|
Holding an Olympics during a pandemic was never going to be easy, and the Tokyo Organizing Committee consulted with numerous public health experts and invested in tracking app systems to help curb the spread of the virus within the Olympic community. But despite these strict countermeasures, an imperfect system and practical issues in compelling thousands of people from around to world to comply with often intense and inconvenient protocols are already leading to lapses that are opening the door for SARS-CoV-2, and in particular its Delta variants, to spark new infections that could quickly flare up into clusters of cases. For example, while the media in Tokyo are under strict testing, contract tracing and bubble measures, and are required to wear masks, there are situations that are providing potential fertile ground for the virus to spread. For the first 14 days after Olympic visitors, including athletes and journalists, arrive Tokyo, they are not allowed to take public transportation or walk in the city. But they are assigned to hotels in the city, at which non-Olympic guests are also staying. That means their rooms may be cleaned and they may be served in restaurants by Tokyo residents, who, given the low vaccination rate so far, are more than likely not immunized against COVID-19. Athletes and media are also asked to take Olympic-only transport, which consists of buses or designated taxis that can be reserved and have been (supposedly) cleaned and cleared. Yet again, given Tokyo’s low vaccination rate, the drivers of these buses aren’t likely to be vaccinated, and return home to their families after their shifts. And in the case of Olympic buses, during those shifts, they are driving consistently packed, standing-room only, cheek to jowl rides during which it’s impossible to impose the social distancing that’s ideally required to contain COVID-19. The Tokyo Organizing Committee did not immediately return a request for comment. 
Read more: This is What Happens When an Athlete Tests Positive for COVID-19 “Even when people are wearing a mask, they have above their head and around them a growing cloud of respiratory droplets,” says David Edwards, faculty member of Harvard University in bioengineering. “People inhale 1 million to 100 million droplets a day, with 80% of those droplets being too small to settle by gravity. A bus is the classical super spread situation where you don’t get great circulation because the windows are not open.” Edwards is founder of FEND, a company that makes a nasal hygiene device that provides a mist for cleansing the upper airways to prevent disease-causing viruses from reaching deeper lung passages. Indoor rooms are no better, says Edwards. “When 10, 20, or 30 people are breathing in a room, the cloud grows and grows. You may be wearing a mask, but that’s going to stop droplets from being inhaled into your lungs.” What about a room with not 10, 20 or 30 people but 100, 200 or 300 people in the Main Press Center workroom, or any of the press rooms at venues, sitting less than six feet apart for hours at a time, with only plexiglass barriers between them? “Barriers are a way to add that much more distance for the droplet to travel. But there are clouds on both sides of the barrier. Barriers lower the probability of the person sitting next to you breathing out a droplet, and it lowers the probability getting in you, but it doesn’t stop the cloud effect,” says Edwards. 
Same goes for the security measures at each of the venues and the main press and broadcasting centers, which require media and athletes to take off their masks and have their picture snapped at the same time that their credential, hung around their neck, is scanned by a standing kiosk machine. Because most journalists aren’t bothering to remove their credential, that means that the space in front of the camera becomes another cloud of happy respiratory droplets containing all manner of bacteria or viruses that are floating around ready to get pulled into the lungs of a new host with the next inhalation. Athletes entering the Main Press Center for press conferences are subject to the same procedures, even if they’re being asked to hang their own medals around their necks for fear of coming into close contact with medal presenters. The only reassuring news comes from the fact that getting infected that way is a matter of both distance and time, says Edwards. The shorter time spent in the vicinity of such a cloud, the less likely the person is to get infected. However, he and his team have found that this likelihood increases with certain variants, such as Delta, which is far more transmissible than the previous versions of SARS-CoV-2. That’s because per unit of respiratory droplet, there is more virus if it’s the Delta variant compared to the Alpha variant. “Our data suggests that there is a lot more of it in the air,” he says, which could explain why people get infected with Delta so quickly if they are around someone who is already infected. The Tokyo Olympics infection control measures are pretty strict about preventing the importation of COVID-19 by Olympic travelers. But given that the bubbles aren’t perfect, and that the practical pressure to move thousands of journalists around in a short period of time precludes the proper social distancing, the virus is likely finding ways to keep flourishing. Health officials can only hope that intensive testing and contact tracing will pick up cases as quickly as possible to contain them. Read more about the Tokyo Olympics:
from https://ift.tt/2V7SSI8 Check out https://takiaisfobia.blogspot.com/
0 Comments
The Opening Ceremony provided the first taste of what an Olympics without fans is like—devoid of the normal buzz of excitement and roar of the appreciative crowd, it was more solemn than celebratory. But it’s one thing to miss the noise for Opening Ceremony, quite another when it’s gone from the competitive events. Not every sport will be as affected by the loss of spectators at the Tokyo Games. Athletes competing in events like archery, which requires concentration and quiet, for example, might actually appreciate the respite. But team-based sports and events like swimming races might seem, well, a little flaccid without fans. Ask athletes if the lack of fans will affect them, and they have their standard answer—they train to compete under any and all conditions, so while it will be weird, they’re ready to push themselves even if nobody is there in person to spur them on. But the reality is that any deviation from the norm has a potential impact on performance, so the quiet of an essentially empty stadium can be unnerving. Like it or not, consciously or unconsciously, athletes take their cues from vocal spectators—encouraged by claps and cheers, and even motivated by boos. “Crowd noise and excitement are something that increase athletes’ adrenalin even further,” says James Houle, lead sports psychologist for Ohio State Athletics. “Without a crowd, athletes will really have to find that energy within themselves or from their teammates. They will have to rely on each other more than ever to help with that energy.” 
And there’s some early, intriguing evidence that having an audience has a quantifiable physiologic effect on the brain. Vikram Chib, associate professor of biomedical engineering at Johns Hopkins University, has studied how the presence of observers can affect people’s performance. He analyzes people’s performance on skilled motor tasks that he trains people to do in the lab, either in front of observers or alone. He found that a part of the brain related to theory of the mind, which processes thinking about what others think of you, become more activated when people are being observed. “We think theory of mind areas feed into how you process motivation, and is what gives rise to performance in an audience setting,” he says. The region of theory of the mind is closely linked to how the brain processes incentives. In Chib’s study, the participants were taught certain skills and offered money if they performed well. “What we do know for certain is that having people watch boosts incentive,” Chib says. “So for athletes, incentives are multi-dimensional—it’s not just the fans, but they are playing for their country, and for the payoff of years and years of training.” For elite athletes at the Olympic level, Chib says the presence or absence of fans may not have as large an impact on performance as it might for less accomplished athletes. So the top podium contenders at the Olympics, for example, may not experience much of a difference by competing in an empty arena. But for other athletes, the lack of fans may keep them from achieving personal bests that the adrenalin rush of competing under the rings might otherwise have provided. “That little bump of having the crowd behind them might have helped them achieve their personal best,” he says. Most other studies on the subject to date explore home field advantage and have produced conflicting results, with some finding that the energy of a home crowd can spur more victories, while others found little impact. Already, the pandemic has provided some additional data on the impact of fans (or lack thereof). A study of Germany’s Bundesliga, for example, the first major sports league to resume games after the pandemic started—without fans—showed that the lack of spectators did affect the soccer players’ performance. Over six weeks playing to empty stadiums, home victories dropped by 10%, players took fewer shots on goal and they scored less than they had before stadiums full of people. Such studies on the presence—or absence—of fans are just beginning, and unusual circumstances during the pandemic like the Olympics sans spectators could provide a living lab for scientists like Chib to learn more about how athletes are affected by competing in front of others. But in the meantime, Olympic athletes and coaches are coming up with other ways to simulate the missing crowds. “We’re going to make that venue loud even if it’s just us in there,” says Team USA Swimming men’s coach Dave Durden, of the swimmers who plan to sit in the stands if they are allowed, and cheer on their teammates. At the top of the elite level, most athletes are used to compartmentalizing, especially in sports like track and field or gymnastics, where more than one athlete competes at a time in different events. So walking out to an empty arena might not be as disconcerting to the most seasoned athletes—and might even help some who get nervous while competing to make the biggest competition of their lives feel more like another practice session. “I personally love hearing the crowd noise if I’m behind,” U.S. swimmer Chase Kalisz said during training camp in July. “I love the crowd, love the noise and love packed arenas. But swimming is a solitary sport, and during training you spend most of the time in isolation by ourselves, so I don’t think personally it will be a big factor.” 
