biomarkers will get us closer to more precise and effective treatments and is just one example of a whole slew of biomarkers for depression that researchers have been uncovering. Sign up for It’s Not Just You here to get an essay every Sunday. Other findings that further establish the link between the biology of the brain and mood disorders may lead to new drug therapies. Earlier this year, researchers in the Department of Psychiatry at McGill University, Montreal, produced evidence that a reduced density of star-shaped brain cells called astrocytes is linked to major depression. These wondrous star cells support neurons, and a single astrocyte cell can interact with up to 2 million synapses at a time. A reduction in astrocytes in the brain regions studied may have adverse effects because those areas are thought to be important for decision-making and emotional regulation, conditions common in major depression. So there may be an opportunity to alleviate depression by developing drugs that boost the astrocytes or their functions. (And there’s optimistic related research on psychedelics like ketamine which may affect astrocyte function.) Surely it’s possible to define the contours and mechanisms of depression in ways that allow us to see what we’re fighting clearly, and to shed the old stigmas, myths, and self-blame that have clung to this disease for too long. After all, in just a year, we had a picture of the coronavirus in our heads with its red spikes; we could get a test for it, and in record time, we had a vaccine. Imagine if we thought of depression, anxiety, and other mood disorders as a pandemic-level crisis and launched a response proportional to the toll these illnesses take, especially in the wake of the pandemic. (And crisis is not too strong a word: the CDC reported the percentage of U.S. adults with recent symptoms of anxiety or a depressive disorder rose to 41.5% in February. The toll in lost productivity, related increases in substance abuse, and heartbreak is immeasurable. The World Health Organization reports that depression is the leading contributor to long-term disability globally) This effort could include an ‘operation warp speed‘ type-accelerator for all this promising biomarker research, plus an infusion of resources to provide universal access to therapists and existing treatments right now. Given that all of us know someone or are someone who’s battled this disease, it’s everyone’s issue. The mental health moonshot we need would provide hope and that in and of itself might save lives. The process of finding effective remedies for depression can be so debilitating that just the thought of going through that cycle of trial and error again is unbearable for some patients, like my sister. (Only about a third of those diagnosed with depression get treatment at all. And a third of those who do get help find their depression doesn’t respond to treatment.) William Styron, whose searing descriptions of depression defined it for generations, wrote about how believing there’s no remedy is what makes the disease intolerable: “It is hopelessness even more than pain that crushes the soul.” I hang on to hope by thinking about the researchers who may someday be able to illuminate the darkest places of the mind by replenishing lost star cells. There’s a universe within us, one we need to explore. And research like the discovery of the link between astrocytes and depression is both a wonder of science and a demonstration of a kind of human magic — faith in the power of knowledge to heal. Did someone forward you this newsletter? Sign up for It’s Not Just You here to get an essay every Sunday. And send comments to me at: [email protected] 
RESOURCES AND INITIATIVESFor Mental Health Awareness Month, the Child Mind Institute launched Getting Better Together – a campaign featuring inspiring, homemade videos from celebrities including Zoe Saldana, sharing their personal stories to support kids who are especially struggling during the pandemic and lend a powerful voice to help eliminate stigma, inspire hope, and encourage kids to ask for help. View the videos on their social channels: Twitter: @ChildMindInst; Instagram: @childmindinstitute; Facebook: facebook.com/ChildMindInstitute

In the wake of COVID-19, millions of people have uncovered new mental health conditions and millions more have had their existing challenges exacerbated. In response to this crisis, more than 500 organizations are teaming up to launch the inaugural ‘Mental Health Action Day’ on May 20. Learn about resources are available to individuals and what you can do to make mental health care a national priority at: www.MentalHealthActionDay.org COPING KITNational Alliance on Mental Illness (NAMI) NAMI Connection is a support group for people with mental health conditions. Groups meet weekly, every other week or monthly, depending on location. This program is also available in Spanish, NAMI Conexión. Find the NAMI Connection support group nearest you NAMI Family Support Group is a support group for family members, significant others and friends of people with mental health conditions. Groups meet weekly, every other week or monthly, depending on location. Find the NAMI Family Support Group nearest you The NAMI HelpLine can be reached Monday through Friday, 10 a.m.