Still, it might take some getting used to, and Houle relies on visualization to acclimate his athletes to a new situation like competing without fans. “When I work with people on visualization, I tell them to look around the arena, and imagine people in the stands,” he says. “And some people practice with crowd noise to prepare. Now I would tell Olympians to go into the arena, look around, and that is it—that’s what it’s going to look like.” “It’s definitely a bummer because we always enjoy having fans,” says Simone Manuel a swimmer on Team USA in Tokyo. “But at the end of the day, once you dive in it’s about swimming fast and getting your hand on the wall first.” Because the clock doesn’t know if fans are there or not. Read more about the Tokyo Olympics:
from https://ift.tt/3kTslcC Check out https://takiaisfobia.blogspot.com/ Like many 18-year-olds, Kelly Danielpour is preparing to start college in the fall, planning out her classes, buying dorm necessities and wondering what her roommate will be like. Unlike many 18-year-olds, she’s also spending her spare time helping teens across the country navigate vaccine-hesitant parents and get their COVID-19 vaccines. As the highly contagious Delta variant spreads, posing a greater risk for people who are unvaccinated and stoking fears of a fourth wave of COVID-19 cases, health experts are urging more Americans to get vaccinated. “This is becoming a pandemic of the unvaccinated,” Rochelle Walensky, director of the Centers for Disease Control and Prevention, said at a press briefing on July 16. And the looming start of a new school year has fueled debates over vaccine and mask requirements for returning students. “There are so many teenagers who are unvaccinated. There are so many adults,” Danielpour tells TIME. Danielpour founded VaxTeen last year to help young people access vaccines and learn about their options if their parents don’t want them to get vaccinated. “A vaccine is a collective health measure. We all have to take part for it to be truly effective.” Vaccination rates are lagging, particularly among young people. Just 42.6% of 18- to 24-year-olds in the U.S. are fully vaccinated against COVID-19 — a smaller percentage than any older age group, according to a Mayo Clinic tracker. Among minors, 38% of 16- to 17-year-olds and 25% of 12- to 15-year-olds were fully vaccinated as of July 14, according to an American Academy of Pediatrics analysis of CDC data. Read more: See How COVID-19 Has Spread in the U.S. and Around the World That analysis also found the pace of child vaccinations is slowing, dropping to 315,000 new vaccinations during the week of July 14 — down from a peak of 1.6 million child vaccinations at the end of May, when children ages 12 and older became eligible to receive the Pfizer-BioNTech COVID-19 vaccine. <strong>“They said that a teenager couldn’t have possibly created the site.”</strong>That’s what worries Danielpour, who just graduated from high school and lives in Los Angeles, where county leaders recently reinstituted a requirement to wear masks indoors due to rising COVID-19 cases. She started the research for VaxTeen before the pandemic, after coming across a Reddit post from a teenager who wanted to get their routine adolescent immunizations but whose parents opposed vaccines. Danielpour fell down a social media “rabbit hole” and encountered lots of other teens in similar situations. Most wanted to know if they could consent to vaccines on their own, without parental permission, and how they could go about getting them. “I was just in awe, and I also realized how many barriers were in place,” she says. “Whenever we talk about sort of the anti-vaccine movement, we always just talk about parents. We don’t really think about kids having their own opinions on this, or being part of this conversation or having the potential to be the decision makers. She wanted VaxTeen to be a resource for those teens, and her work became newly urgent amid the COVID-19 vaccine rollout and the pervasiveness of vaccine hesitancy. 
Nearly a quarter of parents say they will definitely not get their child vaccinated against COVID-19, and 18% said they will only get their child vaccinated if schools require it, according to a recent survey by the Kaiser Family Foundation. “The best thing you can do for yourself and for everyone else is to get vaccinated if you can,” says Joshua Petrie, an assistant professor at the University of Michigan School of Public Health who studies epidemiology and the transmission of respiratory viruses. “The vaccines have been incredibly effective, and they’re our best shot at keeping things at lower levels, particularly with the Delta variant picking up speed here in the U.S.” Ahead of the new school year, the issue of youth vaccinations and school vaccine requirements has grown more divisive. The American College Health Association recommends that colleges require the COVID-19 vaccine for all on-campus students this fall, but some states have prohibited K-12 schools and colleges from imposing such requirements. This week, a federal judge upheld Indiana University’s requirement that all students and faculty be vaccinated against COVID-19. The student plaintiffs, who object to the vaccine mandate, plan to appeal. Read more: A Fourth Wave of COVID-19 Is Brewing in the U.S. Is There Enough Time to Stop It? Facing pressure from conservative lawmakers as vaccine misinformation spreads, the Tennessee Department of Health plans to end adolescent vaccine outreach and stop holding COVID-19 vaccine events at schools, according to a report by the Tennessean on July 13. And lawmakers in other states have introduced legislation on either side of this issue. To the extent that teens aren’t getting vaccinated because of apathy or lack of awareness, the Biden Administration has ramped up outreach to young people, launching a COVID-19 Student Corps to get teens to advocate for the vaccine among peers and the COVID-19 College Vaccine Challenge to encourage colleges to boost vaccination efforts. VaxTeen has focused on teens who want to be vaccinated but who can’t get the shot because of their parents. Young people consistently email Danielpour and reach out over Twitter and Instagram, asking for help and advice. She also scrolls through Reddit and Twitter for posts from teens sharing their vaccination questions and dilemmas. “I just want to be able to go to school in person,” wrote one student on Reddit, who identified herself as a 16-year-old who “can’t change my parents’ minds” about vaccines. “I feel like my health and my concerns are just being completely disregarded,” wrote another 16-year-old girl on Reddit, referring to her mother. “Any advice on how to convince her?” Danielpour responded to both of them, sharing guides on which states allow teens to be vaccinated without parental consent. She has focused her efforts both on access—helping teens find a vaccine clinic along their bus route that’s open on weekends, for example—and awareness, sharing fact-based vaccination information for them to take back to skeptical parents. “In many cases, convincing a parent is a teen’s only option,” she says. Danielpour has received pushback and some hateful comments on social media and in emails from people who disagree with the work she’s doing. Some argue that vaccination decisions should be a discussion only between parents and their children. Others have pushed baseless conspiracy theories that VaxTeen is run by a pharmaceutical company. “They said that a teenager couldn’t have possibly created the site,” Danielpour says—an accusation she tried to take as a compliment. “They don’t think a teen could have possibly done it, and I did.” Read more: Applying to College Was Never Easy. The Pandemic Made it Nearly Impossible She usually reads the opposing comments anyway to better understand vaccine polarization. “It is coming from a place of fear, and the better I understand that, the better VaxTeen’s work will be,” she says. The website directs teens to resources on debunking vaccination myths and talking to parents about vaccines, including questions parents might ask and how best to answer them with factual medical information. If that doesn’t work, the site also includes a guide to each state’s laws on parental consent. Forty states currently require parental consent for children under 18 to be vaccinated, and Nebraska requires it until age 19. Some states allow a minor to “self-consent” at a certain age—14 in Alabama and 16 in South Carolina, for example. And other states, without specifying an age, give healthcare providers the ability to decide if a minor is mature enough to consent to vaccination on their own. In some parts of the country, legal challenges have been issued that would reduce teen access to vaccines. A bill under consideration in South Carolina would prohibit minors from getting the COVID-19 vaccine without parental consent. Meanwhile, two federal lawsuits filed this month are challenging a law passed in Washington, D.C., last year that allows children 11 and older to get vaccines without their parents’ consent. Danielpour would like to see all states let teenagers be vaccinated without parental permission. “I don’t deny that a parent’s job is to keep their child safe. And if you’re encountering a lot of misinformation, then that can scare you,” she says. “But I also think that there’s a line in some sense, and that the more present fear—and the fear based in fact—is of the virus and seeing what it’s doing to everyone.” More than 600,000 people in the U.S. have died from COVID-19. And while children have been less likely to get seriously ill from the virus, they also lost out on formative experiences and rites of passage during the pandemic. Danielpour, who got a COVID-19 vaccine as soon as she could, acknowledges that the return of a traditional high school experience or typical life on a college campus hinges on widespread vaccinations. “There’s so much that depends on that — going back to school or back to normal life, having friends, being in a classroom,” she says. “There are invaluable experiences that are part of growing up that depend on our vaccine success.” from https://ift.tt/2WcqHs8 Check out https://takiaisfobia.blogspot.com/ Dr. James Antoon, an assistant professor of pediatrics at Vanderbilt University Medical Center, often goes an entire summer without diagnosing a single case of respiratory syncytial virus (RSV). The common illness, which typically results in mild, cold-like symptoms but can be severe in infants and elderly adults, usually goes along with the winter flu season. But this summer, RSV cases are spiking, particularly in southern states. Around 2,000 confirmed cases were recorded across the U.S. during the week of July 10, 2021, compared to less than a dozen during the week of July 25, 2020. The actual number of infections is likely higher, since clinicians may not test sick children for RSV outside its usual season, the U.S. Centers for Disease Control and Prevention (CDC) said in a recent advisory. The spike is somewhat logical, even if the timing is unusual. When the pandemic hit, sending people inside and behind masks, respiratory illnesses like RSV circulated at “historically low levels,” the CDC said in a report published today. Now that people are easing up on COVID-19 precautions, they are also coming back into contact with pathogens that have existed, but weren’t spreading much, throughout the pandemic. RSV infections began to tick upward in April 2021, the CDC says. In the U.S., RSV case counts are “incredibly high for the summer,” Antoon says, “but it’s about on par with what we see in the winter.” That suggests COVID-19 prevention delayed the normal RSV season. A similar RSV spike happened during Australia and South Africa’s summer seasons. But what’s harder to explain, Antoon says, is why RSV is circulating widely while some other respiratory viruses, like influenza, aren’t. (Though infection rates for parainfluenza, which causes croup in children, are also rising right now, he notes.) RSV is quite transmissible, more so than some other viruses. But one reason for the surge may be that children who typically wouldn’t be susceptible to RSV are vulnerable this year. Human immunity builds up over time. You’re likely to have the worst reaction to a pathogen the first time you see it. After that, your body knows what it’s up against and is better at fighting it off. Typically, the CDC says, almost all children catch RSV in their first two years of life. But babies who were born during or shortly before the pandemic may not have encountered RSV as they usually would have, meaning they’re extra susceptible to it now. “These viruses don’t disappear in the summer; they’re just much, much lower in frequency,” explains Dr. Richard Malley, a senior physician in pediatrics at Boston Children’s Hospital. Coming off a year when few children got RSV during its usual season, infections may spike “at times when they would normally not be present, presumably because a little bit of the immunity in the whole community was not reinforced by exposure,” he says. That’s no reason for parents to panic, Antoon says. “All the instructions we give to parents winter after winter apply this summer,” he says. At the top of that list is monitoring symptoms. Mild symptoms like a runny nose, coughing and sneezing aren’t cause for alarm, he says—but if a child has trouble breathing, is very lethargic or can’t keep down food or water, they should see a doctor. Adults infected with RSV usually develop nothing more than cold-like symptoms, but elderly adults should be on the lookout for more severe issues, like dehydration or trouble breathing. Beyond that, Antoon says, parents should teach the same disease-prevention practices they did prior to the pandemic, like frequent hand washing, covering coughs and sneezes, and staying home when someone in the household is sick. That’s especially important with the start of traditional flu season only a few months away. “Reduced circulation of influenza viruses during the past year might affect the severity of the upcoming influenza season given the prolonged absence of ongoing natural exposure to influenza viruses,” the CDC warned in its July 22 report. That will make disease mitigation, and flu vaccination, crucial this year. from https://ift.tt/3zt78Kf Check out https://takiaisfobia.blogspot.com/ Jackson Avenue is the main road that cuts through Oxford, Miss. At its northern limit, it circles the Ole Miss campus where Raven Saunders had spent the past three years as a student athlete. At its western end, Jackson splits into a T junction populated by a cluster of familiar American fast food restaurants and retail chains: a Walmart Supercenter, a Home Depot, a Popeye’s, a Chick-Fil-A. Saunders, a senior at University of Mississippi and a star shot putter on the school’s track and field team, knew the intersection well. Turn right, and the road led home. Turn left, and the highway hugged a steep drop-off floating above towering trees below that Saunders had found herself thinking more and more about in January of 2018. Her last year in college hadn’t been easy. She won four NCAA titles while at Ole Miss, and finished fifth at her first Olympic appearance in Rio in 2016. But after an injury in 2017, she couldn’t defend her NCAA title and came in 10th at the world championships. The pressure of balancing academics and sports at an elite level was starting to tear her apart. Because the track season ended as the next school semester began, she never had a true break as a student-athlete—every year, less than a week after returning from world championships, she was back in the classroom. After competing at the Olympics in Rio, she had to pick up her studies two days later. “I was drained,” she tells TIME, days before competing to make her second Olympic team in June. “I would cry a lot and go into isolation. I had suicidal ideation. I thought about different ways to make it happen.” One morning in January 2018, those thoughts hijacked her brain completely. “It was just too much,” she says of the building pressure and depression. Knowing she had a full day of school, practice and other appointments that started at 8:30 a.m., she woke up in a daze and didn’t leave her house until 11:30 a.m.. Instead of driving where she needed to go and checking things off her to-do list, she drove to those places and kept going. “I rode past every place I needed to stop and get things done, and kept going,” she says. “I felt it was like a goodbye and I was going to see everything one last time.” 
Driving west on Jackson Ave. toward the junction, Saunders was ready to take the left toward the drop-off. Something, however, prompted her to text her therapist, whom Saunders trusted completely. Saunders told herself that if her therapist didn’t answer by the time she reached the Walmart, she would take the left hand turn. Just before Saunders got to the light, her therapist responded. “She texted back, ‘I got you, just breathe, calm down,” says Saunders. Saunders turned right, went home and cried. At her therapist’s suggestion, she went to the school and informed her coach about what had just happened, and asked for help. Together with her therapist, he helped Saunders get admitted to a facility for two months. “Man, that was some of the toughest work I’ve ever done,” she says of that stay. She credits it, however, with saving her life, and with teaching her the skills she now relies on to work through her dark moments. On June 24, at the sweltering U.S. Olympic Track and Field Trials in Eugene, Ore., Saunders launched the shot put for a personal best throw and made the team. While their achievements and glorious exploits, chronicled in broadcasts around the world, may make it seem like Olympic athletes live charmed and angst-free lives, that’s far from the case. Saunders’ story is hardly unique. More athletes are reporting mental health issues such as anxiety, depression, psychiatric conditions and eating disorders. The exact percentage of Olympic athletes with mental health concerns isn’t clear, since it hasn’t been recorded. But given the incidence in the general population, coupled with the added pressures of the pandemic and Olympic competition, “the majority of athletes should be using mental health support,” says Naresh Rao, head physician for USA Water Polo and member of the U.S. Olympic and Paralympic Committee (USOPC) medical team at the Tokyo Olympics. “If you look at the percentages of people who have mental health illness in general, it ranges from 40% to 50%. Throw in the pandemic, and the fact that many of these athletes are teenagers or young adults, and you start to see the percentage could go up to as high as 70%.” In some ways the four-year cycle of fame and fallow is similar to the highs and lows of an addictive drug. The withdrawal after the exhilaration of competing, no matter the outcome, is a mental crash that can hit athletes hard. It’s not just the sudden fame that can be disorienting, but the often disturbing realization that after years and sometimes decades of training and devoting themselves to perfecting their sport, they’ve allowed themselves to be defined by their results and their medals, or lack thereof, and may have lost themselves in the process. “I just kept coming back to the idea that I just don’t know who I am without gymnastics,” says gymnast Sam Mikulak, who will compete in Tokyo on his third U.S. Olympic team. During the pandemic, the time away from the gym forced him to confront what he had been dismissing for years. “I was going through an identity crisis and asking myself how I can find happiness, where is the happiness if I don’t have this sport.” 