–8 p.m., ET. 1-800-950-NAMI (6264) or [email protected] Text HOME to 741741 to connect with a Crisis Counselor Free 24/7 support at your fingertips US and Canada: text 741741 UK: text 85258 | Ireland: text 50808 Talk to someone now: National Suicide Prevention Lifeline 1-800-273-8255 CHAT WITH LIFELINE Options For Deaf + Hard of Hearing For TTY Users: Use your preferred relay service or dial 711 then 1-800-273-8255. Share this edition of It’s Not Just You here. Did someone forward you this newsletter? SUBSCRIBE to It’s Not Just You here. from https://ift.tt/3ykqXE7 Check out https://takiaisfobia.blogspot.com/ On June 7, North Carolina attorney general Josh Stein will enter a Durham courtroom with a mission: proving that the e-cigarette company Juul Labs purposely targeted teenagers with its nicotine-rich products. If Stein—who in 2019 became the first state attorney general in the U.S. to sue Juul—is successful, the vaping company may be in for a world of hurt. Hundreds of lawsuits against Juul, many of which were consolidated into multi-district litigation in California, are pushing allegations mirroring Stein’s. They claim Juul purposely designed its stylish, flash-drive-like devices and flavored nicotine e-liquids to appeal to teenagers. The product launched with a flashy marketing campaign that, the complaints argue, was likewise meant to appeal to young people. The suits allege Juul planted the seeds for a youth addiction epidemic that would make nicotine cool again after years of historic declines in cigarette smoking. Juul’s executives have repeatedly denied that they meant to attract children; they say their goal has always been to give adult smokers a better option than deadly combustible cigarettes. To their credit, most health experts agree that e-cigarettes—while not full-stop safe—are less dangerous than cigarettes. And Juul, with a sleek design and satisfying nicotine delivery, could be particularly appealing to adult smokers looking to switch. Whether Juul meant to attract them or not, though, millions of teenagers have used its products. In 2020, about 20% of high school students and 5% of middle-school students said they had vaped some sort of e-cigarette in the past month. Those figures are down from 27.5% and 10.5%, respectively, in 2019—rates high enough to prompt sweeping regulations on e-cigarettes. In late 2019, the Trump Administration raised the legal tobacco purchase age to 21. Days later, the U.S. Food and Drug Administration (FDA) banned many flavored vaping products that could appeal to teenagers. The FDA, which recently announced an impending ban on menthol-flavored combustible cigarettes and flavored cigars, is currently deciding whether to continue allowing the sale of e-cigarette products in the U.S.—and for teen favorites like Juul, data around youth vaping could be the nail in the coffin. How could things have gone so wrong for a company founded by two Stanford students who said they wanted to make cigarettes obsolete? The fall from grace began in June 2015, when Juul was just a promising innovation from a startup called Pax Labs. Juul’s launch, almost six years to the day before the company will stand trial in a North Carolina courtroom, marked both its beginning and the beginning of its end. 
Juul vaporizers were everywhere. Stacks of the slim devices littered every surface, lying there free for the taking—which people were doing happily, grabbing them and exhaling plumes of sweet-smelling vapor. Juul’s June 2015 launch party was held at Jack Studios, a giant industrial loft space in Manhattan often used for fashion photo shoots, with striking views of the city skyline and the Hudson River below. Guests could pose for photos in front of a multicolored triangle pattern, drawn from Juul’s first ad campaign, Vaporized. The Vaporized campaign was fun and colorful, full of fresh-faced models dressed in trendy clothes flirting with the camera and posing against colorful backdrops. Drinks were flowing from the open bar, and every guest left with plenty of Juul swag. The events team hired buzzy DJs Phantogram and May Kwok, and Top Chef winner Ilan Hall handled catering. Marley Kate, the photographer who’d shot the Vaporized campaign, took photos of guests, which were then projected onto the loft’s walls as live art. The best shots had a chance at appearing on the company’s Times Square billboard. The goal was for cool New York City socialites to be seen pulling on Juul vaporizers. The company had specifically chosen to launch Juul in New York City and Los Angeles, two trendsetting cities full of influencers and journalists who, according to a company marketing document released in 2019 by a congressional subcommittee, could help build buzz. Pax—the parent company that made and marketed Juul products—had spent much of its marketing budget on advertisements that appeared in convenience stores and other retail spaces, as well as on the Times Square billboard and in a print ad that appeared in Vice, which called itself part