Read more: COVID-19 Shutdowns Have Taken a Massive Toll on Elite Athletes’ Mental Health And yet, Olympians’ mental health has never been a key concern for the sports governing bodies that oversee them. “It’s as if mental health issues weren’t there, and wasn’t talked about,” says Saunders. “If you got a problem, you deal with it. And if you have any type of mental health problem, people think you’re crazy or something is wrong with you, or you’re off. That’s how I grew up thinking about it.” Physical injuries have long been managed with detailed protocols and services, but coaches and event organizers rarely considered the mental state of athletes, much less ensured there were resources available to address any issues. Tennis star Naomi Osaka highlighted this deficiency by pulling out of the French Open in May, after backlash over her decision not to participate in any press conferences to protect her mental health. But heading into Tokyo, that may be starting to change. Admissions like those from Michael Phelps, who admitted he too experiences depression and was suicidal after his fourth Olympics, have prompted the International Olympic Committee (IOC) and national Olympic bodies including the USOPC to directly address mental health in the same way they advise athletes on nutrition and recovery from physical injury. Tokyo will mark the first time the IOC has guidelines for athletes and their coaches to educate, screen for, and manage mental health issues, the work of independent experts it convened on the subject for the first time before these Games. The USOPC also has more concrete and detailed mental health resources for Team USA athletes, including deeper screening for potential issues that athletes themselves might not be aware of or willing to admit, and referral and treatment options if they need them. Team USA in Tokyo will also include, for the first time, four mental health professionals—a psychologist, two psychiatrists, and a social worker— and each Team USA sport will also have its own dedicated psychologist. The British Olympic Association has a similar team of mental health professionals traveling to Tokyo with Team Great Britain for the first time, while Softball Australia will monitor athletes’ sleep habits on an app as an indicator of potential issues. “Just to know that [these resources] are on hand if you need them is awesome, especially for the younger kids growing up in sports who can reach out and get help if they need it to be better competitors and better athletes,” says gymnast Simone Biles, who works with her own therapist. “It’s a work in progress, and we could certainly be doing things better to improve mental health services, but things are moving in the right direction in terms of supporting athletes with regard to their well being and mental health,” says Nicole Ross, a fencer competing in Tokyo who serves as an athlete representative on a USOPC mental health task force. Stigma remains a problem, however, since the mantra particularly at the elite level is grit your teeth and push through any pain, physical or emotional. “The athletic culture in general is one in which you are driven to continuously push your body and in some cases your mind to the maximum potential,” says two-time Olympic swimming gold medalist Simone Manuel, who revealed at Olympic Trials in June that she experienced depression related to overtraining syndrome. Only recently with prominent athletes like Phelps and Saunders sharing their own struggles with mental health issues is that taboo slowly being eroded. As more athletes vocalize their own experiences, organizations like the USOPC are also finally devoting more resources to addressing the mental health of their athletes and providing them with the tools to improve their mental well being. ‘Athletes are not perfect, flawless gods’“Five years ago, mental health among elite athletes was not a very often-discussed topic,” says Dr. Claudia Reardon, professor of psychiatry at the University of Wisconsin. If there was any focus on athletes’ mental health, it centered around performance and ways to optimize results on the field. “Most of the emphasis when it came to mental health was around sports psychology and performance, and offering resources to help you perform at your highest level,” says Ross. “Occasionally in the health history [questionnaire] there might be some questions about mental health but they were sort of hidden, and weren’t prominent.” 
It wasn’t until 2018 that the IOC convened its first dedicated panel of experts to address all aspects of mental health—the IOC had already tackled other topics such as nutrition and serious physical injuries, but never mental health. The IOC reached out to Reardon and Dr. Brian Hainline, chief medical officer of the NCAA, to co-chair its first working group on the topic. Over several meetings since, Reardon says the group has worked to reach consensus in addressing the biggest barriers in mental health, including stigma and access to resources, across different countries with differing societal norms around mental illness. “When we looked at the world’s research, it was not a surprise to any of us that, lo and behold, elite athletes suffer from depression and anxiety at rates at least equal to—and in many cases may even exceed—general population rates,” says Reardon. “Athletes are not perfect, flawless gods.” One critical recommendation of the consensus statement focused on the first step in addressing mental health issues—recognizing and diagnosing it in the first place. In September 2020, the working group published two screening tool questionnaires to better identify potential issues among elite athletes. One, the Sports Mental Health Assessment Tool (SMHAT), was meant for medical professionals to use, and another, the Sport Mental Health Recognition Tool (SMHRT), was designed to help coaches, friends and family of athletes to identify mental health signs and symptoms. “We can’t rely on athletes universally to bring up and discuss issues related to mental health,” says Reardon, pointing to the long-standing stigmas within the community. The key was to suggest that the SMHAT be part of routine physicals that athletes are used to getting before their seasons start or in order to enter major competitions. That normalizes mental health more by putting it on par with physical evaluations, and doesn’t require the athlete or anyone close to the athlete to specifically request or flag a possible mental health issue. The survey is crafted to raise alarms for any signs that athletes might be a harm to themselves or others, and to immediately connect them with the appropriate support. After the USOPC began using the screening tool with USA Swimming and USA Soccer, Jessica Bartley, the USOPC’s first director of mental health services, says “I was surprised by the number of athletes who were identified as having mental health concerns.” About 80 athletes, or 58%, of the 165 who filled out the questionnaire were identified as potentially having a mental health issue, and Bartley called each to see if they were already getting the help they needed, and, if not, to connect them to a new registry of 150 psychologists and therapists that the USOPC launched in April. The tool identified four athletes as potentially at risk of self-harming behaviors or having suicidal ideation, and Bartley reached out within 15 minutes of receiving their results. “They were all a little surprised when they got a phone call right away,” she says. All four were already working with mental health professionals, and Bartley made sure that they were satisfied with the support they were receiving. If those athletes hadn’t already had a mental health team, Bartley would work with them to create one, including providing financial support for any therapy or residential care they might need. In May, Bartley worked with an athlete who needed treatment for an eating disorder, and helped that athlete find the appropriate treatment center as well as coordinate lodging and payment through insurance, which is covered by a Medical Assistance Fund created by a USOPC donor for $1.5 million that is dedicated to mental health needs. Standardizing that type of reimbursement and access is trickier in other parts of the world where mental health services either aren’t as widely available or financially supported. “It’s all well and good and easy for me to say that everyone should have access to an experienced sports psychologist,” says Reardon “But that’s not relevant in the majority of the world. So it requires us to think about community healers, religious leaders and others who may be in a position to help notice mental health concerns and intervene in culturally appropriate and sustainable ways.” So the IOC is also working on building a network of mental health professionals, including culturally relevant resources such as faith healers and other community leaders in countries around the world, to whom it can refer athletes if needed. ‘Our vulnerability as athletes is going to make us stronger’The second screening tool, the SMHRT is designed for coaches, friends, family members and any non-medical professional who might be close to an elite athlete. Many people who aren’t formally trained in mental health aren’t comfortable approaching athletes even if they sense they are struggling, out of fear they aren’t qualified to help them. “When they don’t know what to do, they don’t do anything. But by not saying anything doesn’t mean they don’t care,” says Reardon. The SMHRT provides exact language for guiding that discussion, and initiating a critical conversation that could save that athlete’s life. It was just such a conversation that finally helped four-time Olympian Allison Schmitt to face the darkness that had been shadowing her for years. To swimming fans, Schmitt is “Schmitty,” easy-going and perpetually smiling, known among teammates for her corny jokes and an easy laugh. She admits that at her Olympic debut in 2012, she swam better than she even expected, and became an instant celebrity when she returned home to Michigan and then in Baltimore, where she trained alongside Phelps, who became a close friend. The attention and whispers of people who recognized her on the street were unnerving, and Schmitt increasingly felt exposed and uncomfortable with her newfound visibility. But it was hard to admit those feelings. “Everything has always gone my way, and I was very grateful for the life I had, the opportunities I had, the successes I had,” she says. “So it was very hard for me to accept that I was struggling because I didn’t want to seem ungrateful.” 