of the “#1 youth media company in the world.” But social media marketing was valuable to the scrappy startup too, in no small part because it was cheap. If influencers were seen using the Juul, their followers would want to try it. And once their followers tried it, they would post about it and tell their friends. But this social media marketing strategy, unlike most utilized by startups, hinged on promoting an age-restricted and highly addictive nicotine product on platforms beloved by teenagers. To get the word of mouth flowing, Pax hired Grit Creative Group, a marketing agency that called itself “an authority on millennial culture,” to secure influencer guests for the Juul launch party. In addition, a network of nearly 300 New York and Los Angeles influencers would be gifted free Juul products over the coming weeks. On the list were movie star Leonardo DiCaprio (who had already been photographed vaping other e-cigarettes), and model Bella Hadid. At the time Juul launched, in June 2015, Hadid had almost a million Instagram followers—and, at 19, was only barely able to legally purchase an e-cigarette in most states. Giving launch-party guests the chance to pose for a professional photographer, and potentially appear on a Times Square billboard, was a brilliant viral marketing move. After the party, social media were awash in photos of young, attractive people holding drinks and puffing on Juuls, their photos hashtagged #Vaporized and #LightsCameraVapor. Juul’s official accounts posted some photos too. “Having way too much fun at the #JUUL launch party,” read one tweet from Juul’s handle, right above a photo of five fashionably dressed young women pouting for the camera. “The party was a resounding success (at least in my mind) in terms of winning over the cool kids,” one employee wrote afterward in an email to chief operating officer Scott Dunlap; the email was later included in the multi-district litigation against Juul, initial trials for which are set to begin next year. Juul didn’t stop at one great party. After that night at Jack Studios, it set off on a six-month “sampling tour” concentrated in urban areas. Juul-branded shipping containers popped up at concerts, clubs and rooftop bars, beckoning people inside with bright colors and the promise of free products. The cargo containers featured a lounge area; an “animated GIF booth” where people could pose for the camera; and a “flavor bar” where guests could try tobacco, mint, fruit or crème brûlée Juul pods. People liked what they saw. “@juulvapor is the best, most satisfying #ecig I’ve ever tried. Great product! Only $50 too!” one customer tweeted a few days after the product launched. “Juul has won me over in just a week,” a blogger wrote on the site Engadget, marveling that after he’d smoked for 14 years, Juul had helped him dramatically cut down on cigarettes. Even the mainstream press was noticing. A Wired profile proclaimed Juul possibly “the first great e-cig.” But some of the social media posts coming in after sampling events made certain executives uneasy. “I would catch myself saying, ‘Wow, they look really young,’” former COO Dunlap told the New York Times. “But you don’t really know. It’s social media after all, where everyone is their younger, idealized selves.” Shortly after the product launched, Ad Age published an article in which a spokesperson from the Campaign for Tobacco-Free Kids voiced concerns about Juul’s marketing appealing to kids. “We’re seeing more and more irresponsible marketing of unregulated products such as e-cigarettes,” the spokesperson said. “We are concerned any time a new product or new advertising campaign goes public regarding cigarettes and tobacco and their addictive nicotine.” The story was a wake-up call. “We were like, ‘Oh my God, that’s terrible,’” says a source involved in the launch campaign, who wished to remain anonymous because they were not authorized to speak about their time at the company. Company executives insist they didn’t want their products to appeal to kids, or even to be perceived as appealing to kids. The Vaporized campaign had been in the world for only a short time, but already Pax executives were realizing it could sink the company before it swam. In July 2015, just a month after Juul officially launched, Pax investor Alexander Asseily began to get very vocal about his concerns, according to documents included in a legal complaint filed by the Hawaii attorney general in 2020 and currently moving through pretrial hearings. If the company kept marketing in ways that could be seen as targeting kids, Pax was going to get lumped in with Big Tobacco, an industry infamous for preying on young people with its marketing. “We will continue to have plenty of agitation if we don’t come to terms with the fact that these substances are almost irretrievably connected to the sh-ttiest companies and practices in the history of business,” Asseily wrote in an email to board members included in the Hawaii legal complaint. “It’s not about faking it—it’s about doing it correctly … which could mean not doing a lot of things we thought we would do like putting young people in our poster ads