Instead, Schmitt bottled up the growing sadness and mental anguish. “It got to the point where I was lying in my bed crying because I didn’t know if I wanted to live any more. I didn’t want to die, I just didn’t want to be living through what I was going through any more.” Months after returning from London, Schmitt’s uncle died by suicide, and “it wasn’t really talked about,” she says. Then, three years later, Schmitt’s 17-year old cousin died by suicide as well. A star basketball player on her high school team, she never discussed her mental torment with Schmitt, nor did Schmitt share her own feelings of inadequacy and purposelessness. To this day, it haunts Schmitt, who gets emotional thinking about what could have been. “That suicide really turned my eyes,” she says. “If she would have shared with me what she was going through, could I have helped? And if I had shared with her what I was going through, maybe she wouldn’t have felt so alone.” Determined not to have her cousin’s death be in vain, Schmitt decided to share her own experience with depression, in the hopes that others would feel more comfortable than she did in admitting they need help and in getting that help. Hearing from teammates or other elite athletes is critical to building a new culture around mental health in high level sports, says Ross, who makes sure that her USA Fencing teammates are aware of the mental health resources that are available to them. “I honestly think it will take individual athlete ambassadors to go directly to their sport and talk to teammates and the national governing body staff about what resources are available, and how they were able to successfully use those resources,” she says. “That grassroots effort is what it is going to take to reach the largest number of athletes.” And that shouldn’t end when the competition does. For the first time, the USOPC has created a support group for athletes who don’t make the team, as well as those who struggle with readjusting to life after retiring. Bartley and her team are also reaching out to athletes every time they experience a major injury or life event that could impact their training or career goals. “That’s never happened before,” says Rachel Flatt, a member of the 2010 Olympic figure-skating team and now an athlete representative of the USOPC mental health task force. Learning to cope with the post-Olympic period, whether it’s the four years before their next Olympics, or retirement, is a growing focus of these mental health efforts. When the pandemic lockdown disrupted gymnast Mikulak’s regular training schedule, he finally confronted something that he had been pushing aside in recent years: what he would do once he stopped competing. “It was scary to think what was going to happen after I retire when I don’t have my gymnastic goals any more that I was constantly pushing for and seeking,” he says. “All of that was going to be gone. The more I looked into my future, the more fear I felt. I just really freaked out.” He started working for the first time with a sports psychologist to address his anxiety, and his broader struggle with his sense of identity outside that of being a gymnast. Together they confronted why, at critical moments when Mikulak had been just a performance away from achieving his dream of winning an Olympic medal, he made costly mistakes. “I was trying to be the most scientifically perfect specimen of gymnastics,” he says of his three previous Olympic experiences. “I felt if it doesn’t happen here, it will never happen anywhere else. So when the pressure I felt was at its greatest, at the 2016 Games, and I had a couple of chances for a medal, I fell short. I was focusing 100% on my physical ability and I did nothing for my mental fitness.” That changed thanks to his work with his therapist, so preparing for the Tokyo Games, he says, was very different. “I could tell, as we were getting closer to Tokyo, that I was starting to feel the same pressure. But this time, my expectations for them is to have no expectations,” he says. “I’m going out there with the intention of doing nothing more than I can do in that moment, and be proud of that, and happy with that. I’m going to go out there on my own terms, and not on anyone else’s.” Like Mikulak, Schmitt has found a new power in speaking out about her journey with depression. “I am personally accepting that speaking out and getting help and being vulnerable is strength,” she says. “And that strength has helped me. Our vulnerability as athletes is going to make us stronger in the long run.” If you or someone you know may be contemplating suicide, call the National Suicide Prevention Lifeline at 1-800-273-8255 or text HOME to 741741 to reach the Crisis Text Line. In emergencies, call 911, or seek care from a local hospital or mental health provider. Read more about the Tokyo Olympics:
from https://ift.tt/3rtEOEV Check out https://takiaisfobia.blogspot.com/ Life expectancy in the United States dropped the most in more than seven decades last year as Covid-19 sent hundreds of thousands of Americans to early deaths. The pandemic’s disproportionate toll on communities of color also widened existing gaps in life expectancy between White and Black Americans, according to estimates released by the Centers for Disease Control and Prevention. The tally represents an extraordinarily grim accounting of an ongoing catastrophe. The first year of the pandemic delivered a bigger blow to American life expectancy than any year of the Vietnam War, the AIDS crisis or the “deaths of despair” that nudged down life expectancies in the mid-2010s. “It’s staggering and depressing,” said Noreen Goldman, a professor of demography and public affairs at Princeton University. “The U.S. lags behind virtually all high-income countries in life expectancy, and now it’s lagging further behind.” The pace of Covid-19 deaths dropped sharply as vaccinations spread in the first half of 2021. But it’s unclear how long it will take for life expectancy to rebound. The U.S. has recorded a total of 609,000 Covid deaths since the pandemic began. More than 43% occurred in 2021, with almost half the year still to come. The first year of the pandemic reduced Americans’ life expectancy at birth by 1.5 years, to 77.3 years. That erased the country’s gains since 2003. It was the largest annual decline since 1943, in the middle of World War II. Goldman said that it was the second largest decline since the 1918 influenza pandemic, which is believed to have killed some 50 million people worldwide. The 2020 pandemic decline widened the distance between the U.S. and other wealthy democracies like France, Israel, South Korea and the U.K., according to research recently published in The BMJ journal. “This is not a decline that happened in other high-income countries, so something went terribly wrong in the U.S. where the number of Americans who died was vastly in excess of what it needed to be,” said Steven Woolf, director emeritus of the Center on Society and Health at Virginia Commonwealth University and one of the authors of the BMJ study. Life expectancy is a statistical construct that reflects death rates in a given place and time. The CDC report describes life expectancy at birth as the “average number of years a group of infants would live if they were to experience throughout life the age-specific death rates prevailing during a period.” It isn’t meant to predict the actual lifespans that people born in that period will experience. Rather, it’s a way to compare death rates across geographies and years. Covid accounted for three-quarters of the decline in 2020. Unintentional injuries, a category that includes record fatal drug overdoses for 2020, also dragged down the measure, as did homicides, diabetes and liver disease. The drop would have been steeper had it not been offset by fewer deaths from other factors including cancer, chronic lower respiratory disease, heart disease and suicide. All demographic groups saw declines in life expectancy in 2020. But the drops weren’t evenly distributed. Men lost more ground than women. Hispanic Americans, who have longer life expectancies than White or Black Americans, recorded the greatest losses during Covid, with life expectancy dropping three full years, double the rate of the country as a whole. Black Americans likewise recorded a 2.9-year loss of life expectancy. That decline widened the gap between Black people and White people in the U.S., a disparity in life expectancy that had been shrinking since the 1990s. Life expectancy for White Americans declined by 1.2 years in 2020. “There’s no biological reason for people of a certain skin color to die at higher rates of a virus,” Woolf said, noting that the disparate impact reflects structural inequities. Skewed representation in frontline jobs like retail, meatpacking, transport and health care, combined with higher rates of chronic conditions, put people of color both at increased risk of exposure to Covid and increased risk of dying from it, Goldman said. Unequal access to health care, language barriers, and crowded or multigenerational housing also contributed to the virus’s disproportionate toll on Hispanic and Black populations, she said. The estimates published by the CDC’s National Center for Health Statistics reflect death certificate data reported by states and cities. The report didn’t include data on populations of Asian Americans, American Indians, Alaskan Natives, Native Hawaiians and other Pacific Islanders. As alarming as the one-year drop in life expectancy in 2020 is, Woolf said that more attention should focus on the decades-long gap in life expectancy that has cut short more American lives than Covid has. In the 20th century, life expectancy generally increased in wealthy countries as science and sanitation helped conquer infectious diseases. In the U.S., troubling signs that the country wasn’t keeping up with other nations’ gains in the measure emerged in the 1990s. This divergence came to be known as the U.S. health disadvantage. “The more important issue than the acute event we’re seeing right now in life expectancy is the long-term trend,” Woolf said. “That’s actually much scarier for the U.S. than what we’re reporting for 2020, as strange as that might sound.” from https://ift.tt/2UwGjGo Check out https://takiaisfobia.blogspot.com/ When COVID-19 began spreading in the U.S. in March 2020, McKale Santin was working at a nursing home in Burlington, Vermont. She and her coworkers didn’t yet know how deadly the virus would become, but she remembers feeling nervous as the first patients got sick and she was asked to examine them with only a surgical mask, not the more protective N95 mask that she wore to test for conditions like tuberculosis. One day, a patient pulled down her own mask to sneeze while Santin was conducting a respiratory assessment. Soon after, the woman became one of Vermont’s first people to die from COVID-19—and Santin fell ill. The 33-year-old nurse developed a deep, burning cough, and a fever so intense she would sweat through her bed sheets for weeks. Sixteen months later, she is still suffering from debilitating symptoms. Formerly a competitive cyclist and rock climber, Santin now has a difficult time climbing the stairs to her apartment, constantly feels fatigued, often loses her balance due to numbness in her feet, has swollen joints, and experiences brain fog. “So much in my life is different now,” she says. “It’s really slow progress. It almost feels like learning how to work your body again.” Santin is one of a growing number of so-called long-haulers—people whose symptoms linger many weeks or months after their initial case of COVID-19. Researchers estimate between 10% and 30% of COVID-19 patients develop long-term symptoms, though these can vary widely in their severity and how or when they appear. The U.S. National Institutes of Health has launched an initiative to study “Long COVID,” post-COVID clinics have popped up around the country and support groups are helping patients share their experiences. But for some long-haulers, the persistent symptoms have prevented them from returning to work full-time or at all, so they’re turning to a government system that’s supposed to help: Social Security disability benefits. While it’s not clear precisely how many new people will need these benefits, if 10% of the 34 million Americans who have had COVID-19 applied for disability, that would mean 3.4 million applicants—which doesn’t include spouses or children who might be eligible as well. Even if just a fraction of those long-haulers or their families apply for disability insurance, it could overwhelm the system, which currently supports 8.1 million disabled workers and 1.4 million of their family members. It’s already a vulnerable moment for the Social Security Administration (SSA). After successive administrations have ignored the looming retirement trust fund issues, the SSA has seen its budget cut dramatically in the last 10 years, even as its number of beneficiaries grew by 22%. It has closed 67 offices around the country since 2010 and shrunk its call center staff, resulting in more busy signals, longer wait times and fewer calls answered according to a report by the SSA Inspector General in May 2020. Even in normal times, the process for getting disability benefits is extremely stringent and hard to navigate, advocates say. But the system is particularly ill-equipped to handle COVID long-haulers, who experience a wide range of symptoms that defy easy documentation and often evolve in ways medical providers don’t yet understand. With the first long-haulers already seeking help, disability advocates are hoping that instead of millions of sick Americans getting stymied by bureaucracy and a struggling agency getting pushed to its breaking point, this can be a moment for reform. Advocates are urging the Social Security Administration to prepare for a coming wave of applicants, update its policies and issue guidance related to COVID-19 to better serve this mysterious and suffering population. “COVID long haulers represent the largest influx of new entrants to the disability community in modern history,” says Rebecca Vallas, a senior fellow at The Century Foundation and a former disability lawyer. “There have been a few key moments in history, and this is one of them, where we have not only the opportunity but the urgent imperative, to wake up and realize which policies are incredibly long overdue for change.” 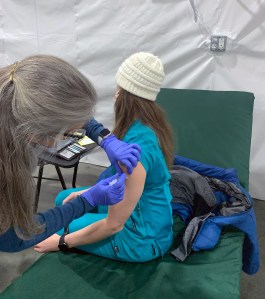
‘No two patients are the same‘Last summer, Santin tried to go back to work, first at a memory care facility and then in a primary care practice. But she was still fatigued, losing balance and unable to function like she could before. So when she had to stop working due to her health this spring, her doctors suggested she apply for Social Security disability benefits. Social Security Disability Insurance is supposed to be there for Americans who have paid into it, protecting them from the risk that every person faces of an unexpected injury or sickness that prevents them from working. But the system is notoriously complex. The U.S. has some of the most stringent eligibility criteria for disability benefits among countries with advanced economies, according to the Organization for Economic Cooperation and Development. The application is lengthy and can take months to complete. Getting approved often requires multiple appeals, and waiting for each hearing can take months on its own. Even then, fewer than four in 10 applicants are granted benefits. “As someone with brain fog, if I didn’t have the connection with a social worker and the case manager to help me, I wouldn’t be able to complete the forms,” Santin says. The laborious forms and appeals process aren’t the only impediments. To qualify for disability benefits from the SSA, an individual must show they have an impairment that prevents them from “substantial, gainful activity” that is expected to last at least 12 months or result in their death. But long haulers often don’t have the medical evidence needed to prove this, since many of them have barely been sick for 12 months and have the kinds of symptoms—fatigue, chronic pain, brain fog—that are difficult to capture with traditional screening tools, blood tests or imaging. Some symptoms can appear months after the initial infection, and doctors are still trying to figure out what causes them and how long they’ll last. “No two patients are the same,” says Dr. Noah Greenspan, a physician who started a long-haul treatment clinic in New York early in the pandemic. “So a lot of people are having difficulty getting the right diagnostic tests, and then even getting care.” Last June, Democratic Representatives John Larson of Connecticut, chair of the House Ways and Means Social Security Subcommittee, and Danny Davis of Illinois, chair of the Worker and Family Subcommittee, urged the Social Security Administration to work with the National Academies of Sciences, Engineering and Medicine (NASEM) to examine the long-term impact of COVID-19 on people’s ability to work. A spokesperson for the agency says it has been “regularly consulting” with NASEM “throughout the pandemic” and heard from experts on COVID-19 at a regularly scheduled National Disability Forum on Nov. 18. The spokesperson says SSA can evaluate COVID long haulers under its current rules, but, “Researchers are still learning about the disease and we will continue to look at our policies as research evolves.” In the meantime, benefits applications can languish for more than a year while the applicants struggle to live and pay their bills in uncertainty. If they try to work during this time, many worry that effort can be used against