or drafting in the wake of big players in the market.” Shortly after, Asseily began brainstorming with chief marketing officer Richard Mumby about what the company could do differently. They kicked around ideas like a program through which smokers could turn in their cigarette packs or subpar vaping products in exchange for discounts on Juul products. It would “send the only message that’s needed,” Asseily wrote in an email to members of the leadership team included in the multidistrict litigation complaint. “Juul is a superior alternative to conventional smoking and mediocre vaping products.” That idea never got off the ground, but it was clear something had to change. Mumby began working on a replacement for the campaign he had only just launched, one that people within the company hoped would have no appeal to—or even the perception of an appeal to—kids. The new concept would have a more muted color scheme and focus on shots of the product itself rather than on models. Some of the Vaporized ads were pulled immediately, even before the new spots were ready. While this was happening, however, the Juul brand was beginning to spread, slowly but surely, on social media and online. If parents had known what Juul was back then, they probably would have been appalled. But the device was so new, and looked so much like a flash drive, that they might not have known that what their children were actually seeing as they scrolled through social feeds on their phones was an addictive e-cigarette. And even if they did know what Juul was, they almost certainly wouldn’t have known how much nicotine it contained. That ingredient was disclosed only at the very bottom of the ad, in tiny print. Besides, the eye was drawn to other words. JUUL, the ads read in huge block letters. VAPORIZED. 
Matthew Myers, president of the Campaign for Tobacco-Free Kids, watched uneasily as this unfolded. When he saw Juul’s ads, all he could think of were old cigarette ads. They ticked the same boxes: young, fun models selling sex, sophistication and a good time. “As somebody who’s worked in this field and looked at cigarette industry behavior too long,” Myers says, “the instant reaction is: Juul is replicating the 1950s and 1960s playbook from the cigarette companies.” Pax executives may have said Juul was for adult smokers only, but to Myers, their actions didn’t match their words. Juul’s Vaporized campaign came out amid a spirited debate in the public-health world. In 2015, the World Health Organization commissioned a report that warned e-cigarettes might damage the lungs and expose users to carcinogens. The same year, Public Health England, an agency sponsored by England’s Department of Health and Social Care, declared in a highly publicized report that thanks to their lower levels of carcinogens and harmful chemicals, e-cigarettes were 95% safer than combustible cigarettes. It was difficult figuring out what to believe, but the anti-vaping crowd had at least one leg up: it could always bring the conversation back to Big Tobacco, especially as Pax and other companies made dubious marketing decisions like Vaporized. Many people, like Myers, saw history repeating itself in Juul’s Vaporized campaign. Big Tobacco had lied to the public and targeted teenagers for decades; if it looked like vaping companies were following in their footsteps, e-cigarettes suddenly came out looking a bit more sinister. No matter how deeply scientists believed in tobacco-harm reduction, there was little they could do to defend themselves when e-cigarette brands were lumped in with Big Tobacco. “When we push back against [anti-e-cigarette rhetoric], we sound like we’re defending the tobacco industry,” laments Raymond Niaura, a tobacco dependence and treatment expert at New York University who supports the use of e-cigarettes. Pax executives should have known about these dynamics and designed a launch campaign that had no possible link to Big Tobacco. But the promise of future growth seemed to trump historical caution. “They had the Silicon Valley mindset of ‘We’re a tech company; we’re not a tobacco company,’” says Gregory Conley, president of the American Vaping Association. “And so, they hired very, very few people with experience in tobacco” early on. If they had, Conley says, they might have had on staff people able to see where things were going, who would have never let a campaign with even a chance of drawing comparisons to Big Tobacco end up on a billboard in Times Square. Instead, the comparisons to cigarette ads and the allegations of targeting teenagers clouded Juul’s reputation right from the very beginning—even more so as teen vaping rates soared and Juul gobbled up market share. To this day, health experts and anti-vaping advocates often point to Juul’s ill-fated Vaporized campaign as evidence that it purposely hooked teenagers and engineered a brand-new addiction. For years, that allegation mostly amounted to bad press. Now, though, Juul may be in for its most serious threats yet. The outcome of Stein’s lawsuit in North Carolina could set a precedent for the hundreds of other pending cases against Juul, filed by school districts, individuals