them. Wait times for hearings vary by office but can be up to 16 months in some parts of the country, according to SSA data. The backlog had been declining before the pandemic, but with pent-up demand from the last year and the likely influx of long haulers, wait times are expected to rise again. “It is a tremendously difficult time for claimants,” says Stacy Cloyd, director of policy and administrative advocacy at the National Organization of Social Security Claimants’ Representatives. “People sometimes lose their homes. People see their health decline, both because of the mental stress and because of a lack of access to health care during that time. It is a tremendous amount of stress on disability claimants and on their families.” Starting to changeLong COVID patients could spur changes to the system, as their plight has given more urgency to advocates’ demands. Stop the Wait, a coalition of disability and aging groups, is calling on Congress to eliminate official waiting periods built into the Social Security Disability Insurance program. After completing the application process, people have to wait five months for any benefits to begin and two years to receive Medicare coverage. “It’s a devastation both for the individuals and their families and for our economy, where people don’t have any money coming in, they can’t spend, they can’t contribute to the economy,” says Eve Hill, a disability lawyer and lead organizer of the campaign. It can also push people onto other government programs such as Medicaid, which states have to help pay for while the person is waiting for their federal benefits. In 2019, Democratic Sen. Bob Casey of Pennsylvania and Democratic Rep. Lloyd Doggett of Texas introduced a bipartisan effort to get rid of the waiting periods. The bills were not voted on then, but a spokesperson for Casey’s office said he plans to re-introduce the legislation this year. Since then, President Joe Biden included the issue in his disability plan on the campaign trail, Congress eliminated the waiting periods for people with amyotrophic lateral sclerosis (ALS), and the Stop the Wait campaign wrote an open letter asking Congress to do so for others with disabilities too. It’s not just waiting periods gaining attention in Washington. Groups like the Long COVID Alliance, Survivor Corps and Body Politic have come together to learn from how the government has handled other diseases such as fibromyalgia and chronic fatigue syndrome and advocate for new investments in research on long COVID. In April, the Senate Finance Committee held a hearing to examine the Social Security Administration’s customer service during the pandemic, and Senators from both parties said the agency needed to do more to simplify its applications, reach out to vulnerable communities and help eligible people apply for the benefits. To this end, Democratic Sen. Sherrod Brown of Ohio is working on legislation that would create a navigator program to help people apply for items like disability benefits or the Child Tax Credit, similar to the one used under the Affordable Care Act to connect people to health insurance. But such improvements rely on the Social Security Administration having adequate funding to process claims properly. Biden’s 2022 budget request included a 10% boost to SSA funding, but that is still less than the agency itself said it needs to do its job effectively, notes Kathleen Romig, a senior analyst at the Center on Budget and Policy Priorities who used to work at the SSA. “Even if 100% of these [long COVID] claims are denied, you still have to decide them. And that’s really time consuming. And so it’s going to take a lot of staff time. And it’s going to take a lot of money. As a result, it’s going to put even more strain on this agency that’s already under a lot of strain,” she says. However, Romig also notes that times of crisis are often when government programs get created or overhauled. After all, Social Security was created as part of the New Deal, the bold economic agenda President Franklin D. Roosevelt enacted as a way out of the Great Depression. “Social Security is something that was battle tested, in part because it was born out of such a similar circumstance,” she says. “Advocates see SSA’s main job now as making sure people have access to benefits after a period of some significant barriers to access.” There are signs Biden may agree with that mission. He recently fired the Trump-appointed Social Security Commissioner Andrew Saul, who clashed with the agency’s workers during his tenure and had proposed a host of more stringent rules for disability beneficiaries. “I expect that with President Biden’s recent removal of former Commissioner Andrew Saul and appointment of Acting Commissioner Kilolo Kijakazi, SSA will be rededicating itself to ensuring that people can access the Social Security benefits they have earned and are eligible for, including by properly evaluating the long-term effects of COVID-19 on the ability to work,” Rep. Larson said in a statement to TIME. There may be some progress in Washington, but in Vermont, Santin knows she still has a long road ahead. She is has been adapting to her new, more circumscribed life, but she says she feels lucky to have the support system of her doctors and case managers and is taking things one day at a time. “It’s wild,” she says, “the amount of work somebody with disabilities needs to put into the application for disability.” from https://ift.tt/2UoZCBC Check out https://takiaisfobia.blogspot.com/ Japanese health authorities have an aggressive testing plan in place for the Tokyo Olympics, but positive COVID-19 tests are already cropping up. With the Olympics taking place during a pandemic, in a city under a state of emergency, the Tokyo Organizing Committee has created a stringent set of policies governing how athletes and their coaches, trainers and other staff must behave to minimize the risk of both importing infections and spreading disease in the Olympic community. But even with aggressive testing, infections can happen. That’s because the virus is so unpredictable, and even though about 80% of athletes reported being vaccinated, the vaccines can’t prevent infections 100% of the time. [time-brightcove not-tgx=”true”] Already, the system has detected three positive cases in the Olympic Village, and at least a few more among athletes training outside of the Village, including the first positive test in a Team USA member, who is an alternate on the women’s gymnastics team. The cases in the Village, among members of the South African men’s soccer team, meant the entire team was isolated and prevented from training together until repeated tests among them continue to be negative. The strategy for keeping infections to a minimum over the coming weeks involves keeping Olympic-related visitors in as much of a bubble as possible, and testing everyone frequently. Any travelers from abroad are asked to minimize their travel 14 days before their Tokyo-bound flight, and to follow mitigation measures such as wearing masks, social distancing, and hand washing regardless of whether they are vaccinated or not. Read more: Meet 6 Heroes Who Helped Battle COVID-19 Before Competing in the Tokyo Olympics and Paralympics Once in Tokyo, athletes will remain in their designated training areas until several days before their competition, at which time they will move into the Olympic Village. To minimize risk of spreading the virus, athletes will dine in shifts or be allowed to bring their food back to their rooms. Most competitors will have one roommate, and are being asked to spend time only with their roommate and a small list of other close contacts such as their coach while in the Village. Each athlete is also required to download a health tracking app and answer daily questions about whether they experience any COVID-19-related symptoms. To get to their training sites or competitions, they can only take Olympic transport in cars or buses in which the drivers are tested and monitored as closely as the athletes are. Athletes will be tested daily, and their temperatures will be recorded every time they enter the Olympic Village. Olympic competitors will have two opportunities to spit into a specially bar-coded collection container—either in the morning or in the evening—and must be supervised by the designated COVID-19 Liaison Officer (CLO) of their respective teams. The results of the spit tests are made available about 12 hours later to the CLO, who then follows up with any athlete whose test comes back positive. To confirm the positive result, athletes will be asked to go to a designated clinic in a dedicated Olympic transport vehicle to the Village for another test, this time, one that involves a nasopharyngeal swab. The athlete will remain in the isolation ward of the clinic for three to five hours until the results are available. 