and attorneys general from states including Massachusetts, California, Colorado, Hawaii and Minnesota. Beyond that, the outcome in North Carolina could color the FDA’s impending decision on e-cigarette products like Juul. After years of allowing e-cigarettes to be sold without formal FDA approval, the agency is now sifting through applications from hundreds of companies trying to prove their products can help protect public health, the benchmark they must meet to stay on the U.S. market. Vaping products’ popularity among teenagers is likely to be a strike against many manufacturers—so if a state attorney general can prove that Juul purposely lured underage customers, the aggressive regulators of the Biden Administration’s FDA could find that too large a red flag to ignore. E-cigarette makers like Juul may be next on the FDA’s chopping block, particularly if the company’s past comes back to haunt it. Juul’s supporters argue too much attention has been paid to a single advertising campaign that ran for only a few months and, the company contends, made little impact on Juul’s sales. But as the saying goes, you don’t get a second chance at a first impression. If Juul had a target on its back in the years that have followed, it was only because it put one there with its early, unforced error. And now, lawyers like North Carolina’s Stein are shooting for a bull’s-eye. Adapted from Ducharme’s book, Big Vape: The Incendiary Rise of Juul, out May 25 from https://ift.tt/3eRsppC Check out https://takiaisfobia.blogspot.com/ In news everyone has been waiting for since last year, the U.S. Centers for Disease Control and Prevention (CDC) said May 13 that people who are fully vaccinated against COVID-19 can ditch their masks, both indoors and outdoors, and stop social distancing as well. It was welcome news, especially as politicians and many in the public have been criticizing the CDC for moving too slowly to update its guidelines as more people in the U.S.--over 35% as of today—have received a full course of vaccinations. In addition, while initial research only showed that vaccination prevented COVID-19 disease, recent data suggest that vaccinated people are also protected from getting infected with SARS-CoV-2—the virus that causes COVID-19—and are therefore also far less likely to spread it. In a press briefing, CDC Director Dr. Rochelle Walensky cited the vaccination effort, the real-world data showing the shots are working, the dropping case counts in the U.S., and scientific evidence that the vaccines protect against worrisome variants that have emerged around the world as reasons for the updating the agency’s mask advice. “If you are fully vaccinated, you can start doing things you stopped doing because of the pandemic,” she said. “We have all longed for this moment when we can get back to some sense of normalcy. Based on the continuing downward trajectory of cases, the scientific data on the performance of our vaccines and the understanding of how the virus spreads, that moment has come for those who are fully vaccinated.” There are still inconsistencies in the CDC guidance, however, that may cause confusion over coming days and weeks. For example, the CDC still requires passengers on planes, buses and trains to wear masks, regardless of their vaccination status. Walensky acknowledged the disconnect in the agency’s advice, saying “we are going to be looking at all of our guidance and updating all of our guidance—including travel—shortly, now that we have this new guidance out there.” Walensky denied that the update was meant to incentivize more people to get vaccinated, given that rates have slowed in recent weeks. Instead, she said, it was based on “the science.” “Several things happened in the last two weeks,” she added. “Cases have dropped by a third, and in the last two weeks, there is increasingly available vaccine, which is now available for people 12 to 15 years. And we have had the coalescence of more science that emerged and improved [our understanding] for three reasons—one, on the effectiveness of the vaccines, two, on the effectiveness of the vaccines against the variants, and three, the effectiveness of the vaccine in preventing transmissibility.” Dr. Anthony Fauci, President Joe Biden’s chief medical advisor, noted at the briefing that if people who are fully vaccinated still feel more comfortable wearing masks in public settings, they should continue to do so. “People have to make their own personal choice,” he said. “What Dr. Walensky described was the [new] recommendation that is based on science, and it’s just a recommendation. There is absolutely nothing wrong with the individual who has a certain level of risk aversion and doesn’t want to take even the very low risk of infection if they are vaccinated, and still wear a mask indoors or outdoors. There is nothing wrong with that, and they shouldn’t be criticized.” from https://ift.tt/2SSxztb Check out https://takiaisfobia.blogspot.com/ |
Authorhttps://takiaisfobia.blogspot.com/ Archives
April 2023
Categories |
 A version of this article also appeared in the
A version of this article also appeared in the RSS Feed
RSS Feed