If the confirmatory test is also positive, then the athlete is moved to a dedicated hotel facility outside the Village, again in dedicated Olympic transport. Volunteers arrange to bring the athletes’ necessary belongings to the hotel. In the meantime, the athlete and the CLO work to create a list of immediate contacts—defined as those who were together 15 minutes or more while less than 1 m apart without wearing masks—who will then be asked to get another COVID-19 test. At this point, the Results Advisory Expert Group (RAEG) will review the case to determine if the athlete and the close contacts can continue competing. The RAEG is made up of eight members and 46 advisors; all eight of the members are doctors, with four having expertise in sports medicine, two in infectious disease and two in public health. The group will review every positive case on a daily basis and determine the risk of having that athlete continue to compete. “It’s hard to believe that they will be able to compete if it wasn’t a false positive, regardless of the sport,” says Dr. Naresh Rao, head physician for USA Water Polo and a member of the Tokyo medical team for the U.S. Olympic and Paralympic Committee. The RAEG provides the results of its reviews to the Infectious Diseases Control Center for Tokyo 2020, which then reports the group’s determinations to the respective Olympic committees of the athletes involved. The International Olympic Committee has said that any athlete or Olympic personnel who fail to comply with testing procedures or guidance from RAEG can face a range of penalties, from fines to suspension to deportation. Read more about the Tokyo Olympics:
from https://ift.tt/3BmUOx8 Check out https://takiaisfobia.blogspot.com/ With every passing day, the United States appears more likely to be on the cusp of a dreaded fourth wave of COVID-19 infections, even as the percentage of fully vaccinated Americans inches toward 50%. In the past two weeks, the number of average new daily cases has more than doubled, from 13,200 on July 4 to more than 32,300 on July 18, a surge that harbors grim reminders of the fronts of the second and third waves in the summer and fall of 2020. But on closer inspection, this surge looks significantly different than those we have seen in the past—and may very well be worse than it looks on the page. The coronavirus pandemic has never, even in its worst heights last winter, struck the U.S. uniformly. Instead, it has wandered from eruptions in specific urban areas to suburban and rural counties and then back again, like a persistent hurricane. Now, as the gap between states’ completed vaccination rates widens—Alabama has vaccinated just 33.7% of residents, compared to nearly 70% in Vermont—the per capita rate of new cases has clustered in a handful of regions where a majority of adults remain unvaccinated even as reopening continues apace. Here’s a county-level map of the 14-day growth of cases per 100,000 residents by county:  To draw on my amateur oceanography, the current crest resembles less a wave than a rip tide, with surges of current inundating several hotspots while the remainder of the country remains blissfully unaware (or unwilling to admit) that the pandemic is not remotely over. The upshot is that local data, rather than state- or nationwide-level figures, now paint the most accurate picture of the current state of the outbreak. “State-wide cases don’t tell the entire story. We need a finer-toothed comb,” says Jennifer Nuzzo, the lead epidemiologist for the Johns Hopkins University Testing Insights Initiative. As Nuzzo notes, the most recent documented outbreaks are more concentrated in rural areas than those of the worst spikes over the past 16 months (though the virus didn’t spare any corner of the country). What appears to be different now, even within more rural regions, is a blossoming of outbreaks that are at the moment highly clustered, particularly along the border between Arkansas and Missouri as well as northeast Florida and southeast Georgia. But any such observation comes with the same caveat that we on the Numbers Beat have been striving to communicate since the beginning: The number of cases is contingent on the number of people being tested for the virus, a figure that can only underestimate the true picture, not exaggerate it. Let’s recall: A year ago, COVID-19 skeptics, including then-Vice President Mike Pence, were attributing a spike in cases at the time to an increase in testing, a claim that was easily debunked. Now we face the opposite question: As the number of weekly tests has plummeted, taking a back seat to vaccination, and with the sense of urgency abating (for now), is the situation in fact worse than it appears? “I don’t worry that we are missing the severe cases,” including when a patient is hospitalized, Nuzzo says. “It’s everybody else I worry about. We have turned our telescope to a different part of the sky.” Murray Côté, an associate professor of health policy and management at Texas A&M University, agrees. “I still think we’re missing a chunk” of positive cases, he says. “It’s a confluence of things. We don’t have the testing facilities we used to have [earlier in the pandemic].” That chunk, both Côté and Nuzzo say, is likely made up of people who are experiencing mild or no symptoms, but can still be part of a transmission chain. I last spoke with Côté in June 2020 when unwinding Pence’s claim that the summer surge was a product of more testing. Our conversation this time felt both reversed, as we were discussing a possible under-calculation of reality, as well as strangely familiar, because a year ago, we were seeing a new surge amid a widespread relaxation of safety measures—not unlike the freedom from safety measures like maskless dining we currently enjoy. “We’re behaving exactly the same way as we did last year,” Côté says. To refresh your memory: Around this time in 2020, the U.S. had a brief moment where cases began to drop. Some Americans started to ease their social distancing and mask wearing, and it led to both a summer surge and, after another lull, the massive winter spike that turned out to be the worst stretch of the global outbreak to hit any country in the world. What’s different now is that this time we have highly effective vaccines—but, while inoculation can protect individuals, vaccination rates in many communities across the U.S. remain too low to prevent fresh outbreaks. In the heady days of spring, 2021, many states began reducing the frequency of their reports on new cases to every few days or once a week. That was a foolish mistake when, even with a massive reduction in testing, the seven-day rolling average of new cases never dipped below 10,000 at the national level. Given that the best-case scenario—even before the emergence of the Delta variant—was a reduction of cases and deaths to endemic levels for years to come, states must pair their desperate attempts to vaccinate more individuals with a renewed focus on surveillance and contact tracing. For now, the best way to prevent the current spikes from becoming a proper fourth wave is vaccination (which, even if cases continue to rise, can help prevent hospitalizations and deaths), increased surveillance, and a return to mitigation measures. Indeed, Los Angeles County on Sunday reinstituted mandatory mask-wearing in businesses and public areas, a major rollback after the U.S. Centers for Disease Control and Prevention said on May 13 that fully vaccinated individuals could shed their masks in many scenarios. Unless states can rapidly revive widespread and easily available testing, L.A. will be far from the last county to ask residents to mask up once again. from https://ift.tt/3iw50uK Check out https://takiaisfobia.blogspot.com/ On Monday, 51 Texas lawmakers boarded planes to Washington, D.C. The legislators, the bulk of the Texas House of Representatives Democratic delegation, had fled their state in hopes of stopping a vote on bills that would change the times and ways that citizens in the state may vote, as well as the experience Texans may have while casting a ballot. The Democrats say the proposed laws would come with the very real possibility of voter suppression and intimidation; one measure in question, for example, would allow untrained and armed poll watchers to stand close enough to voters to see how they vote. [time-brightcove not-tgx=”true”] On Saturday, that developing political story ran headlong into the realities of the ongoing pandemic, when three of the Texas Democrats reported testing positive for COVID-19. Read more: In Texas, Democrats Go All In to Fight Voting Restrictions All three lawmakers had been vaccinated, according to their caucus, as have most other members of the Texas House of Representatives. Among those who had tested positive Saturday were state Rep. Celia Israel, 57, a Democrat representing a district that includes Austin and nearby suburbs. The district, where people of color make up the majority of residents, reports one of the higher vaccination rates in the state. It’s made up mostly of Travis County, where 61.84% of residents 12 and over have, like their representative, been fully vaccinated. Statewide, about 59% of all Texas residents in that age range have been fully vaccinated. “Let this be a reminder that COVID-19 is still very much among us, with infection rates on the rise and more infectious variants spreading nationwide,” Israel said in a statement issued Saturday evening. “While I have fully complied with CDC guidelines and am fully vaccinated this will not 100% prevent infection. “Thankfully I am doing well and hope to get over the infection with mild symptoms. I am currently quarantining until I test negative. I urge anyone not vaccinated to do so as soon as possible to help stop the spread.” The Texas House Democratic Caucus did not identify the two other members of the delegation who have tested positive for the coronavirus. (I was alerted to Israel’s status because I was in masked but close contact with her while reporting this week.) COVID-19 cases have been on the rise in Texas, as in most states in the U.S., which experts have attributed to factors including the highly contagious Delta variant and the slowing rate of vaccinations. On Thursday, Austin officials tightened the city’s COVID-19 guidelines in response to an alarming spike in cases. Read more: Texas Was Already One of the Hardest States to Vote in. It May Get Even Harder Before the news of the positive tests, outlets like Fox News, as well as the lawmakers’ political opponents back home, had highlighted images of legislators aboard a charter flight from Texas to Washington, D.C., in which many appear not to have worn masks. While commercial airlines require all passengers to wear masks during flights, current CDC guidelines do not recommend them for those who have been fully vaccinated. Breakthrough COVID-19 cases are possible even after vaccination—as would be the case with any vaccine—but there is evidence that those cases may be less severe. An AP analysis found that about 99% of COVID-19 hospitalizations in the U.S. in May were among unvaccinated people. Israel also thanked her Republican and Democratic colleagues for the well wishes and concern some have expressed for her and for her partner, whom Israel had planned to marry Thursday on the floor of the Texas House of Representatives, before the delegation decided to flee the state. “Most importantly, I hope this instance highlights the sacrifices we’re willing to make for the cause of democracy,” the lawmaker said in her statement. “I would not change anything to protect the right to vote.” from https://ift.tt/3BdNbcc Check out https://takiaisfobia.blogspot.com/ |
Authorhttps://takiaisfobia.blogspot.com/ Archives
April 2023
Categories |
 RSS Feed
RSS Feed
